Abstract
Inappropriate use of lasers in frenotomy can lead to serious complications in patients with ankyloglossia (tongue-tie), a condition that restricts tongue mobility and affects functions like breastfeeding, swallowing, speech, and facial development. While laser frenotomies have gained popularity, improper technique and insufficient training can result in significant postoperative complications. These include hemorrhage, airway obstruction, scarring, salivary ductal injury, and functional impairments, including and not limited to compromised speech, mastication, and swallowing. In this case series, we discuss the complications of laser frenotomies performed on infants, adolescents, and adults. Each case outlines challenges such as uncontrolled bleeding, recurrent swellings, reduced tongue mobility, salivary duct obstruction, speech impairments, compromised mastication and permanent disability. Through these cases, we highlight the need for proper training, improved education, mentorship, interdisciplinary collaboration, and careful patient selection when performing a frenotomy in addition to the manufacturers demonstrating due diligence with respect to competent use of their equipment.
Ankyloglossia, or tongue tie, is a condition where the lingual frenum, the tissue connecting the tongue to the floor of the mouth, is abnormally short thereby limiting tongue mobility.1 This restriction originates during embryologic development. By the fourth week of gestation, the tongue begins forming as the tuberculum impar and lateral lingual buds from the first pharyngeal arch merge to create the anterior two-thirds of the tongue.2 Over the next three weeks, the lingual frenum helps guide the tongue’s anterior growth. Normally, the frenum then undergoes cellular apoptosis, allowing the tongue to separate from the floor of the mouth. However, incomplete separation results in a restrictive frenum, commonly referred to as a tongue tie.3,4
The clinical diagnosis of tongue tie typically begins in neonates and infants, often due to difficulties with breastfeeding, though not all infants/neonates with tongue tie experience such issues.5-8 Breastfeeding may be impacted during both the latch and suckling phases. For a normal latch, the tongue must extend anteriorly past the mandible and rest below the mother’s nipple and breast.9-11 Effective suckling requires the tongue to elevate along the entire palate to generate sufficient suction for milk extraction.9-12 A tongue tie that restricts anterior tongue mobility can prevent proper tongue extension for latching, while a tongue tie that limits mid-tongue elevation can hinder the creation of enough suction/vacuum for appropriate suckling.9,10,13,14 In either situation, infants may present with symptoms such as poor latching, weak suckling, tiredness, extended feeding times, frequent feeding, reflux, poor milk transfer, and inadequate weight gain; for mothers, symptoms may include nipple pain, mastitis, poor milk transfer, low milk supply, tiredness, and frustration.9,10,14-31 When breastfeeding difficulties arise, evaluation by a lactation specialist or an appropriately trained healthcare professional is recommended to confirm the presence of tongue tie and assess its impact.5,6,15,32-34 Non-surgical therapies are often the first line of treatment; however, if the tongue tie is determined to affect breastfeeding, a surgical release may improve outcomes with proper aftercare and professional support.7,27,29,32,35-38
A tongue tie may also impact swallowing after infancy. Tongue ties can limit tongue extension in the transition from feeding to swallowing and result in poor tongue-jaw dissociation resulting in dysphagia.39-45 Restrictions to tongue movement can impair mastication and lateralization of the bolus, causing greater bolus spread.40,46,47 This can lead to poor bolus organization, with residue left in the vestibules, on the cheeks, or on the tooth surfaces.48 The inability to move the tongue freely, combined with poor tongue-jaw dissociation, can also make it difficult to recognize and clear residue from these areas.46 Additionally, tongue tie may restrict mid-tongue elevation, impairing the ability to generate the necessary pressure and suction during the oral phase of swallowing to propel the bolus into the pharynx.40,44,47,49 As a result, compensatory strategies may develop during bolus formation to aid in swallowing, potentially leaving residue on the soft palate or the dorsum of the tongue.46,47,49
Residual infantile swallowing patterns associated with tongue tie may also lead to compensations such as anterior or posterior tongue thrusting to provide sufficient tongue pressure during bolus transfer from the oral to the pharyngeal phase.40,50,51 Poor tongue-jaw dissociation can further result in reduced tongue muscle tone and endurance, prompting long-term compensatory muscle recruitment from the lips, cheeks, jaw, and neck during swallowing.48,52,53 This may manifest as food aversions, texture sensitivities, and difficulties in transitioning from the oral to the pharyngeal phase of swallowing.42,43 Therefore, children and adults with feeding difficulties should be evaluated for tongue tie as part of an assessment by feeding therapists.5,42 Collaboration with feeding therapists for proper diagnosis and therapy is essential, as neuromuscular retraining both before and after surgical release of the tongue tie is crucial to maximize beneficial outcomes from surgery.5,41-43
A tongue tie can adversely impact speech, especially when it leads to poor tongue-jaw dissociation with significant muscular compensations.50,54-62 A tongue tie restricting anterior movement can limit tongue tip elevation leading to speech sound distortions and/or sound substitutions.55,63-71 Difficulty elevating the tongue tip to or near the incisive papilla often results in tongue tip depression with compensatory use of the tongue blade, producing a wider airflow column during speech sound production.55,65-72 When the tongue tie causes medial restriction and limits mid-tongue elevation, the lateral borders of the tongue may also fail to elevate during the production of lingual alveolar and palatal sounds.41,64-66,71 As compensation, the tongue’s center elevates, which can result in lateral sound distortions.41,65,66,71,72 Additionally, the tongue tie elevates the mandible, leading to overuse of jaw stabilization muscles over time.48,53,54 This can display as patients reporting generalized mouth and/or jaw muscle fatigue and/or unclear speech progressively worsening with extended use.52,73 Children and adults with speech concerns related to tongue tie should be evaluated by a speech-language pathologist experienced in orofacial myofunctional disorders for an accurate diagnosis.5,54,62,68,73-80 As previously mentioned with feeding therapists, coordinated therapy with a speech-language pathologist is crucial, as neuromuscular retraining is often necessary both before and after surgical release to maximize the beneficial surgical outcomes.5,59,73,77,78,81-84
The tongue plays a crucial role in facial development, occlusion, and maintaining airway patency.4,48,85-89 Restrictions in tongue mobility are linked to various dental malocclusions, including dental crowding, Class II and Class III malocclusions, loss of maxillary inter-canine space, anterior open bite, increased spacing of mandibular incisors, and gingival recession and other periodontal issues.4,48,50,89-98 A tongue tie has also been associated with maxillary hypoplasia and soft palate elongation.88,95,96 In some cases, tongue tie revision with appropriate orofacial myofunctional therapy has been shown to help improve existing malocclusion without orthodontic intervention.95,99 Additionally, restrictions in tongue movement are correlated with changes in airway patency, as the collapse of the tongue base into the oropharynx significantly contributes to airway obstruction in obstructive sleep apnea.100-103 Tongue tie has been correlated with a higher risk for obstructive sleep apnea.104-109 Surgical release of the tongue tie, when coordinated with appropriate orofacial myofunctional therapy, has demonstrated improvements in snoring and obstructive sleep apnea symptoms.110-114 Tongue tie release for the purposes of correcting malocclusion should never be undertaken without appropriate interdisciplinary collaboration including with an orthodontist and orofacial myofunctional therapist. Similarly, release for improving airway stability in obstructive sleep apnea should only be undertaken with appropriate collaboration with sleep physicians and orofacial myofunctional therapists.111
The prevalence of tongue tie varies widely, reaching up to 16% in specific populations, with a higher incidence in males compared to females.4,21,22,29,39,48,50,115-124 While complications from tongue tie release are rare, there are notable surgical risks associated with the procedure. Over the last decade there has been a ten-fold increase of frenoplasties/frrenotomies completed in North America.46 With the recent increase in dentists providing tongue tie surgical releases, review of potential complications from tongue tie release is prudent.125-134 The purchase of new tools and technology does not replace the need for appropriate clinical training, diagnosis of the functional problem and sound surgical technique. This case series reviews major complications associated with inappropriate surgical release of tongue ties. We aim to emphasize the importance of appropriate training, diagnosis and collaboration for tongue tie management.
Table 1: Summary of patient demographics, surgical details, complications, revisions and outcomes.
| Case Number | Age | Gender | Surgical Tool | Post-op Complications | Time to Complication | Number of Revisions | Procedures performed | Outcome After Revisions | Permanent issues |
| 1 | 10 Days | Female | Diode Laser | Uncontrolled bleeding risk, hypovolemic shock | Immediate | 0 | None | Encouraged monitoring, scar tissue massage | Lingual scarring |
| 2 | 14 Years | Male | Diode Laser | Recurrent swelling, salivary duct obstruction | Within 6 months | 1 | Z-Plasty, Wharton’s duct recanalization | Improved salivary flow, mild scarring | Recurrent mild salivary obstruction |
| 3 | 13 Years | Male | Diode Laser | Extensive hematoma, airway encroachment | Immediate | 2 | Extensive debridement, Z-Plasty | Improved mobility, mild scarring | Asymmetric tongue function |
| 4 | 31 Years | Female | Diode Laser | Infection, paresthesia, dysarthria, dysphagia | 5 days post-op | 3 | Multiple Z-Plasties, scar debridement | Improved swallowing, mild articulation gain | Lingual paresthesia, dysphagia, dysarthria |
Case 1
A ten-day-old female neonate presented to a general dental practice for a lingual frenoplasty. The parents reported no difficulties with breastfeeding, no pain or discomfort during latching, and had no concerns regarding feeding duration, gas, or reflux. The procedure was performed by a general dentist using an Er:YAG laser. The patient and family were discharged with no bleeding at the surgical site. Once the family arrived at home bleeding started in the floor of the mouth. Upon reaching the after-hours contact for the general dental office, they were provided with instructions to apply pressure with a moist tea bag to stop bleeding at the surgical site. Unable to control the bleeding, the parents took the infant to the hospital emergency room. Emergency room physicians noted extensive bleeding from three vessels, requiring approximately 30 minutes to achieve hemostasis before closing the large open lingual surgical site. The extent of the bleeding was deemed life-threatening, posing a potential risk for hypovolemic shock.
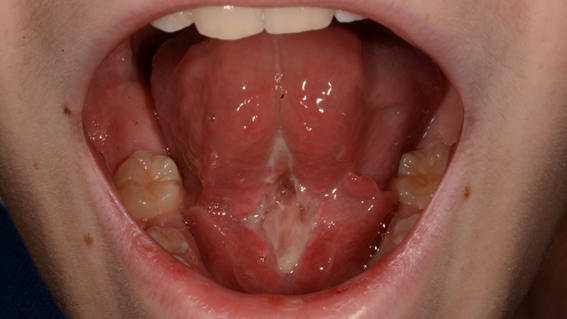
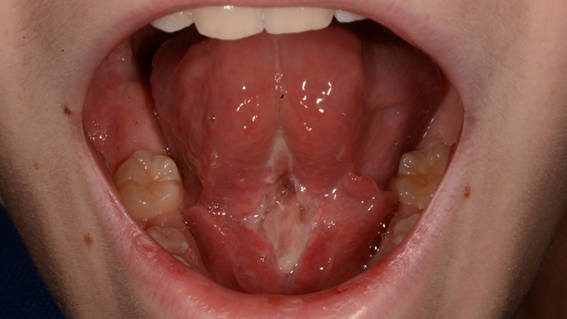
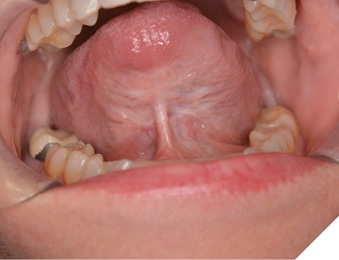
Two months later, a postsurgical evaluation and second opinion were conducted by an oral and maxillofacial surgeon. The examination revealed significant scarring along the floor of the mouth and the ventral surface of the tongue, along with grade 3 ankyloglossia and limited anterior tongue mobility (Fig. 1). Recommendations included home physiotherapy for scar tissue massage and manipulation. Since the infant’s mother reported no difficulties with breastfeeding, immediate surgical intervention was not advised. The mother was encouraged to seek evaluation by a speech-language pathologist and to return for re-assessment when the infant turned two.
Fig. 1
Case 2
A fourteen-year-old male presented to a general dental practice for a lingual frenoplasty. The frenectomy had been completed by a diode laser without primary closure and the surgical site left open to heal by secondary intention. Post-surgery, the patient reported extensive bleeding and extreme pain. After initial wound healing, he reported feeling a recurrent swelling under the right side of his tongue while eating, which did not resolve over a six-month period. The patient sought a second opinion from his physician, who referred him to an oral and maxillofacial surgeon for further evaluation.
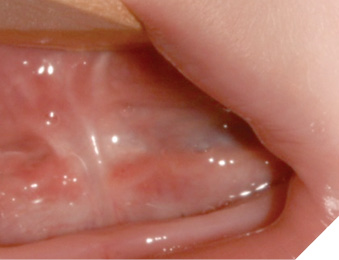
Clinical examination demonstrated extensive ankyloglossia, secondary to scar, and obliteration of the right Wharton’s duct of the submandibular gland, while normal flow from the left Wharton’s duct was present. Extensive scar tissue was noted in the area with no clinical evidence of a Wharton’ duct. Cone beam CT scans showed no evidence of sialolithiasis in either submandibular gland. The patient was scheduled for revision of the right Wharton’s duct using a cannula stent, along with a revision frenoplasty with Z-plasty.
Revision surgery was performed eight months after the initial frenectomy and involved extensive debridement of the floor of the mouth and lingual tongue, a lingual Z-plasty, and recanalization of the right Wharton’s duct. Due to the extent of scar tissue, submucosal dissection was necessary to locate the duct for successful recanalization. Post-surgical evaluation noted improved tongue range of motion, reduced recurrent swelling of the right submandibular gland, and mild salivary flow from the right Wharton’s duct. At the one-year follow-up, there was a noted mild improvement in salivary flow from the right Wharton’s duct. Continued regular monitoring was scheduled to evaluate for further improvement and determine if additional surgical intervention would be necessary.
Case 3
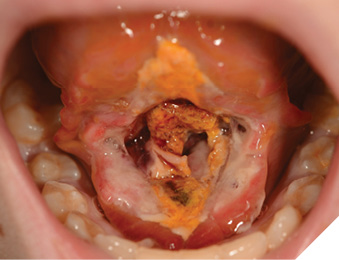
A 13-year-old male presented to the hospital emergency room with an extensive floor of mouth hematoma that was encroaching on his airway, following a frenectomy performed with a diode laser earlier that day. Pediatric otolaryngology specialists brought the patient to the operating room, where an emergent airway intubation was performed under general anesthesia. Sutures along the floor of the mouth and ventral tongue were removed, the hematoma was debrided, and active bleeding sites were cauterized. The wound was packed with FlosealTM hemostatic matrix and SurgicelTM (resorbable oxidized cellulose material); due to the size of the wound, primary closure was not attempted after achieving hemostasis (Fig. 2). Prior to discharge, the patient tolerated clear fluids but experienced difficulty eating solid foods. He was discharged two days post-surgery in stable condition.
Fig. 2
A follow-up evaluation with an oral and maxillofacial surgeon was arranged for 10 days after discharge. During this visit, complete dehiscence of the sublingual area with exposure of the genioglossus muscles was noted (Fig. 3). Postoperative oral hygiene practices were reviewed. Further evaluation one week later showed extensive submucosal scarring across the entire floor of the mouth and the base of the tongue, leading to asymmetric tongue function. The patient also displayed speech impairment, with his mother noting that his speech sounded “awkward and funny.” Tongue exercises were recommended, and a re-evaluation was scheduled for three months later.
Fig. 3
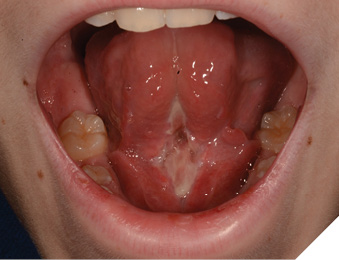
At the three-month follow-up, significant scar tissue was noted along the floor of the mouth, base of the tongue, and along the anterior mid-tongue, severely restricting tongue movement (Fig. 4). The patient was unable to reach the tip of his tongue to his palate, reported pain on tongue protrusion, and demonstrated considerable speech impairment. Given the extent of the scar tissue and tongue restriction, the patient was referred to a cleft lip and palate clinic for speech therapy, with plans for surgical revision and scar tissue removal afterwards. Revision surgery was completed 12 months later and included extensive debridement of the floor of the mouth and lingual tongue, and lingual and maxillary labial frenoplasty with Z-plasty. Post-surgical evaluation noted improved tongue range of motion and relatively normal tongue function, with the patient’s mother stating he was “doing so much better.” At the three-month post-surgical follow-up, normal tongue function was observed, with only mild scarring near the lingual frenum. The patient was subsequently discharged from specialist care.
Fig. 4
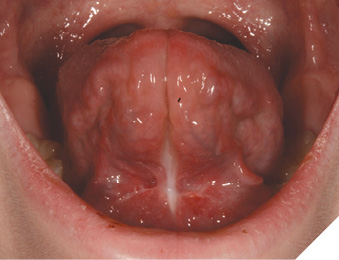
Case 4
A 31-year-old female presented to a general dental clinic for a frenectomy. The patient had no history of dysphagia, articulation difficulties, or sleep apnea, but the procedure was recommended by the dentist due to measured limitations in tongue mobility. The frenectomy was completed with a diode laser, and the surgical site was left open to heal by secondary intention. During a two-week postsurgical follow-up, the patient exhibited significantly reduced tongue function. A revision surgery was conducted by the same dentist approximately three weeks later, using the same technique. The patient was also prescribed Tantum Rinse, Peridex Rinse, Ibuprofen, and Toradol. Within a week the patient developed a fever of 40°C, throat and ear pain, and difficulty swallowing. The patient was advised by the dentist to go to the emergency room and request intravenous antibiotics.
The patient was admitted to the hospital with submandibular swelling and suppuration from the surgical site, elevated fever, and acute left facial pain. She remained hospitalized for approximately two weeks, receiving intravenous antibiotics and steroids. Her physician referred her to an oral and maxillofacial surgeon for further consultation. At discharge, the patient was stable but continued to experience numbness and pain in her tongue, along with difficulties in speech and swallowing (Fig. 5).
Fig. 5
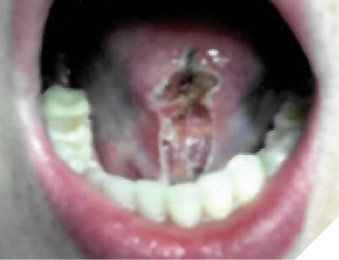
The patient was evaluated by an oral and maxillofacial surgeon 2 months later. Extensive scarring was noted across the floor of the mouth and the ventral surface of the tongue (Fig. 6). The ventral aspect of the tongue was scarred to the floor of the mouth. Due to the extent of scarring, the ventral surface of the tongue was difficult to distinguish the normal landmarks and anatomy of floor of the mouth. Clinical examination revealed significant loss of tongue mobility, anesthesia affecting the anterior third of the tongue including loss of taste and symptoms of dysphagia and dysarthria. Significant muscle deterioration was noted.
Fig. 6
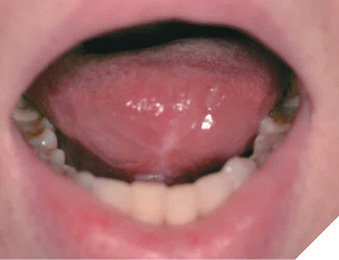
While some permanent disability was anticipated, multiple surgeries were planned to restore as much function as possible. The first revision surgery by oral and maxillofacial surgical specialists was conducted approximately 6 months after the patient’s initial frenectomy. This involved major debridement of the ventral tongue scar and floor of the mouth with dermal grafting and soft tissue Z-plasty to improve tongue length. Initial results showed improved tongue range of motion and slight improvements in swallowing, but no improvements in speech. A second major revision surgery was performed six months later, which involved further debridement of the ventral tongue surface and a more extensive soft tissue Z-plasty to achieve greater tongue extension and scar reduction. Following this procedure, the patient reported additional improvements in swallowing and some enhancement in speech articulation, although her speech remained significantly slurred, with ongoing difficulties pronouncing /s/ and /t/ sounds. The patient reported continued loss of taste and paresthesia in the anterior third of her tongue.
A final major revision surgery was completed approximately 1.5 years later, focusing again on scar reduction and further improvements in tongue mobility. Following this procedure, the patient noted mild improvements in eating and swallowing, but no other further enhancements. The patient also reported she continued to be questioned socially and challenged academically on whether she was under the influence of drugs or alcohol due to her slurred speech. Ultimately, the patient was deemed to have a permanent disability due to her persistent lingual paresthesia, loss of taste, dysphagia, and dysarthria (Fig. 7).
Fig. 7
Discussion and Conclusion
While surgical release of tongue ties is generally considered a safe and simple procedure, surgical complications can have disastrous consequences.5,27,127,135-137 As more clinicians perform tongue tie releases with differing tools, new technology, and different techniques, clinicians must be aware of potential surgical complications, their clinical management, and their potential consequences. While there are certainly indications for tongue tie surgery as reviewed in our article, it is imperative that clinicians be well trained and educate patients/parents appropriately prior to any surgical procedure. Proper preoperative counseling can significantly enhance patient understanding, expectations, and consent. As reviewed in our case series, major complications from tongue tie surgery can include significant loss of function, inability to achieve hemostasis of the surgical site, secondary hemorrhage, blood loss leading to hypovolemic shock, decreased tongue range of motion, damage to salivary ducts, dysarthria, dysphagia, neuralgia, hypogeusia, chronic pain, psychologic and emotional toll to the patient and their family members. In some instances, these complications can become permanent disabilities with lifelong limitations to a person’s capabilities and development.
Moreover, it is important for clinicians to establish clear communication channels with patients and their families throughout the surgical process. Preoperative consultations should focus on discussing not only the benefits of the procedure but also the associated risks and complications. This shared decision-making approach fosters trust and allows families to make informed choices regarding their care. Postoperatively, regular follow-ups should be scheduled to monitor recovery and address any complications that may arise.
Furthermore, it is essential to recognize the impact of clinician experience and technique on surgical outcomes. As more practitioners enter the field of tongue tie surgery, ongoing education and mentorship become critical. The integration of simulation-based training and peer-reviewed case discussions could significantly improve surgical skills and decision-making processes. The potential for complications, especially in vulnerable populations such as neonates/infants and young children, necessitates a thorough understanding of both the anatomical nuances and the psychological aspects involved in the surgical journey. We emphasize the need for practitioners interested in providing tongue tie surgeries to seek advanced clinical education and work in conjunction with interdisciplinary teams for appropriate management and patient care. By fostering an environment of continuous learning and collaboration, we can enhance the safety and efficacy of frenotomies, ultimately benefiting patients affected by ankyloglossia across all age groups. In addition, any intention to proceed with a frenoplasty must be evidenced based and predictably demonstrate a true and proven benefit to the patient. 
Oral Health welcomes this original article.
References
- Becker S, Brizuela M, Mendez MD. Ankyloglossia (Tongue-Tie) [Updated 2023 Jun 9]. In: StatPearls [Internet].Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from https://www.ncbi.nlm.nih.gov/books/NBK482295/
- Jain P, Rathee M. Embryology, Tongue. [Updated 2023 Aug 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK547697/
- Ganesan K, Girgis S, Mitchell S. Lingual frenotomy in neonates: past, present, and future. Br J Oral Maxillofac Surg. 2019;57(3):207-13. https://doi.org/10.1016/j.bjoms.2019.03.004
- Pompéia LE, Ilinsky RS, Ortolani CLF, Faltin K, Jr. ANKYLOGLOSSIA AND ITS INFLUENCE ON GROWTH AND DEVELOPMENT OF THE STOMATOGNATHIC SYSTEM. Rev Paul Pediatr. 2017;35(2):216-21. https://doi.org/10.1590/1984-0462/;2017;35;2;00016.
- Messner AH, Walsh J, Rosenfeld RM, Schwartz SR, Ishman SL, Baldassari C, et al. Clinical Consensus Statement: Ankyloglossia in Children. Otolaryngol Head Neck Surg. 2020;162(5):597-611. https://doi.org/10.1177/0194599820915457.
- Hentschel R. Breastfeeding problems should be the only relevant criteria for deciding whether to carry out a frenotomy in infancy. Acta Paediatr. 2018;107(10):1697-701. https://doi.org/10.1111/apa.14439
- Hogan M, Westcott C, Griffiths M. Randomized, controlled trial of division of tongue-tie in infants with feeding problems. J Paediatr Child Health. 2005;41(5-6):246-50. https://doi.org/10.1111/j.1440-1754.2005.00604.x
- Messner AH, Lalakea ML, Aby J, Macmahon J, Bair E. Ankyloglossia: incidence and associated feeding difficulties. Arch Otolaryngol Head Neck Surg. 2000;126(1):36-9. https://doi.org/10.1001/archotol.126.1.36
- Francis DO, Chinnadurai S, Morad A, Epstein RA, Kohanim S, Krishnaswami S, et al. Treatments for Ankyloglossia and Ankyloglossia With Concomitant Lip-Tie [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2015 May. (Comparative Effectiveness Reviews, No. 149.) Executive Summary. Accessed September 9, 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK299112/ p. ES-1
- Francis DO, Chinnadurai S, Morad A, Epstein RA, Kohanim S, Krishnaswami S, et al. Treatments for Ankyloglossia and Ankyloglossia With Concomitant Lip-Tie [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2015 May. (Comparative Effectiveness Review No. 149). Accessed September 10, 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK299112/
- Elad D, Kozlovsky P, Blum O, Laine AF, Po MJ, Botzer E,et al. Biomechanics of milk extraction during breast-feeding. Proc Natl Acad Sci U S A. 2014;111(14):5230-5. https://doi.org/10.1073/pnas.1319798111
- Post ED, Rupert AW, Schulpen TW. Problematische borstvoeding door een te korte tongriem [Problematic breastfeeding due to a short frenulum]. Ned Tijdschr Geneeskd. 2010;154:A918. Dutch.
- Campanha SMA, Martinelli RLC, Palhares DB. Association between ankyloglossia and breastfeeding. Codas. 2019;31(1):e20170264. https://doi.org/10.1590/2317-1782/20182018264
- Geddes DT, Langton DB, Gollow I, Jacobs LA, Hartmann PE, Simmer K. Frenulotomy for breastfeeding infants with ankyloglossia: effect on milk removal and sucking mechanism as imaged by ultrasound. Pediatrics. 2008;122(1):e188-94. https://doi.org/10.1542/peds.2007-2553.
- Ballard JL, Auer CE, Khoury JC. Ankyloglossia: assessment, incidence, and effect of frenuloplasty on the breastfeeding dyad. Pediatrics. 2002;110(5):e63. https://doi.org/10.1542/peds.110.5.e63
- Walker RD, Messing S, Rosen-Carole C, McKenna Benoit M. Defining Tip-Frenulum Length for Ankyloglossia and Its Impact on Breastfeeding: A Prospective Cohort Study. Breastfeed Med. 2018;13(3):204-10. https://doi.org/10.1089/bfm.2017.0116
- Amir LH, James JP, Beatty J. Review of tongue-tie release at a tertiary maternity hospital. J Paediatr Child Health. 2005;41(5-6):243-5. https://doi.org/10.1111/j.1440-1754.2005.00603.x
- Buryk M, Bloom D, Shope T. Efficacy of neonatal release of ankyloglossia: a randomized trial. Pediatrics. 2011;128(2):280-88. https://doi.org/10.1542/peds.2011-0077
- Todd DA, Hogan MJ. Tongue-tie in the newborn: early diagnosis and division prevents poor breastfeeding outcomes. Breastfeed Rev. 2015;23(1):11-6.
- Berry J, Griffiths M, Westcott C. A double-blind, randomized, controlled trial of tongue-tie division and its immediate effect on breastfeeding. Breastfeed Med. 2012;7(3):189-93. https://doi.org/10.1089/bfm.2011.0030
- Dollberg S, Botzer E, Grunis E, Mimouni FB. Immediate nipple pain relief after frenotomy in breast-fed infants with ankyloglossia: a randomized, prospective study. J Pediatr Surg. 2006;41(9):1598-1600. https://doi.org/10.1016/j.jpedsurg.2006.05.024
- Edmunds J, Miles SC, Fulbrook P. Tongue-tie and breastfeeding: a review of the literature. Breastfeed Rev. 2011;19(1):19-26.
- Garbin CP, Sakalidis VS, Chadwick LM, Whan E, Hartmann PE, Geddes DT. Evidence of improved milk intake after frenotomy: a case report. Pediatrics. 2013;132(5):e1413-7. https://doi.org/10.1542/peds.2012-2651
- Ghaheri BA, Cole M, Fausel SC, Chuop M, Mace JC. Breastfeeding improvement following tongue-tie and lip-tie release: A prospective cohort study. Laryngoscope. 2017;127(5):1217-23. https://doi.org/10.1002/lary.26306
- Siegel SA. Aerophagia Induced Reflux in Breastfeeding Infants With Ankyloglossia and Shortened Maxillary Labial Frenula (Tongue and Lip Tie). Int J Clin Pediatr. 2016;5(1):6-8. https://doi.org/10.14740/ijcp246w
- Slagter KW, Raghoebar GM, Hamming I, Meijer J, Vissink A. Effect of frenotomy on breastfeeding and reflux: results from the BRIEF prospective longitudinal cohort study. Clin Oral Investig. 2021;25(6):3431-9. https://doi.org/10.1007/s00784-020-03665-y
- Griffiths DM. Do tongue ties affect breastfeeding? J Hum Lact. 2004;20(4):409-14. https://doi.org/10.1177/0890334404266976
- Miranda BH, Milroy CJ. A quick snip – A study of the impact of outpatient tongue tie release on neonatal growth and breastfeeding. J Plast Reconstr Aesthet Surg. 2010;63(9):e683-5. https://doi.org/10.1016/j.bjps.2010.04.003
- O’Callahan C, Macary S, Clemente S. The effects of office-based frenotomy for anterior and posterior ankyloglossia on breastfeeding. Int J Pediatr Otorhinolaryngol. 2013;77(5):827-32. https://doi.org/10.1016/j.ijporl.2013.02.022
- Wakhanrittee J, Khorana J, Kiatipunsodsai S. The outcomes of a frenulotomy on breastfeeding infants followed up for 3 months at Thammasat University Hospital. Pediatr Surg Int. 2016;32(10):945-52. https://doi/org/10.1007/s00383-016-3952-8.
- Veyssiere A, Kun-Darbois JD, Paulus C, Chatellier A, Caillot A, Bénateau H. Diagnostic et prise en charge de l’ankyloglossie chez le jeune enfant [Diagnosis and management of ankyloglossia in young children]. Rev Stomatol Chir Maxillofac Chir Orale. 2015;116(4):215-20. French. https://doi.org/10.1016/j.revsto.2015.06.003
- Srinivasan A, Dobrich C, Mitnick H, Feldman P. Ankyloglossia in breastfeeding infants: the effect of frenotomy on maternal nipple pain and latch. Breastfeed Med. 2006;1(4):216-24. https://doi.org/10.1089/bfm.2006.1.216
- Riskin A, Mansovsky M, Coler-Botzer T, Kugelman A, Shaoul R, Hemo M, et al. Tongue-tie and breastfeeding in newborns-mothers’ perspective. Breastfeed Med. 2014;9(9):430-7. https://doi.org/10.1089/bfm.2014.0072
- Kumar M, Kalke E. Tongue-tie, breastfeeding difficulties and the role of Frenotomy. Acta Paediatr. 2012;101(7):687-9. https://doi.org/10.1111/j.1651-2227.2012.02661.x
- Ito Y. Does frenotomy improve breast-feeding difficulties in infants with ankyloglossia? Pediatr Int. 2014;56(4):497-505. https://doi.org/10.1111/ped.12429
- Ghaheri BA, Cole M, Mace JC. Revision Lingual Frenotomy Improves Patient-Reported Breastfeeding Outcomes: A Prospective Cohort Study. J Hum Lact. 2018;34(3):566-74. https://doi.org/10.1177/0890334418775624
- Karabulut R, Sönmez K, Türkyilmaz Z, Demiroğullari B, Ozen IO, Bağbanci B, et al. Ankyloglossia and effects on breast-feeding, speech problems and mechanical/social issues in children. B-ENT. 2008;4(2):81-5.
- Martinelli RL, Marchesan IQ, Gusmão RJ, Honório HM, Berretin-Felix G. The effects of frenotomy on breastfeeding. J Appl Oral Sci. 2015;23(2):153-7. https://doi.org/10.1590/1678-775720140339
- Bordoni B, Morabito B, Mitrano R, Simonelli M, Toccafondi A. The Anatomical Relationships of the Tongue with the Body System. Cureus. 2018;10(12):e3695. https://doi.org/10.7759/cureus.3695
- Genna CW, Saperstein Y, Siegel SA, Laine AF, Elad D. Quantitative imaging of tongue kinematics during infant feeding and adult swallowing reveals highly conserved patterns. Physiol Rep. 2021;9(3):e14685. https://doi.org/10.14814/phy2.14685
- Baxter R, Hughes L. Speech and Feeding Improvements in Children After Posterior Tongue-Tie Release: A Case Series. Int J Clin Pediatr. 2018;7(3):29-35. https://doi.org/10.14740/ijcp295w
- Cheng J, Raynor E. Ankyloglossia and Dysphagia. In: Ongkasuwan J, Chiou E, eds. Pediatric Dysphagia. Springer; 2018. https://doi.org/10.1007/978-3-319-97025-7_13
- Buck LS, Frey H, Davis M, Robbins M, Spankovich C, Narisetty V, et al. Characteristics and considerations for children with ankyloglossia undergoing frenulectomy for dysphagia and aspiration. Am J Otolaryngol. 2020;41(3):102393. https://doi.org/10.1016/j.amjoto.2020.102393
- Matsuo K, Palmer JB. Anatomy and physiology of feeding and swallowing: normal and abnormal. Phys Med Rehabil Clin N Am. 2008;19(4):691-707, vii. https://doi.org/10.1016/j.pmr.2008.06.001
- Moulton K, Seikel JA, Loftin JG, Devine N. Examining the effects of ankyloglossia on swallowing function. Int J Oral Myol. 2018;44(1):5-21. https://doi.org/10.52010/ijom.2018.44.1.1
- Kummer AW. Ankyloglossia: to clip or not to clip? That’s the question. The Asha Leader. Dec 2005. https://doi.org/10.1044/leader.FTR2.10172005.6
- Brooks L, Landry A, Deshpande A, Marchica C, Cooley A, Raol N. Posterior Tongue Tie, Base of Tongue Movement, and Pharyngeal Dysphagia: What is the Connection? Dysphagia. 2020;35(1):129-32. https://doi.org/10.1007/s00455-019-10040-x
- Dezio M, Piras A, Gallottini L, Denotti G. Tongue-tie from embriology to treatment: a literature review. JPNIM. 2015;4(1):e040101. https://doi.org/10.7363/040101.
- Logemann JE. Evaluation and treatment of swallowing disorders. College Hill Press;1983:214–27.
- Dydyk A, Milona M, Janiszewska-Olszowska J, Wyganowska M, Grocholewicz K. Influence of Shortened Tongue Frenulum on Tongue Mobility, Speech and Occlusion. J Clin Med. 2023;12(23):7415. https://doi.org/10.3390/jcm12237415
- Ferrés-Amat E, Pastor-Vera T, Ferrés-Amat E, Mareque-Bueno J, Prats-Armengol J, Ferrés-Padró E. Multidisciplinary management of ankyloglossia in childhood. Treatment of 101 cases. A protocol. Med Oral Patol Oral Cir Bucal. 2016;21(1):e39-47. https://doi.org/10.4317/medoral.20736
- Hoang DA, Nguyen TM, Jagomägi T. Restricted tongue mobility and ankyloglossia in 6-8-year-old Vietnamese school children: prevalence and association with tongue strength and endurance. Eur Arch Paediatr Dent. 2024;25(6):791-9. https://doi.org/10.1007/s40368-024-00938-y.
- Tecco S, Baldini A, Mummolo S, Marchetti E, Giuca MR, Marzo G, et al. Frenulectomy of the tongue and the influence of rehabilitation exercises on the sEMG activity of masticatory muscles. J Electromyogr Kinesiol. 2015;25(4):619-28. https://doi.org/10.1016/j.jelekin.2015.04.003
- Walls A, Pierce M, Wang H, Steehler A, Steehler M, Harley EH Jr. Parental perception of speech and tongue mobility in three-year olds after neonatal frenotomy. Int J Pediatr Otorhinolaryngol. 2014;78(1):128-31. https://doi.org/10.1016/j.ijporl.2013.11.006
- Dollberg S, Manor Y, Makai E, Botzer E. Evaluation of speech intelligibility in children with tongue-tie. Acta Paediatr. 2011;100(9):e125-7. https://doi.org/10.1111/j.1651-2227.2011.02265.x
- Ostapiuk B, Logopedyczne PT. Asymmetry in sound production in persons with ankyloglossia. Logopedia 2010;39-40;113-37.
- Itoh S. [Clinical study on speech disorders and speech therapy of ankyloglossia]. Kokubyo Gakkai Zasshi. 1988;55(1):159-84. Japanese. https://doi.org/10.5357/koubyou.55.159
- Messner AH, Lalakea ML. The effect of ankyloglossia on speech in children. Otolaryngol Head Neck Surg. 2002;127(6):539-45. https://doi.org/10.1067/mhn.2002.129731
- Kim TH, Lee YC, Yoo SD, Lee SA, Eun YG. Comparison of simple frenotomy with 4-flap Z-frenuloplasty in treatment for ankyloglossia with articulation difficulty: A prospective randomized study. Int J Pediatr Otorhinolaryngol. 2020;136:110146. https://doi.org/10.1016/j.ijporl.2020.110146
- Lalakea ML, Messner AH. Ankyloglossia: the adolescent and adult perspective. Otolaryngol Head Neck Surg. 2003;128(5):746-52. https://doi.org/10.1016/S0194-59980300258-4
- Heller J, Gabbay J, O’Hara C, Heller M, Bradley JP. Improved ankyloglossia correction with four-flap Z-frenuloplasty. Ann Plast Surg. 2005;54(6):623-8. https://doi.org/10.1097/01.sap.0000157917.91853.be
- Salt H, Claessen M, Johnston T, Smart S. Speech production in young children with tongue-tie. Int J Pediatr Otorhinolaryngol. 2020;134:110035. https://doi.org/10.1016/j.ijporl.2020.110035
- 63. Marchesan IQ, Teixeira AN, Cattoni DM. Correlações entre diferentes frênulos linguais e alterações na fala. [Correlations between different lingual frenulum and speech disorders]. Distúrb Comun, São Paulo. 2010;22(3):195-200. Portuguese.
- 64. Braga LAS, Silva J, Pantuzzo CL, Motta AR. Prevalência de alteração no frênulo lingual e suas implicações na fala de escolares. [Prevalence of change in lingual frenulum and its implications in speech of school children]. Revista CEFAC. 2009;11(Suppl 3):378-90. https://doi.org/10.1590/S1516-18462009000700014
- 65. Ostapiuk B. Poglady na temat ruchomości jfizyka w ankyloglosji a potrzeby artykulacyjne [Tongue mobility in ankyloglossia with regard to articulation]. Ann Acad Med Stetin. 2006;52(Suppl 3):37-47. Polish.
- 66. Marchesan QI. Lingual frenulum: classification and speech interference. Int J Orofacial Myology. 2004;30:31-8.
- 67. Fletcher SG, Meldrum JR. Lingual function and relative length of the lingual frenulum. J Speech Hear Res. 1968;11(2):382-90. https://doi.org/10.1044/jshr.1102.382
- 68. Block JR. The role of the speech clinician in determining indications for frenulotomy in cases of ankyloglossia. N Y State Dent J. 1968;34(8):479-81.
- 69. PLUMMER RN. Tongue tie speech. Ariz Med. 1956;13(4):139.
- 70. Olivi G, Signore A, Olivi M, Genovese MD. Lingual frenectomy: functional evaluation and new therapeutical approach. Eur J Paediatr Dent. 2012;13(2):101-6.
- 71. Martinelli RLC, Marchesan IQ, Berretin-Felix G. [Estratégias de compensação na produção do flape alveolar em casos de anquiloglossia]. Compensatory strategies for the alveolar flap [ɾ] production in the presence of ankyloglossia. Revista CEFAC. 2019;21(3):310419. Portuguese. https://doi.org/10.1590/1982-0216/201921310419
- 72. Suzart DD, de Carvalho ARR. [Alterações de fala relacionadas às alterações do frênulo lingual em escolares]. Speech disorders related to alterations of the lingual frenulum in schoolchildren. Revista CEFAC. 2016;18(6):1332-9. Portuguese. https://doi.org/10.1590/1982-0216201618621715
- 73. Summersgill I, Nguyen G, Grey C, Norouz-Knutsen L, Merkel-Walsh R, Katzenmeir C, et al. Muscle tension dysphonia in singers and professional speakers with ankyloglossia: Impact of treatment with lingual frenuloplasty and orofacial myofunctional therapy. Int J of Orofacial Myology and Myofunctional Therapy. 2023:49(1):1-8. https://doi.org/10.52010/ijom.2023.49.1.1
- 74. Marchesan IQ. PROTOCOLO DE AVALIAÇÃO DO FRÊNULO DA LÍNGUA [Tongue frenulum evaluation protocol]. Revista CEFAC. 2010;12(6):977-89. Portuguese.
- 75. Wright JE. Tongue-tie. J Paediatr Child Health. 1995;31(4):276-8. https://doi.org/10.1111/j.1440-1754.1995.tb00810.x
- 76. Wang J, Yang X, Hao S, Wang Y. The effect of ankyloglossia and tongue-tie division on speech articulation: A systematic review. Int J Paediatr Dent. 2022;32(2):144-56. https://doi.org/10.1111/ipd.12802
- 77. Messner AH, Lalakea ML. Ankyloglossia: controversies in management. Int J Pediatr Otorhinolaryngol. 2000;31;54(2-3):123-31. https://doi.org/10.1016/s0165-5876(00)00359-1
- 78. Suter VG, Bornstein MM. Ankyloglossia: facts and myths in diagnosis and treatment. J Periodontol. 2009;80(8):1204-19. https://doi.org/10.1902/jop.2009.090086
- 79. Carnino JM, Rodriguez Lara F, Chan WP, Kennedy DG, Levi JR. Speech Outcomes of Frenectomy for Tongue-Tie Release: A Systematic Review and Meta-Analysis. Ann Otol Rhinol Laryngol. 2024;133(6):566-74. https://doi.org/10.1177/00034894241236234
- 80. Melong J, Bezuhly M, Hong P. The Effect of Tongue-Tie Release on Speech Articulation and Intelligibility. Ear Nose Throat J. 2024;103(7):NP450-54. https://doi.org/10.1177/01455613211064045
- 81. Bhattad MS, Baliga MS, Kriplani R. Clinical guidelines and management of ankyloglossia with 1-year followup: report of 3 cases. Case Rep Dent. 2013;2013:185803. https://doi.org/10.1155/2013/185803
- 82. Belmehdi A, El Harti K, El Wady W. Ankyloglossia as an oral functional problem and its surgical management [Zrost języka z dnem jamy ustnej jako wada czynnościowa i jej leczenie chirurgiczne]. Dent Med Probl 2018;55(2):213-16.
- 83. Iyer VH, Sudersan S. A comprehensive Treatment Protocol for Lingual Frenectomy with Combination of Lasers and Speech Therapy: Two Case Reports. Int J Laser Dent. 2015;(1):12-21.
- 84. Ito Y, Shimizu T, Nakamura T, Takatama C. Effectiveness of tongue-tie division for speech disorder in children. Pediatr Int. 2015;57(2):222-6. https://doi.org/10.1111/ped.12474
- 85. Yoon AJ, Zaghi S, Ha S, Law CS, Guilleminault C, Liu SY. How tongue mobility changes face and jaw development. Accessed September 9, 2024. https://doi.org/10.21203/rs.2.15056/v1
- 86. Ardekani MD, Tabatabaee Z, Halvani N, Tabatabaee H, Yasaee S. Evaluation of Hyoid Position in Children of 7-11 Years Old with Ankyloglossia in Lateral Cephalometic Radiographs. Maedica (Bucur). 2016;11(3):198-202.
- 87. Mew J. Guest Editorial. The influence of the tongue on dentofacial growth. Angle Orthod. 2015;85(4):715. https://doi.org/10.2319/angl-85-04-715-715.1
- 88. Yoon AJ, Zaghi S, Ha S, Law CS, Guilleminault C, Liu SY. Ankyloglossia as a risk factor for maxillary hypoplasia and soft palate elongation: A functional – morphological study. Orthod Craniofac Res. 2017;20(4):237-44. https://doi.org/10.1111/ocr.12206
- 89. Vaz AC, Bai PM. Lingual frenulum and malocclusion: An overlooked tissue or a minor issue. Indian J Dent Res. 2015;26(5):488-92. https://doi.org/10.4103/0970-9290.172044
- 90. Calvo-Henríquez C, Neves SM, Branco AM, Lechien JR, Reinoso FB, Rojas XM, et al. Relationship between short lingual frenulum and malocclusion. A multicentre study. Acta Otorrinolaringol Esp (Engl Ed). 2022;73(3):177-83. https://doi.org/10.1016/j.otoeng.2021.01.003
- 91. Meenakshi S, Jagannathan N. Assessment of lingual frenulum lengths in skeletal malocclusion. J Clin Diagn Res. 2014;8(3):202-4. https://doi.org/10.7860/JCDR/2014/7079.4162
- 92. Cordray H, Mahendran GN, Tey CS, Nemeth J, Raol N. The Impact of Ankyloglossia Beyond Breastfeeding: A Scoping Review of Potential Symptoms. Am J Speech Lang Pathol. 2023;32(6):3048-63. https://doi.org/10.1044/2023_AJSLP-23-00169
- 93. Biswas P, Agarwal N, Saha P, Ansari N, Choudhary S, Sharma P. Lingual frenulum length: A prospecting link to craniofacial morphology in adults. J Orthod Sci. 2023;12:54. https://doi.org/10.4103/jos.jos_108_22
- 94. Shah SS, Agarwal PV, Rathi N, Agarwal SR, Tasgaonkar A. Tongues Tied by Orofacial Myofunctional Therapy about Tongue Tie: A Narrative Review. Int J Clin Pediatr Dent. 2024;17(1):109-13. https://doi.org/10.5005/jp-journals-10005-2736
- 95. Defabianis P. Ankyloglossia and its influence on maxillary and mandibular development. (A seven year follow-up case report). Funct Orthod. 2000;17(4):25-33.
- 96. Jang SJ, Cha BK, Ngan P, Choi DS, Lee SK, Jang I. Relationship between the lingual frenulum and craniofacial morphology in adults. Am J Orthod Dentofacial Orthop. 2011;139(4 Suppl):e361-7. https://doi.org/10.1016/j.ajodo.2009.07.017
- 97. Srinivasan B, Chitharanjan AB. Skeletal and dental characteristics in subjects with ankyloglossia. Prog Orthod. 2013;14:44. https://doi.org/10.1186/2196-1042-14-44
- 98. Ewart NP. A lingual mucogingival problem associated with ankyloglossia: a case report. N Z Dent J. 1990;86(383):16-17.
- 99. Virji SA, Ng ET, Jayachandran S, Heit TC. A case study on myofunctional therapy and malocclusions created by oral habits. Can J Dent Hyg. 2023;57(1):61-8.
- 100. Vroegop AV, Vanderveken OM, Boudewyns AN, Scholman J, Saldien V, Wouters K, et al. Drug-induced sleep endoscopy in sleep-disordered breathing: report on 1,249 cases. Laryngoscope. 2014;124(3):797-802. https://doi.org/10.1002/lary.24479
- 101. Lai YJ, Li CY, Hung CH, Lin C. Severity of tongue base collapse in various body positions in patients with obstructive sleep apnea: A trajectory analysis. J Formos Med Assoc. 2024;123(11):1175-81. https://doi.org/10.1016/j.jfma.2024.01.033
- 102. Sung CM, Tan SN, Shin MH, Lee J, Kim HC, Lim SC, et al. The Site of Airway Collapse in Sleep Apnea, Its Associations with Disease Severity and Obesity, and Implications for Mechanical Interventions. Am J Respir Crit Care Med. 2021;204(1):103-106. https://doi.org/10.1164/rccm.202011-4266LE
- 103. Hendricks R, Patel Z, Suleman L, Khalfey H, Engela E, Adams S. The role of the tongue base in obstructive sleep apnoea. 2024;1-12. Transactions of the Royal Society of South Africa, 1–12. https://doi.org/10.1080/0035919X.2024.2355464
- 104. Mukai S, Mukai C, Asaoka K. Ankyloglossia with deviation of the epiglottis and larynx. Ann Otol Rhinol Laryngol Suppl. 1991;153:3-20. https://doi.org/10.1177/00034894911000s501
- 105. Villa MP, Evangelisti M, Barreto M, Cecili M, Kaditis A. Short lingual frenulum as a risk factor for sleep-disordered breathing in school-age children. Sleep Med. 2020;66:119-22. https://doi.org/10.1016/j.sleep.2019.09.019
- 106. Huang YS, Quo S, Berkowski JA, Guilleminault C. Short lingual frenulum and obstructive sleep apnea in children. Int J Pediatr Res 2015;1:003.
- 107. Brożek-Mądry E, Burska Z, Steć Z, Burghard M, Krzeski A. Short lingual frenulum and head-forward posture in children with the risk of obstructive sleep apnea. Int J Pediatr Otorhinolaryngol. 2021;144:110699. https://doi.org/10.1016/j.ijporl.2021.110699
- 108. Bussi MT, Corrêa CC, Cassettari AJ, Giacomin LT, Faria AC, Moreira APSM, et al. Is ankyloglossia associated with obstructive sleep apnea? Braz J Otorhinolaryngol. 2022;88 Suppl 1(Suppl 1):S156-62. https://doi/org/10.1016/j.bjorl.2021.09.008
- 109. Guilleminault C, Huseni S, Lo L. A frequent phenotype for paediatric sleep apnoea: short lingual frenulum. ERJ Open Res. 2016;2(3):00043-2016. https://doi.org/10.1183/23120541.00043-2016
- 110. Mukai S, Mukai C, Asaoka K. Congenital ankyloglossia with deviation of the epiglottis and larynx: symptoms and respiratory function in adults. Ann Otol Rhinol Laryngol. 1993;102(8 Pt 1):620-4. https://doi.org/10.1177/000348949310200810
- 111. Zaghi S, Valcu-Pinkerton S, Jabara M, Norouz-Knutsen L, Govardhan C, Moeller J, et al. Lingual frenuloplasty with myofunctional therapy: Exploring safety an efficacy in 348 cases. Larynscope Investig Otolaryngol. 2019:4(5):489-96. https://doi.org/10.1002/lio2.297
- 112. Camacho M, Certal V, Abdullatif J, Zaghi S, Ruoff CM, Capasso R, et al. Myofunctional Therapy to Treat Obstructive Sleep Apnea: A Systematic Review and Meta-analysis. Sleep. 2015;38(5):669-75. https://doi.org/10.5665/sleep.4652
- 113. Govardham C, Murdock J, Norouz-Knutsen L, Valcu-Pinkerton S, Zaghi S. Lingual and maxillary labial frenuloplasty with myofuntional therapy as a treatment for mouth breathing and snoring. Case Rep Otolaryngol. 2019;3408053 https://doi.org/10.1155/2019/3408053
- 114. Correa EJ, O’Connor-Reina C, Rodríguez-Alcalá L, Benjumea F, Casado-Morente JC, Baptista PM, et al. Does Frenotomy Modify Upper Airway Collapse in OSA Adult Patients? Case Report and Systematic Review. J Clin Med. 2022;12(1):201. https://doi.org/10.3390/jcm12010201
- 115. Akbari D, Bogaardt H, Docking K. Ankyloglossia in Central Australia: Prevalence, identification and management in infants. Int J Pediatr Otorhinolaryngol. 2023;170:111604. https://doi.org/10.1016/j.ijporl.2023.111604
- 116. Klockars T. Familial ankyloglossia (tongue-tie). Int J Pediatr Otorhinolaryngol. 2007;71(8):1321-4. https://doi.org/10.1016/j.ijporl.2007.05.018
- 117. Han SH, Kim MC, Choi YS, Lim JS, Han KT. A study on the genetic inheritance of ankyloglossia based on pedigree analysis. Arch Plast Surg. 2012;39(4):329-32. https://doi.org/10.5999/aps.2012.39.4.329
- 118. Walsh J, McKenna Benoit M. Ankyloglossia and Other Oral Ties. Otolaryngol Clin North Am. 2019;52(5):795-811. https://doi.org/10.1016/j.otc.2019.06.008
- 119. Ricke LA, Baker NJ, Madlon-Kay DJ, DeFor TA. Newborn tongue-tie: prevalence and effect on breast-feeding. J Am Board Fam Pract. 2005;18(1):1-7. https://doi.org/10.3122/jabfm.18.1.1
- 120. Puapornpong P, Raungrongmorakot K, Mahasitthiwat V, Ketsuwan S. Comparisons of the latching on between newborns with tongue-tie and normal newborns. J Med Assoc Thai. 2014;97(3):255-9.
- 121. Hill RR, Lee CS, Pados BF. The prevalence of ankyloglossia in children aged <1 year: a systematic review and meta-analysis. Pediatr Res. 2021;90(2):259-66. https://doi.org/10.1038/s41390-020-01239-y
- 122. Tomara E, Dagla M, Antoniou E, Iatrakis G. Ankyloglossia as a Barrier to Breastfeeding: A Literature Review. Children (Basel). 2023;10(12):1902. https://doi.org/10.3390/children10121902
- 123. González Jiménez D, Costa Romero M, Riaño Galán I, González Martínez MT, Rodríguez Pando MC, Lobete Prieto C. Prevalencia de anquiloglosia en recién nacidos en el Principado de Asturias [Prevalence of ankyloglossia in newborns in Asturias (Spain)]. An Pediatr (Barc). 2014;81(2):115-9. Spanish. https://doi.org/10.1016/j.anpedi.2013.10.030
- 124. Jamilian A, Fattahi FH, Kootanayi NG. Ankyloglossia and tongue mobility. Eur Arch Paediatr Dent. 2014;15(1):33-5. https://doi.org/10.1007/s40368-013-0049-0
- 125. Ellehauge E, Jensen JS, Grønhøj C, Hjuler T. Trends of ankyloglossia and lingual frenotomy in hospital settings among children in Denmark. Dan Med J. 2020;67(5):A01200051.
- 126. Joseph KS, Kinniburgh B, Metcalfe A, Razaz N, Sabr Y, Lisonkova S. Temporal trends in ankyloglossia and frenotomy in British Columbia, Canada, 2004-2013: a population based study. CMJA Open. 2016;4(1):E33-40. https://doi.org/10.9778/cmajo.20150063
- 127. Walsh J, Tunkel D. Diagnosis and Treatment of Ankyloglossia in Newborns and Infants: A Review. JAMA Otolaryngol Head Neck Surg. 2017;143(10):1032-9. https://doi.org/10.1001/jamaoto.2017.0948
- 128. American Academy of Pediatrics. AAP Addresses Rise in Tongue-Tie Diagnoses for Breastfeeding Concerns. August 2024. Accessed September 8, 2024. https://www.healthychildren.org/English/news/Pages/AAP-report-addresses-rise-in-tongue-tie-diagnoses-for-breastfeeding-concerns.aspx#:~:text=When%20breastfeeding%20difficulties%20arise%2C%20a,report%20by%20the%20American%20Academy.
- 129. NYTimes. Inside the Booming Business of Cutting Babies’ Tongues. Accessed September 9, 2024. https://www.nytimes.com/2023/12/18/health/tongue-tie-release-breastfeeding.html
- 130. Katie Dangerfied. Global News. Is tongue-tie surgery for babies needed? Experts are divided. Aug 17, 2024. Accessed September 8, 2024. https://globalnews.ca/news/10700050/tongue-tie-surgery-babies-overdiagnosis/
- 131. CBS News. Tongue-ties may be overdiagnosed and needlessly treated in infants, pediatrician group says. July 29, 2024. Accessed September 8, 2024. https://www.cbsnews.com/news/tongue-ties-overdiagnosis-needless-treatment-infants-pediatrics/
- 132. The Washington Post. What are tongue-ties, and can they be fixed. June 10, 2024. Accessed September 9, 2024. https://Washingtonpost.com/wellness/2024/06/10/tongue-tie-breastfeeding-babies-surgery
- 133. ABC NEWS. Williams C. Thursday. June 13, 2024. For some new mums, navigating the complexity of tongue-ties can be a tricky topic. Accessed September 9, 2024. https://www.abc.net.au/news/2024-06-14/tongue-tie-release-australia-parents-health-care-professionals/103923260
- 134. The Sydney Morning Herald. A Miracle solution for some, ‘barbaric’ for others. The truth behind the boom in cutting babies’ tongues. Accessed September 9, 2024. https://www.smh.com.au/national/a-miracle-solution-for-some-barbaric-for-others-the-truth-behind-the-boom-in-cutting-babies-tongues-20240502-p5foac.html
- 135. Hale M, Mills N, Edmonds L, Dawes P, Dickson N, Barker D, et al. Complications following frenotomy for ankyloglossia: A 24-month prospective New Zealand Paediatric Surveillance Unit study. J Paediatr Child Health. 2020;56(4):557-62. https://doi.org/10.1111/jpc.14682
- 136. Francis DO, Krishnaswami S, McPheeters M. Treatment of ankyloglossia and breastfeeding outcomes: a systematic review. Pediatrics. 2015;135(6):e1458-66. https://doi.org/10.1542/peds.2015-0658
- 137. Solis-Pazmino P, Kim GS, Lincango-Naranjo E, Prokop L, Ponce OJ, Truong MT. Major complications after tongue-tie release: A case report and systematic review. Int J Pediatr Otorhinolaryngol. 2020;138:110356. https://doi.org/10.1016/j.ijporl.2020.110356
About the authors

Dr. Kevin E. Lung is the Chief, Pediatric Oral and Maxillofacial Surgery, Stollery Children’s/University Hospital, Edmonton, Alberta, and Director, Undergraduate and GPR Implant Surgery Clinic, Faculty of Medicine and Dentistry at the University of Alberta. He has a private practice at Kingsway Oral Surgery, Edmonton, Alberta.

Dr. Jason Adam is in General Practice Residency, Edmonton, Alberta.

Dr. Enoch T. Ng has a practice at Enjoy Dental, Edmonton, Alberta.