Oral health professionals, dentists and hygienists, are in a unique position to recognize and report signs of abuse and neglect during their dental exams and procedures as it is estimated over 50% of injuries from child abuse occur on the head and neck. It is also important to learn the indicators of child abuse, to understand the legal obligations, to learn how to report suspected child abuse, to learn how to prep for possible future court testimony when lacking experience in testifying, and to learn how to document and write a report. A lack of knowledge and training of child abuse recognition is a barrier to reporting.1 Proper training has shown to increase interpersonal support for reporting.1
Jessica Shaw, RDH, co-author, has a passion for this subject, and her goal has always been to support dental hygienists as a teacher and mentor on child abuse recognition and reporting. She has professionally and personally experienced this in her workplace. Children are more likely to communicate abuse with a hygienist than with a dentist. The power of observation, looking for non-accidental trauma signs.
It was found that HCP’s who completed a minimum 10 hours of training reported identifying child abuse in a larger percentage of child abuse rather than those with no training.2 Educational sessions are the cornerstone of screening dissemination. Standardized educational programs and established screening protocols improve detection of child abuse and decrease bias.3 To learn to distinguish accidental and non-accidental trauma. Child abuse crosses all genders, cultures, and social status.
Dentists have a duty to report when there is a child in need of protection who is under the age of 16. If a child is 16 or 17, a dentist is permitted to report, but it is not mandatory. This arises from the Child, Youth and Family Services Act, 2017, section 125. Failure to report can result in a conviction with a fine of up to $5,000. It is mandatory for a dentist or hygienist to immediately report to their local Children’s Aid Society if that dentist “has reasonable grounds” to suspect concerns relating to abuse or neglect of a child. You can find the full list in the Act itself, but two common examples include: 1) the child has suffered (or is likely to suffer) physical or sexual abuse inflicted by their parent/guardian; and 2) the child requires treatment to cure, prevent or alleviate physical harm or suffering and the parent/guardian does not provide it. This applies to dentists and hygienists.
While a report can formally be made to the Children’s Aid Society, the dentist who is reporting should be prepared to answer for that report and explain the reasons behind it.1 I would strongly suggest thoroughly documenting your report and the basis for it at the time you are making it. A proper report includes: the description of the injury and anatomical location; is the injury likely or unlikely compatible with the mechanism of the injury as described by the caregiver. If the caregiver’s explanation of the injury is not compatible with the injury, then it should raise concerns for abuse and prompt further evaluation.
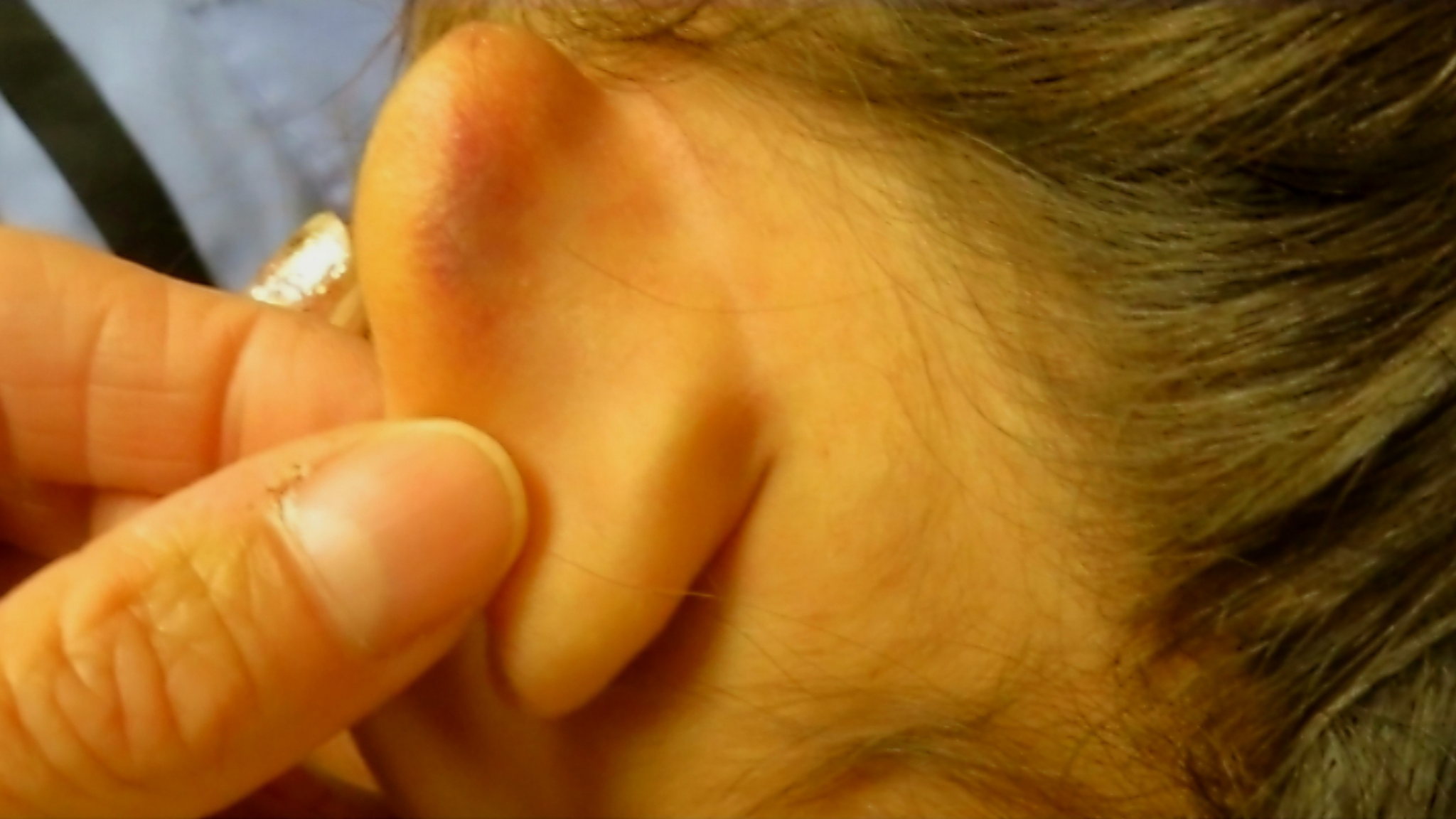
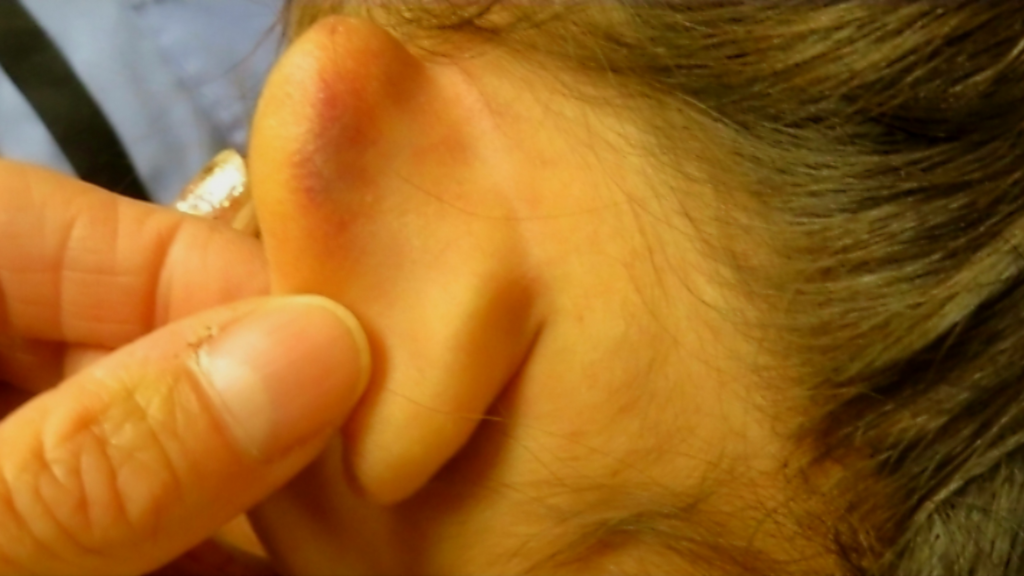
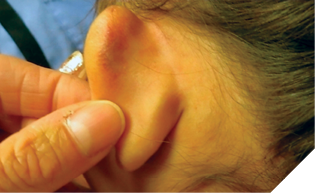
For example, there is bruising to the ear observed (Fig. 1). The caregiver’s explanation was that the 5-year-old female fell at soccer practice. The injury is unlikely compatible with the mechanism of a fall at soccer practice and this should raise concern for abuse. Prompt further evaluation should be done and a decision whether or not to refer to any medical sub-specialties. As an aside, if photographs are taken, a personal cell phone is not to be used as confidentiality and the chain of evidence custody would be broken. Sometimes caregivers make up false stories not consistent with the injury that we observe. Sometimes nice people tell lies.
Fig. 1
The only way to learn these proper recognition and reporting skill is via training. In California, child abuse recognition as mandatory training is offered for free. In New York state, the dental license body made it mandatory for dentists and hygienists to take the training, or else their license would not be renewed. In Pennsylvania, quote: “This course will fulfill the CE requirement for dentists and hygienists renewing a Pennsylvania dental license.”
John McIntyre, a lawyer who focuses on the healthcare profession, explained in a recent April 2025 OD article: “All the reporting obligations above have some form of protection from being sued if the dentist who reports does so in good faith, without malice, and/or with reasonable grounds for suspicion. However, if such a report does not meet those requirements, a lawsuit for the damages the individual experienced as a result of the report can proceed.
Additionally, we sometimes see individuals who were reported against in turn filing a complaint with the RCDSO about the report. This can result in a complaint investigation and review by the Inquiries, Complaints and Reports Committee, where the dentist will want to explain their decision to report and why it meets their obligations. A report that is not done in good faith or that doesn’t have reasonable grounds may result in remedial or disciplinary action.”4
An upset caregiver can also launch a civil lawsuit against the reporting healthcare professional who reports the suspicion of child abuse. What is your response going to be when your child abuse reporting is questioned? “Sorry, I had no training.”
It is important for the oral healthcare provider to distinguish age-appropriate, non-abusive injuries from suspicious injuries. Begin each appointment by performing a thorough intraoral and extraoral examination.
Extra-orally, signs of possible abuse, maltreatment, or neglect include: Physical marks such as bruising (varying degrees of healing), slap or finger marks, pinched ears, burns, lacerations, contusions, abrasions, welts, scars, scratches, broken bones, or dark rings around the eyes signaling lack of sleep and stress.5 If the child is wearing more clothing than what is weather appropriate, be sure to evaluate the skin of the neck, arms, and legs. You should be able to evaluate the arms with ease by taking the patient’s blood pressure on the forearm instead of a wrist cuff. When performing an extraoral examination, be sure to have the patient lean forward so you can see the back of the neck and slightly down the collar of their shirt looking for any unusual marks. Ligature marks on the neck, wrist, ankles that can be induced from restraints (rope, shoelace, muzzle, belt, rope, wire).6 Bitemarks are often seen in cases of physical child abuse. A bitemark is a patterned injury. There many kinds of patterned injuries: hand slap halo to facial cheeks, knuckle marks, whipped with phone cord or belt or coat hanger or spoon/ladle. This list of patterned injury sources is by no way all inclusive. Cigarette burn marks and cigarette lighter burn marks are also sadistic patterned injuries. Not only studying bruising, but also burn injuries that are either accidental or non-accidental.
The child may appear withdrawn, fidgety, or anxious.7 They may avoid eye contact and not answer questions or engage in conversation. The most common child abuse injuries of the head and neck are abrasions, lacerations, hematomas, and cranial vault and maxillofacial fractures.5 Trauma inflicted to the skull often results in damage to hard and soft tissues of the mouth.
Intraorally, signs of possible abuse, maltreatment, or neglect include: Bruising, abrasions, or lacerations occur on the tongue, lips, oral mucosa, hard and soft palate, gingiva, alveolar mucosa, and frenum.5,6 Unexplained erythema, ecchymosis (bruising), and/or petechiae of the palate, especially at the junction of the soft and hard palate, may be evidence of forced oral sex, but discretion is required as soft palate bruising could also be caused by trauma from a lollypop or a popsicle.8 Tooth fracture, dislocation, subluxation, or avulsion. The anterior teeth are the most commonly affected.5,6 Torn frenum and any signs of sexually transmitted disease such as human papilloma virus, herpes, unusual lesions for the child’s age, ulcers, erythematous vesicles, or perioral lesions. Gonorrhea is one of the most common sexually transmitted diseases found in children of sexual abuse.5,6 Detection of semen in the oral cavity is possible for several days after exposure so reporting any suspicion of sexual abuse requires an immediate referral to a medical provider for swabbing.8 Gags applied in the mouth may leave bruises, lichenification (secondary skin lesion with hyperpigmentation, thickening of the skin, and exaggerated skin lines), or scarring in the corners of the mouth.8 Lichenification refers to areas of hard, thickened skin.
In summary, documentation is so important. Again, if an injury is found, obtain its origin and history from both the caregiver and the child and determine if the story aligns with your observations. Evaluate the behavior of the child and caregiver, and document all findings. It is crucial that injuries are documented at the time of appointment and as thoroughly as possible because evidence can be lost over time through healing processes. Record the date, time, and location of the examination. Record who was with the child at the time of the appointment. Record the caregiver’s and child’s stories of how the injuries occurred. Take photographs of the injuries showing the anatomical location and close-up photographs with a ruler—preferably the recommended American Board of Forensic Odontology No. 2 scale. Take one photograph with the scale and one without. The camera must be aligned perpendicular to the No. 2 scale.9
Dentists and hygienists serve an important role in recognition and reporting of child abuse. It is recommended that educational programs be formal, structured, and mandatory with a focus on dental-specific screening protocols, child physical abuse detection, and interview techniques for discussing suspected abuse with parents/caregiver. Studying of multiple pediatric trauma cases need to be studied as a part of training. Over time, these integrated screening tools become a part of routine day-to-day dental clinical practice in Ontario and Canada. 
Oral Health welcomes this original article.
References
- McTavish, J.R., Kimber, M., Devries, K., Colombini, M., MacGregor, J.C.D., Wathen, C.N., Agarwal, A., & MacMillan, H.L. (2017). Mandated reporters’ experiences with reporting child maltreatment: A metasynthesis of qualitative studies. BMJ Open, 7, e013942
- King, G., Reece, R., Bendel, R., & Patel, V. (1998). The effects of sociodemographic variables, training, and attitudes on the lifetime reporting practices of mandated reporters. Child Maltreatment, 3, 3, 276-283.
- Carson SM. Implementation of a comprehensive program to improve child physical abuse screening and detection in the emergency department. J Emerg Nurs. 2018 May 17; 1-6.
- McIntyre, John. OD Journal, Apr 2025. See Something, Say Something: A Dentist’s Duty to Report. Pg 30-32
- Nagarajan, S.K., (2018, January-April). Craniofacial and oral manifestation of child abuse: A dental surgeon’s guide. Journal of Forensic Dental Sciences, 10, 1, 5-7.
- Costacurta, M., Benavoli, D., Arcudi, G., & Docimo, R. (2015). Oral and dental signs of child abuse and neglect. Oral & Implantology (Rome), 8, 68-73.
- Rayman, S., Dincer, E., & Almas, K. (2013, June-July). Child abuse: Concerns for oral health practitioners. New York State Dental Journal, 30-34
- American Academy of Pediatrics. (1999, August). Oral and dental aspects of child abuse and neglect. Pediatrics, 104, 2, 348-350.
- Adserias-Garriga, J. (2019). A review of forensic analysis of dental and maxillofacial skeletal trauma. Forensic Science International, 299, 80- 88.
About the authors

James Frizzell, BSc, DDS (U of T). Dental Forensics 2019 (McGill). Identification of Abusive Pediatric Bruise Injuries course (Sick Kids Hosp Toronto 2025). Frequent speaker for Academy of Forensic Nursing. He can be reached at jamesfrizzell983@gmail.com.

Jessica Shaw, RDH (Niagara College). Co-author. Teacher. Mentor to hygienist colleagues on Child Abuse Recognition & Reporting. She can be reached at jessica.shaw33@hotmail.com