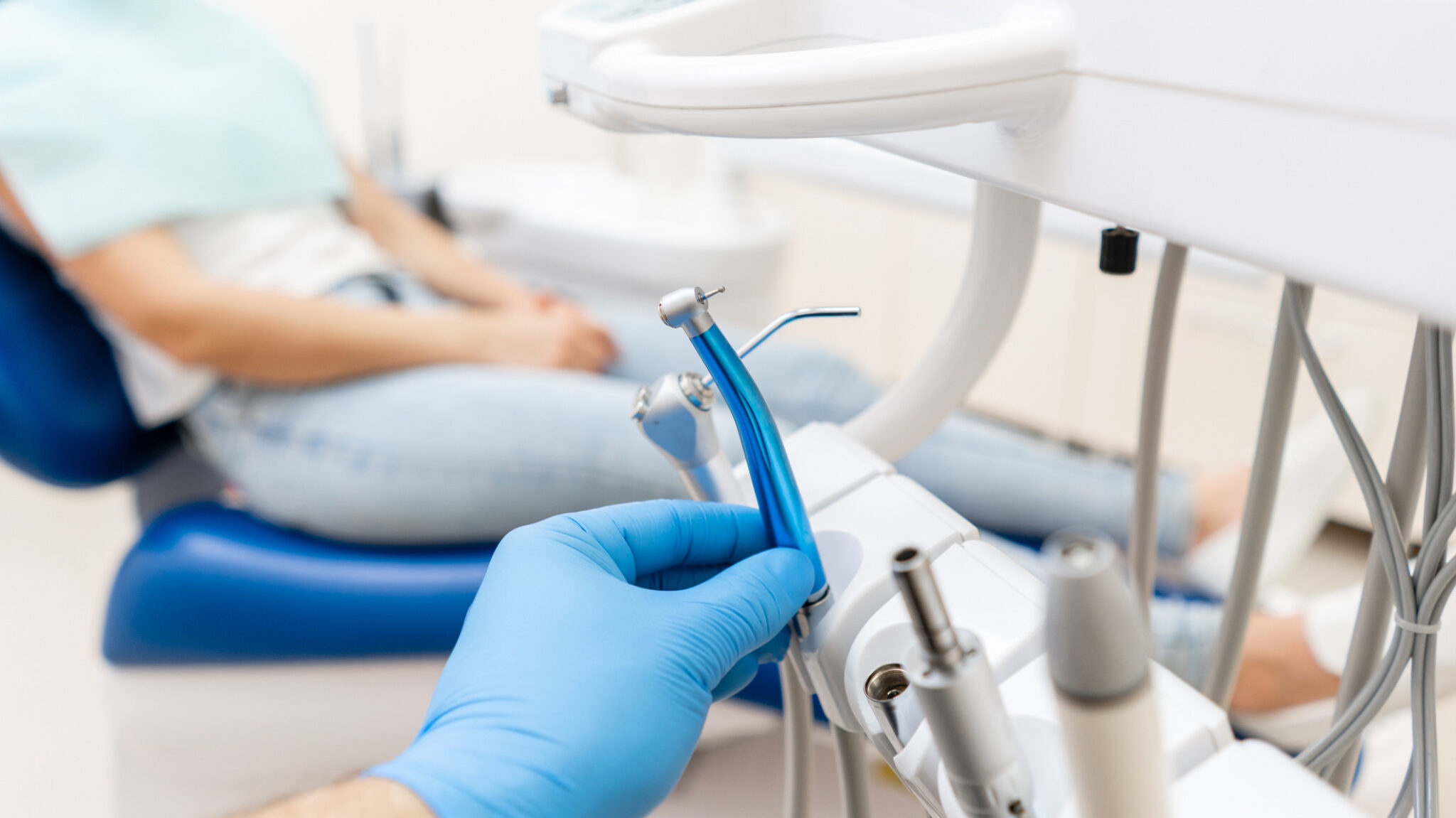
The Canadian Dental Care Plan (CDCP) is closing out 2025 — the year it completed its national rollout — with what the federal government is calling a major milestone.
By late November, nearly six million Canadians had enrolled in the program, according to Health Canada. More than 27,000 oral health providers are now participating, and roughly 60 per cent of approved CDCP members had received dental care as of Nov. 30.
Despite those headline numbers, ongoing challenges continue to affect both patients and providers.
Dentist sentiment remains mixed
A Dec. 3 survey by the Ontario Dental Association (ODA) suggests growing unease among dentists participating in the plan. While 67 per cent of respondents said they support the CDCP and 74 per cent believe it is improving access to dental care to a great or moderate extent, 46 per cent reported feeling less positive overall about their experience with the program.
One persistent source of tension is balance billing — and widespread misunderstanding among patients about what the CDCP actually covers.
“From day one, the Canadian Dental Care Plan was presented like medicare — as if patients wouldn’t have to pay anything — and that misunderstanding has never really been corrected,” said Bernard Dolansky, senior national partner and transition consultant at Tier Three Brokerage.
“Politicians have never clearly emphasized that the CDCP is a partial-payment plan, not free dental care. That has created unrealistic expectations from the start,” he said. “Dental offices that have been most successful with the CDCP are those that clearly and proactively inform patients about what is and is not covered.”
Under the program’s design, co-payments apply for households earning more than $70,000 annually, meaning care is not fully covered for all enrollees.
Urban–rural divide in balance billing
Dolansky said balance billing practices appear to differ sharply by geography.
“In urban centres, where competition for patients is high, some dentists may choose not to balance bill,” he said. “In contrast, in rural areas — including rural Ontario — balance billing is far less of an issue because patients don’t have the same level of choice. If they want care, they have to see the dentist who’s available.”
According to the ODA survey, about 80 per cent of dentists reported that they balance bill. However, Dolansky said claims data reviewed by the Canadian Dental Association (CDA) suggest the true figure may be significantly lower — possibly closer to 50 per cent.
“The truth is probably somewhere in the middle,” he said, adding that self-reported surveys can overstate certain behaviours. “When I ask dentists how many are not balance billing, no one puts up a hand. Statistically, that can’t be true.”
Related: The Canada Dental Care Plan: Missing pieces – A commentary on the national dental program
Related: The CDCP and data: You don’t improve it if you don’t measure it
De-insurance trends emerging
The ODA survey also flagged early signs of de-insurance behaviour following the CDCP rollout. While 53 per cent of dentists reported seeing little or no shift away from private insurance, nearly three in 10 said they had observed patients switching from private plans to the CDCP to a great or moderate extent. The reasons are still not clear yet but there were initial fears that the CDCP could possible erode private insurance.
The ODA also said the Canadian Life and Health Insurance Association has committed to providing data to help validate those observations and explore potential solutions.
Coordination with provincial programs improves
Coordination of benefits between the CDCP and provincial dental programs also appears to be increasing. Just over half of dentists (52 per cent) reported having patients who are coordinating benefits.
Sentiment on that process was mixed but trending neutral to positive, with 37 per cent of dentists describing their experience as neutral and 34 per cent reporting a positive experience.
Related: Changes, challenges, opportunities and the CDCP
Related: Health Canada pushes back on fears CDCP will erode private coverage
Pre-authorizations and denied claims
Administrative hurdles also remain a concern. The ODA survey found that about 85 per cent of dentists experience claim denials to a great or moderate extent, with many reporting processing times exceeding 21 days.
Patients requiring complex treatments — or care exceeding standard CDCP limits — must obtain pre-authorization through the plan’s administrator, Sun Life, which requires detailed treatment plans and diagnostic documentation such as X-rays.
Health Canada data released in July showed that roughly 50 per cent of complex-care claims were denied between Nov. 1, 2024, and June 20, 2025. However, as of mid-July, more than 80 per cent of pre-authorizations were being processed within seven days.
In response to requests for updated figures, Health Canada said that since the CDCP’s launch, more than 637,000 members have submitted nearly 2.2 million pre-authorization requests. Of those:
- More than 803,000 were approved
- Over 620,000 were denied due to incomplete or missing information (and may be resubmitted)
- Approximately 760,000 were denied for other reasons, including not meeting eligibility criteria, duplication or exceeded frequency limits
Related: Dental program improving, industry says, but misconceptions about ‘free’ care persist
Cost and long-term sustainability
The CDCP is one of the largest new social programs introduced by the federal government in decades. Budget 2023 allocated $13 billion over five years, with $4.4 billion in ongoing annual funding thereafter.
However, Health Canada has said administrative costs reached $472.9 million as of March 31, a figure that has drawn criticism from some opposition MPs.
When asked about the plan’s long-term sustainability, Mostafa Askari, chief economist at the Institute of Fiscal Studies and Democracy, said the CDCP cannot be evaluated in isolation.
“Its sustainability cannot be assessed separately from the fiscal sustainability of the federal government overall,” Askari said, noting that Ottawa’s long-term fiscal position is currently considered sustainable.
He said the plan’s success will ultimately be judged on two measures: how many Canadians actually receive care and whether oral health outcomes improve over time.
“This needs to be evaluated a few years after the program was first initiated,” Askari said. He added that it is difficult to predict whether the federal government will introduce other programs of similar scale.
Because funding for the CDCP is separate from federal health transfers to provinces and territories and drawn from general revenues, Askari said Ottawa’s new fiscal anchor — balancing the operational budget by 2028–29 — makes it unlikely the government will launch another program comparable in size in the near future.
In October, the B.C. government said improved access to dental care through the CDCP is also expected to ease pressure on the health-care system. Emergency-department visits for preventable dental conditions cost Canada’s health system more than $31 million in 2022–23, with B.C.’s share at $6.5 million.
Whether the CDCP ultimately reduces those costs, however, remains to be seen.