Note from editor
Oral Health is proud to introduce a brand-new series by Dr. Bruce Pynn and Dr. Hagen Klieb, featuring a curated collection of compelling cases. This series aims to raise awareness and deepen understanding of unique and unusual oral pathology.
How would you diagnose this case?
A healthy 49-year-old female was referred to the Oral and Maxillofacial Pathology service for evaluation of intensely painful gingival lesions, which were associated with bleeding and difficulty brushing. These symptoms began approximately six months ago without any clear precipitating event. Initially, she consulted her general dentist, who performed debridement and prescribed Peridex, but there was no improvement. She was apparently informed that the lesions were due to inadequate oral hygiene. Seeking a second opinion, the patient consulted another general dentist, who subsequently referred her to a periodontist, and from there, she was referred to the oral pathology service.
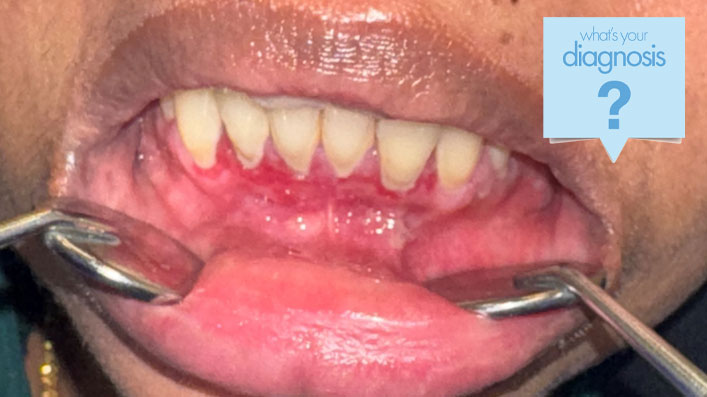
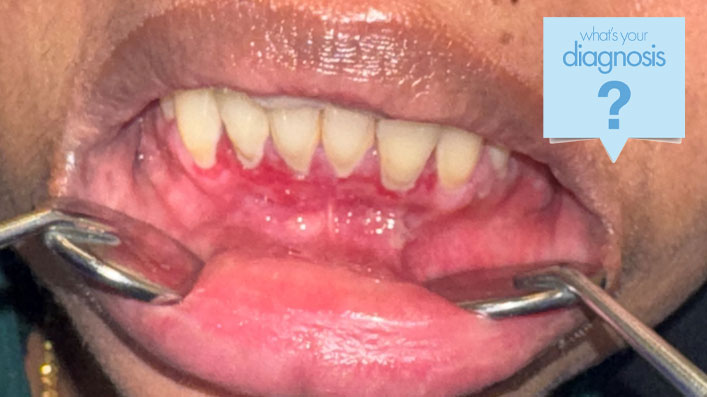
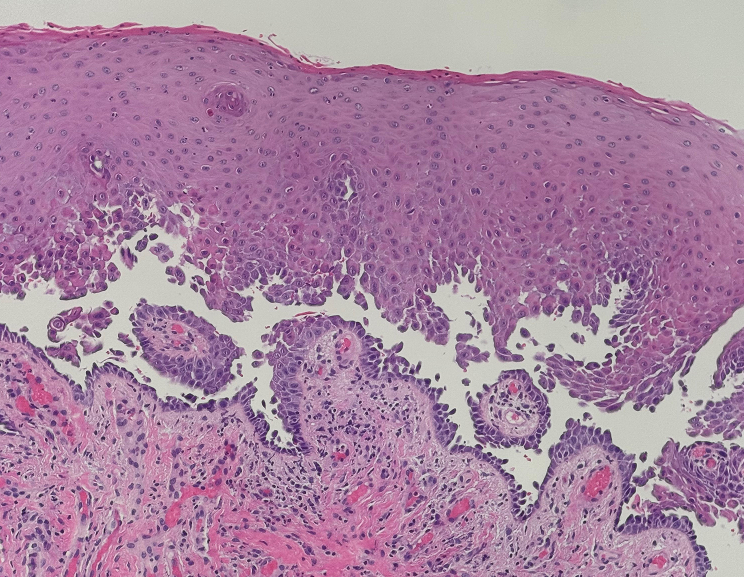
On examination, there was no cervical lymphadenopathy. Intraoral examination revealed diffusely erythematous and friable gingival tissues (see Fig. 1). There was light plaque accumulation. A gingival biopsy was obtained (see Fig. 2).
Fig. 1
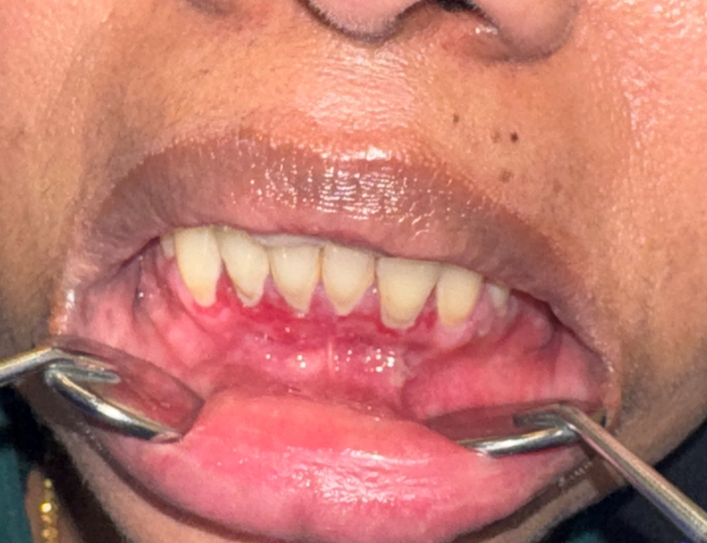
Fig. 2
Which of the following statements is most accurate based on the clinical presentation?
A. The histologic findings are consistent with nonspecific acute and chronic gingivitis, and the patient’s condition can likely be managed by improving oral hygiene.
B. The clinical presentation is indicative of a potentially life-threatening condition; systemic immunosuppressive therapy is likely required.
C. The presentation suggests ascorbic acid deficiency, requiring medical evaluation and dietary changes.
D. The patient’s condition is likely due to lichen planus, and a topical corticosteroid would be appropriate first line management.
If correct, you will be entered to win a $100 CAD Amazon gift card. **Contest end date: January 15th, 2026 at 11:59pm