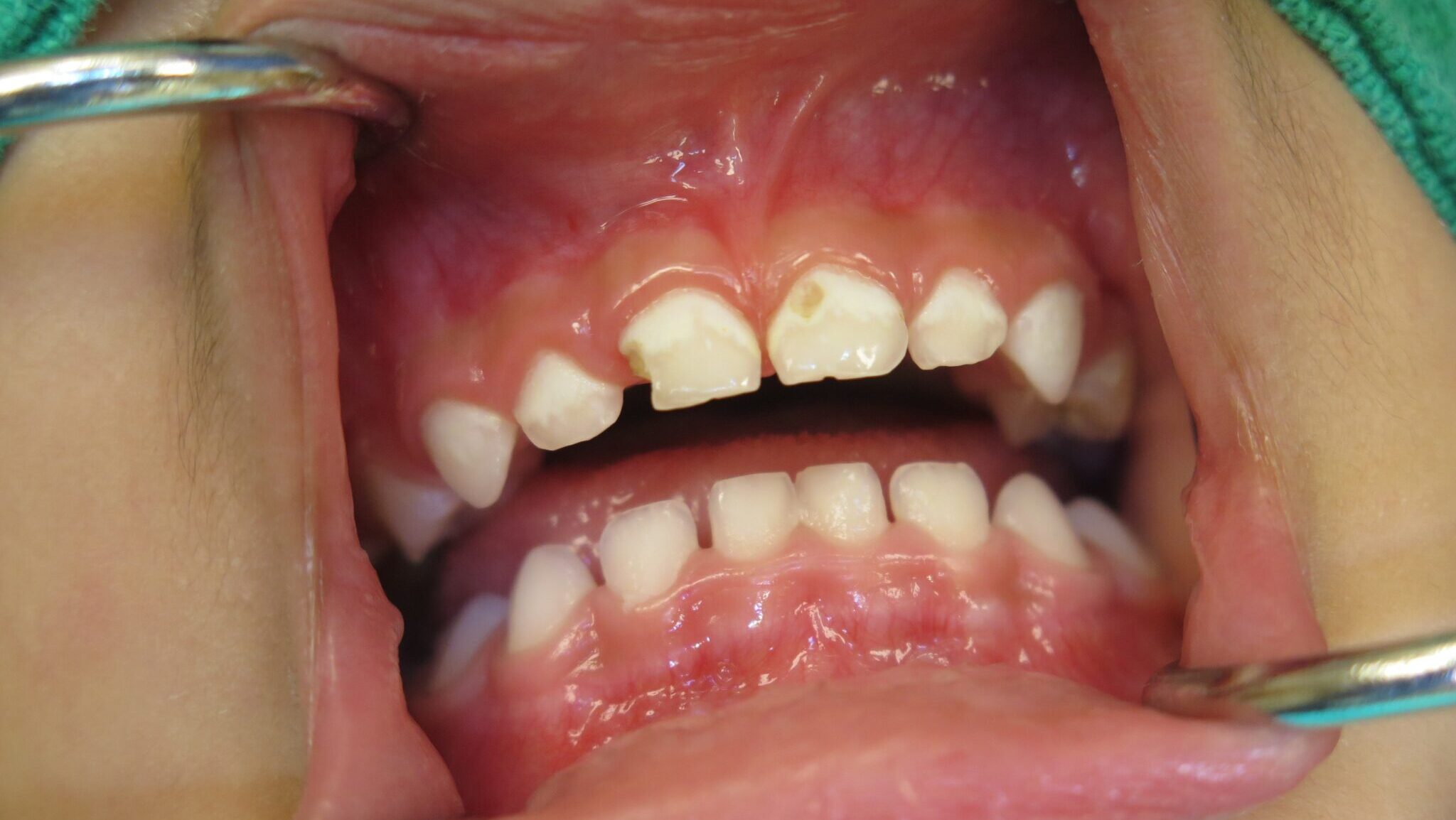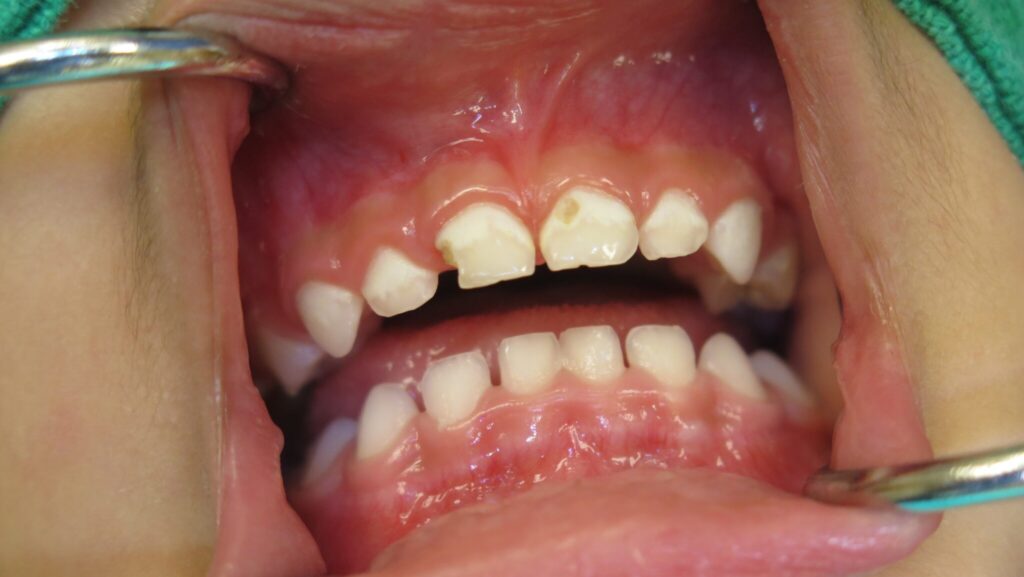
Early Childhood Caries (ECC) or Baby Bottle Syndrome (BBS) is a rampant form of tooth decay that destroys the newly erupted primary teeth very quickly. The tooth decay progresses at an astonishingly quick rate and will occur even before the tooth fully erupts. ECC is different from normally occurring tooth decay in that it appears at a very early age, usually before the age of 2, and involves mostly the maxillary incisors. In later stages it can involve upper first maxillary molars and the lower molars as well if the child is still bottle feeding after two-and-a-half years of age. The mandibular incisors are rarely involved. The decay progresses very rapidly and can destroy the whole erupted tooth in a number of months (Fig. 1). Typical forms of caries are usually not as aggressive and usually start in the pits and fissures or interproximally on the molars. Typical dental caries do not usually occur at a very early age, for example below the age of 2 years.
Fig. 1
ECC occurs in young children who are fed nocturnally on demand with a fermentable carbohydrate, typically milk. Night-time feeding, whether by bottle or breast feeding, before the eruption of the maxillary incisors is not problematic. Taking a baby bottle during the day, no matter how frequently, does not seem to cause this problem. Feeding a child with a baby bottle before going to sleep is also not problematic. This may be due to the self-cleaning action of the salivary flow during the daytime. With EEC there is reduced salivary flow at night, so the substates are not washed away, but stay on the surface of the teeth. The substances in the bottle also have an effect. The more carbohydrates, the more virulent the decay. A sweetened drink such as apple juice is worse than milk, which is worse than natural breast milk. The substate stays on the tooth surface all night and is replenished regularly by repeated feedings. Why are the maxillary incisors so severely decayed, while the mandibular incisors are virtually immune with ECC? The mandibular incisors are largely unaffected due to the position of the child’s tongue while feeding. As the child sucks on the bottle, the tongue covers and protects the mandibular incisors. The primary incisors when newly erupted are not yet fully calcified and may explain why the decay progresses so quickly. The maxillary first molars may be involved but the maxillary cuspids are usually not involved as they erupt later. The second molars of both jaws may be involved if the child is still night feeding after they erupt. It may be difficult to determine if the teeth are painful, especially if the child is colicky. A good sign that the teeth are painful is that the child is not biting with their front teeth, and yet they have no other teeth. You should note that if the decay of the teeth is extensive and the teeth are infected, with draining fistulas, there may not be any pain (Fig. 1). The treatment depends at what stage you catch the disease. In the very early stages, before cavitation or incipient lesion stages, you can institute preventive measures, such as good oral hygiene with a fluoridated toothpaste and regular topical fluoride applications. However, for these recommendations to work, the night feeding must stop. Incipient lesions will appear as white frosty areas of decalcification lesions on the buccal surfaces of the teeth (Fig. 2).
Fig. 2
One treatment modality that is effective with incipient decay of this nature is professionally applied Silver Diamine Fluoride (SDF). SDF can help to arrest or slow down the progression of the lesions. One side effect that parents need to be warned about is black staining. It is important to discuss this before the treatment because it may introduce a real esthetic concern. If the teeth are extensively decayed, and with draining fistulas, the only treatment may be extraction of effected teeth (Fig. 3). If the teeth have cavitated lesions, then restorative options can be given. This usually involves an extensive treatment plan with sedation, typically a general anaesthetic (GA). For the very young, treatment should only be caried out at a hospital for safety reasons. Restoring the teeth will give the child a full functioning dentition and let the jaws develop properly. The ideal restoration for gross decay from ECC is a full coverage crown. The best being zirconium crowns (Fig. 4) or stainless steel with plastic white facings. Since the work is done under GA, the best and strongest treatment options should be considered. This will help to prevent further treatments due to failure that could involve subsequent sedations.
Fig. 3
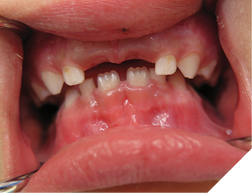
Fig. 4
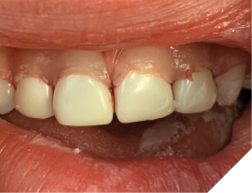
The practitioner must be careful in diagnosing pulp exposures when preparing these teeth. Primary teeth have relatively larger pulp chambers, and pulp therapy will likely be required in these cases. Even if you have a draining fistula and the root is fully developed, a root canal procedure can be caried out. It goes without saying, you should not initiate any restorative treatment until the night feeding is terminated. Although even extensively destroyed teeth can be restored by a skilled dentist, sometimes extractions are the only option. What happens if you do not treat severe rampant decay? There are many reasons why you cannot do treatment. It may be the parents refusing to put their young child under a GA due to the risks associated, or parents being reluctant for their child to have a painful treatment experience, if done without a GA. There may not be any nearby facilities to carry out the procedure safely. If not treated, ECC will progress, even if the child stops night feeding. The decay will lead to periapical infections of the jaws that can harm the developing dentition. There may not be any pain if the fistulas is draining. Over time they may blow up to a painful cellulitis that will require emergency care at an inconvenient time or place.
When stopping the night feeding, check to make sure the child is thriving. If you are not sure, consult with the treating physician before stopping night feeding. When you are going to stop night feeding, it needs to be abrupt and fully stopped, not phased out. Only water can be given at night. This will be difficult, and I recommend stopping night feeding on a weekend as parents will experience 1-2 sleepless nights. Remember to console the mother, as there is often guilt attached. Reinforce that it is for the child’s benefit, even though it is difficult to carry out. Once night feeding has been stopped, do not re-institute under any circumstances.
What is the differential diagnosis of ECC and other types of severe tooth decay? Decay due to a diet high in carbohydrates and poor oral hygiene starts at a much later date, when the child is 3-4 years of age. The decay is mainly in pits and fissures of the molars, or interproximal in the maxillary incisors, rarely labial, or lingual. If the molars are more severely decayed than the incisors, there is something else at work. Most likely the diagnosis is hypoplastic/hypocalcified teeth, which have a cloudy appearance with a yellow or brownish colour. You may see a case of hypoplastic teeth combined with night feeding, in which case all the teeth will be severely decayed except the mandibular incisors.
Once the restorative treatment is complete, I recommend an immediate post op assessment be carried out 3-4 days post-surgery. I spend this time going over the treatment, what to expect in the next couple of days, and make sure the night feeding is fully terminated. A hygiene program to prevent any recurrence can be set in place at this visit as well. I will see the child 1 month post op to check and make sure oral hygiene is up to standard. Often, it is not, and the child has a severe gingivitis, as the parents do not want to hurt the child and brush too gently to be effective. Even if hygiene is good, I see the child again 3 months post op for an evaluation. If oral hygiene is good, then I will recommend placing them on a 6-month recall. If oral hygiene is poor, a 3-month program is set up until oral hygiene is up to standards. If the treatment is done by specialty office, the primary dentist should be notified of the completion of the treatment, and let them know I will be doing recalls and follow up for two years, to monitor and adjust any treatment. After that, they will be referred back to their office. Recurrences of treatment are more common with patients who do not return or go back to their dentist immediately. In 1-2 years, they are back for a retreatment, under GA, due to the extent of renewed decay. The patients who stick to a strict preventive regime are far less likely to return with new decay.
Early prevention involves speaking to pregnant mothers and educating them on the prevention of ECC. Parents can then be informed that the first appointment to the dentist should be when the first tooth erupts and no later than 1 year of age. Another excellent way to get information out to young parents is at pre-natal classes. You can do lectures at daycare centres and give lectures to providers. However, giving information is not enough. It is a good idea to set up an appointment at 6-months-of-age to help parents manage. So do not lecture and scold but reassure the parent and give what help you can. Even extensive treatment has long-term potential problems. Early extractions can cause problems in jaw development. Early dental infections can affect the developing immune system. And even the use of antibiotics can affect the microbiome in unforeseen ways. Thus, prevention is GOLDEN. 
Oral Health welcomes this original article.
About the author

Dr. Jack Maltz is a pediatric dentist providing dental care to children in Brampton for over 40 years. Dr. Maltz is the former head of the OSPD and the Head of the Brampton Civic Hospital Department of Dentistry. Dr. Maltz can be reached at Drjdentistry5@gmail.com.