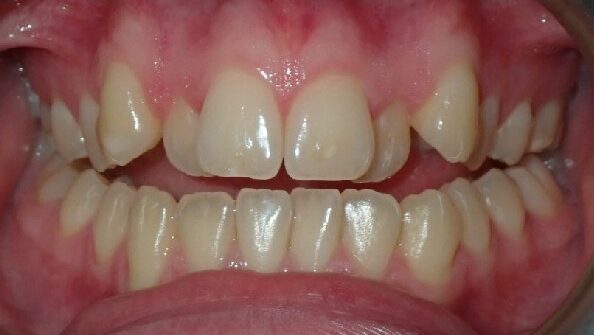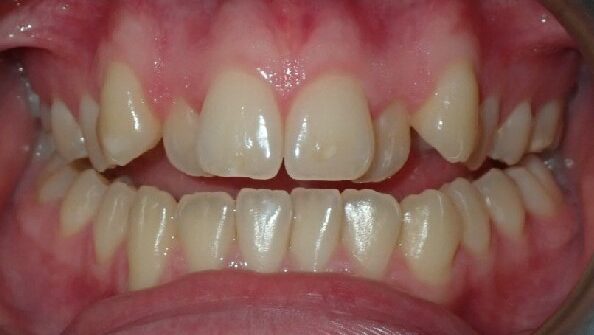
One of the most challenging malocclusions to treat orthodontically is an anterior open bite (AOB). This malocclusion is defined as a lack of occlusal contacts between the incisors +/- the canines in maximum intercuspation resulting in a lack of vertical overlap of the incisors and occurs for several reasons (Table 1).1-3 It is important to discuss this malocclusion due to incisal guidance being an important component of a functional occlusion, the prevalence in our mixed dentition patients being estimated to be around every 1 in 5 patients,4 and that if the underlying cause of the AOB is not resolved there is a high chance of relapse after orthodontic forces are removed.2,5 These cases can be disappointing for both orthodontists and patients when they need retreatment and, even then, our prognosis for stability is guarded.
Table 1: Causes of anterior open bite
| Non-nutritive sucking habits – thumb, pacifier, blankets1, digits6 |
| Airway (mouth breathing) – adenoid and tonsil hypertrophy, allergic rhinitis7, nasal septum deviation8 |
| Hereditary growth patterns – posterior vertical excess of dentoalveolar and skeletal bases4 |
| Condylar resorption9,10 |
| Anterior tongue thrust11 and low tongue posture12 |
| Size of the tongue – macroglossia13 |
| Iatrogenic long term night guard use14 |
AOBs are traditionally categorized into skeletal, dental, or a combination but it may be more nuanced when we attempt to better understand how this malocclusion develops. Moss hypothesized that any alteration to the craniofacial muscles can affect the growth of the underlying skeletal structures and dentition.15 When we can better understand and manipulate the factors that may be responsible for these occlusal relationships we can develop a treatment plan to minimize negative vertical changes over time. There are several treatment modalities available depending on the patient’s age and severity of the malocclusion (Table 2).3,9,16,17,18 If habit cessation occurs before the age of three there is literature to support spontaneous resolution of the AOB.19,20 As orthodontists, the recommendation of the American Association of Orthodontists to see our patients at age 7 can decrease the successful spontaneous improvement if habits are allowed to persist this long. Taking a thorough medical history for habits and evaluating swallow with lips retracted are important for diagnosing potential orofacial dysfunctions. It is also prudent to evaluate nasal patency to better understand if an ENT evaluation is indicated for mouth breathing and tongue thrust21 and this can be done by directing these patients for referral through their family doctor. It is important to note that observing AOB changes in the early mixed dentition should be critically assessed since we are witnessing active eruption of permanent dentition which can attribute to some of the open bite.
Read related article: Myofunctional therapy can transform your dental hygiene career
Table 2: Treatment options for anterior open bite and mechanisms of action
| Habit cessation – allows anterior tooth eruption |
| Habit breaking appliances (cribs) – nociceptive reflex prevents tongue thrust and allows anterior tooth eruption |
| Tongue spurs – nociceptive reflex prevents tongue thrust and allows anterior tooth eruption |
| Posterior bite blocks – intrudes posterior teeth for autorotation (forward and up) closure of mandible |
| TADs/Miniscrews – intrudes posterior teeth for autorotation (forward and up) closure of mandible |
| Vertical Elastics – extrudes maxillary and mandibular incisors |
| Extractions – retroclines and extrudes incisors |
| Clear aligners – selective intrusion of posterior teeth |
| Orthognathic surgery – surgically repositions maxilla and allows for autorotation (forward and up) closure of the mandible |
| Clenching exercises – intrudes posterior teeth for autorotation (forward and up) closure of the mandible |
| Orofacial myofunctional therapy – retrains tongue resting and swallowing position along with lip seal and allows for natural anterior tooth eruption |
Orofacial myofunctional therapy (OMT) has become a hot topic over the last decade due to a paradigm shift for airway awareness and care. The majority of articles look at OMT as a successful modality to treat obstructive sleep apnea and sleep disordered breathing.7,22 As an orthodontic resident I had to do a literature search on OMT and it was incredibly frustrating in that the papers would say, “this group did myofunctional therapy” and the reader was left still wondering, “what is myofunctional therapy?” Out of my own curiosity I enrolled in the introductory course through the Academy of Orofacial Myofunctional Therapy (AOMT). It was then that I realized that my own father (a retired dentist) had tried some form of OMT on me by having me hold a popsicle stick between my lips to help improve my lip seal. Did it work? No. Did I understand the importance of it? Also, no. The aims of OMT exercises are to treat disorders of the stomatognathic system such as lip incompetence and mouth breathing, tongue thrust habit, improper joint patterns and mandibular deviation, chewing and swallowing patterns23 with the goals being improved occlusal stability, enhanced facial esthetics, and increased patient satisfaction alongside orthodontic treatment.24 Shah et al. have done a wonderful job describing with photographs the most current exercises used in OMT for those interested in learning more.12 Looking back through the literature we can see that OMT is not a new idea but its definition has changed to be more limited to the tongue position and lip seal through a series of facial and tongue exercises focusing on proper tongue resting and swallowing positions.24 Profit noted that historically in the 1920s OMT was originally a term used for exercises aimed at stretching the muscles of mastication forward for those patients with mandibular retrognathism to help remodel and “grow” the mandible in a forward direction.32 By the 1950s, Straub used the term OMT to distinguish a different set of exercises for AOBs caused by “malfunction of the tongue”. In 1976 Profit stated that “myofunctional therapy refers broadly to any therapeutic approach which involves muscle exercises, whether an appliance is involved or not,” but made special note that most of our attention falls towards open bites and tongue function. His historic words ring true almost 50 years later in that depending on your beliefs on how malocclusions develop you will lean towards extractions if you believe in hereditary influences and you will lean towards non-extraction if you believe environmental influences are amenable to OMT. 32
My preferred patient to include OMT in their treatment plan is during interceptive orthodontic treatment in the early mixed dentition with a thumb habit and AOB (Fig. 1).3 In the presence of a habit the tongue sits inferiorly on the floor of the mouth and thrusts anteriorly to press against the incisors to create a seal during swallowing. If this persists after habit cessation we continue to see an alteration of the incisor eruption. The importance of this is that we are eliminating one habit to replace it with an improved habit – improved tongue position at rest and swallowing to allow the tongue to provide a buccal force on the lingual surfaces of the maxillary posterior teeth and remove it from the anterior teeth to allow for natural incisor eruption. OMT in growing children has been shown to yield greater improvements of AOB correction but it is important to note that they likely start with larger open bites18 and that their compliance may be less22 making predictability a challenge. There is also discussion as to when timing might be best to start OMT as Klocke et al. reviewed longitudinal growth patterns and showed spontaneous bite closure occurring until the age of 12.25 This study, of course, was in the absence of habits and tongue thrusts. The challenges with understanding the efficacy of OMT over the last decade is that the literature has remained scarce and biased with lack of randomization and attrition of participants making drawing conclusions on its benefits difficult to quantify.23,26 While we do need more robust studies on this treatment modality there are a few studies demonstrating a statistically significant difference in AOB stability for those treated with orthodontics and OMT than with orthodontics alone.18,24
Fig. 1A
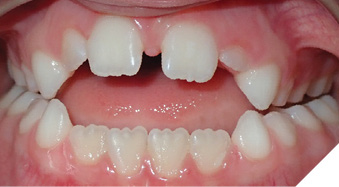
Fig. 1B
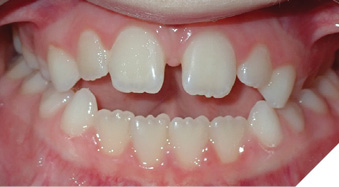
Fig. 1C
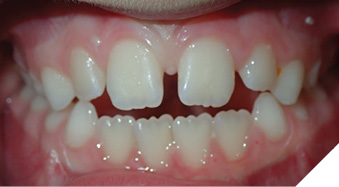
Patient A (Fig. 1A-C) presented to us at 7.2 years old and had stopped her pacifier habit several months prior. Her orthodontic plan can be found in Table 3. We referred her to a speech-language pathologist (SLP) for OMT and her diagnosis and treatment plan can be found in Table 4. While anyone licensed in an allied health field (SLP, RDH, DDS, DMD, OT, PT) can perform OMT, I find our SLPs have a different diagnostic criteria than the dental field and they can develop a treatment plan to include speech therapy if there are any co-existing speech concerns. They work collaboratively with other health care providers such as orthodontists, dental specialists for tethered oral tissues, osteopaths, chiropractors, and discuss with their family physician about referral to ENT, allergist, or neurologist as needed. There is an additional benefit of insurance coverage for OMT if our patients have speech therapy benefits.
Table 3: Orthodontic diagnosis and treatment plan for Patient A
| Orthodontic Diagnosis | Orthodontic Treatment Plan |
| Straight profile Class II division 1 malocclusion Anterior open bite 5mm Spacing in the maxillary arch Mild crowding in the mandibular arch Maxillary diastema with strong maxillary labial frenum Constricted maxilla with bilateral posterior crossbites Low tongue posture and anterior tongue thrust | Referral to OMT and re-evaluate in 6 months After 6 months OMT open bite closed to 3mm: – Continue OMT – Maxillary expansion – Partial maxillary braces – 10-12 months – Retention Limitations/Concerns: May not achieve ideal open bite closure |
Table 4: OMT diagnosis and treatment plan for Patient A
| OMT Diagnosis | OMT Treatment Goals and Plan |
| Oromotor Exam: – subtle tethering of the labial frenum with spacing of maxillary incisors; labial strength and coordination was adequate with slight reduction in protrusion – reduced lingual tip elevation and depression extra orally; no activation of the lateral margins – tethering of sublingual oral tissue – palate high and narrow; velar elevation adequate and symmetrical Natural Oral Rest Posture: – moderate to severely poor oral rest posture characterized by low, forward tongue posture at rest (apex typically resting slightly between the anterior dentition; blade low); mildly elevated freeway space and lips apart at rest approximately half of the time Swallow Pattern: – moderate tongue thrust swallow pattern across all viscosities with observable increase of force, degree of protrusion, and amount of surface area of the teeth contacted by the tongue when moving and swallowing liquids and solids – demonstrated tendency to bring her tongue to the cup or spoon for each oral trial – poor bolus gathering, and mild mentalis strain during the swallow – frequent wiping of mouth with back of her hand post swallow Articulation: – sibilant distortions (frontal lisp) | Goals: a) establish proper oral rest posture (lips closed, tongue on alveolar ridge, nasal breathing) b) remediate gather and swallow pattern; eliminate tongue thrust and establish a mature swallow pattern c) educate caregivers on strategies for generalization and maintenance d) articulation remediation should family decide to pursue elimination of sibilant distortions Treatment plan: Phase One – Development of New Muscle Movements (5-7 weekly sessions) Phase Two – Integrating Movements into Patterns (3-5 weekly sessions) Phase Three – Strengthening Patterns (2-3 sessions biweekly) Phase Four – Retention (2-3 sessions as requested or recommended by clinician) Outcomes and Challenges: Patient was very self-motivated to improve oral rest position but regression was noted when due to scheduling conflicts sessions were deferred. Lisp is still present but can be addressed after expansion is completed |
Patient B (Figs. 2A-C) presented to us at 20 years old with the chief concern that after two rounds of braces elsewhere and maxillary and mandibular fixed retainer she did not like her AOB. She self-reported that she had upper and lower braces in grade 5 for 2 years and again in grade 9 for 1.5 years. Her orthodontic diagnosis and treatment plan can be found in Table 5 and her OMT diagnosis and treatment plan can be found in Table 6. With the addition of OMT this patient was able to maintain stability of her overbite correction at her most recent re-evaluation three years into retention.
Fig. 2A
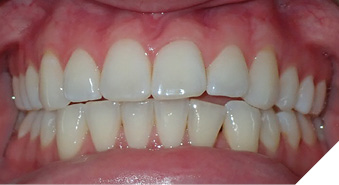
Fig. 2B
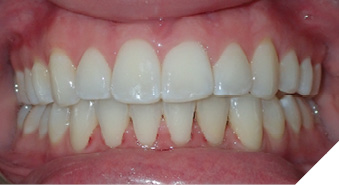
Fig. 2C
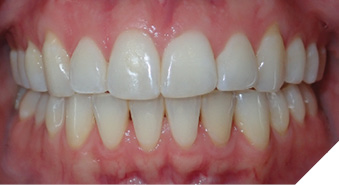
Table 5: Orthodontic diagnosis and treatment plan for Patient B
| Orthodontic Diagnosis | Orthodontic Treatment Plan |
| Convex profile Retrognathic mandible Class II division 1 malocclusion Excess overjet 5mm Proclined incisors Open bite tendency Mild crowding in the mandibular arch Tongue thrust Previous orthodontics with fixed retainers | Remove fixed retainers Referral to OMT Maxillary and mandibular retreatment with clear aligners Longterm retention with fixed and removable retainers Limitations/Concerns: Risk of anterior open bite relapse |
Table 6: OMT diagnosis and treatment plan for Patient B
| OMT Diagnosis | OMT Treatment Goals and Plan |
| Oromotor Exam: – TMJ click, no lock or pain Airway: – self-reports snoring and drooling at night – observed to have lips together at rest approximately half of the time during today’s assessment – slightly apart at other times Oral Habits: – gum chewing and bites cuticles Dental: – history of splint use Natural Oral Rest Posture: – mild to moderately poor oral rest posture, characterized by lips only intermittently together at rest; mentalis strain observed with labial contact; tongue tip rests against teeth and tongue blade low in oral cavity with elevated freeway space Swallow Pattern: – mild anterior tongue thrust swallow – adequate mastication and bolus gathering – overactive mentalis and forward tongue movement across viscosities (liquid and solid) – licks lips after each trial | Goals: a) Prior to initiating sessions, extinguish oral habits that are counterproductive to the goal of optimal oral rest posture (i.e. gum chewing, finger skin biting) b) establish optimal oral rest posture (lips closed, tongue on alveolar ridge, tongue blade to palate, nasal breathing) c) eliminate tongue thrust swallow d) educate client on generalization and maintenance Treatment plan: Phase One – Development of New Muscle Movements (5 weekly sessions) Phase Two – Integrating Movements into Patterns (3 weekly sessions) Phase Three – Strengthening Patterns (3 sessions biweekly) Phase Four – Retention (not needed) Outcomes: Optimal rest posture achieved |
While myofunctional therapy sounds like the perfect solution for every patient there are factors that can hindrance its success. Sadly, most of our follow up reports from our myofunctional colleague report “patient not interested in proceeding with services” (Table 7). With our patients’ increasingly busy lives compliance becomes the biggest hurdle. This challenge has resulted in the creation of a one-page instruction sheet for patients to work on their resting tongue position at home (Fig. 5).
Table 7: Factors limiting success of myofunctional therapy18
| Patient Factors | Orthodontist Factors | Myofunctional Therapist Factors |
| Additional cost | Limited office space | Difference in training and expertise |
| Time consuming | Lack of trained provider | |
| Compliance based motivation | Time consuming | |
| Ability to follow instructions | Thought that there is not enough scientific literature support | |
| Parental motivation |
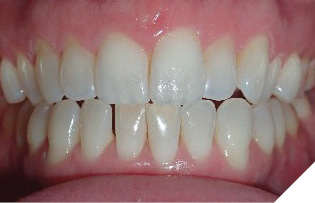
There have been a handful of patients who have spontaneously demonstrated surprisingly positive bite changes without OMT and have made me start to question the overall role of our facial muscles in combination with the tongue and lips for the correction of AOBs. Patient C presented with a challenging AOB occluding only on her second molars (Fig. 3). Time was needed to finalize the treatment plan as there were several molars treated with root canals and an uncommon extraction pattern was decided to be presented. Upon returning to the office for finalization of the treatment plan it was no longer deemed appropriate due to the spontaneous improvement of the bite and she was treated with braces and elastics alone. Patient D returned to the office 17 years after her initial evaluation. Her treatment plan was orthognathic surgery and, upon returning, was able to be treated with clear aligners alone (Fig. 4). One of the commonalities among these patients was stress and self-reported clenching. There are theories for our vertical growers with increased lower face heights that their facial muscles are hypotonic and generate weaker masticatory forces allowing the molars to erupt and act as a wedge effect to open the bite anteriorly. Additional research is needed to evaluate if clenching exercises would be beneficial for AOB correction and stability if the TMJ structures allow. In essence, the tongue and lips are very important but our musculature, as a whole, dictates the forces on our skeleton as the original definition of OMT intended.
Fig. 3A
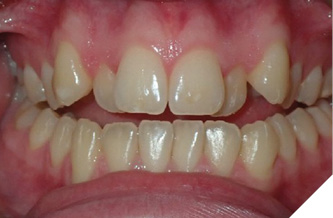
Fig. 3B
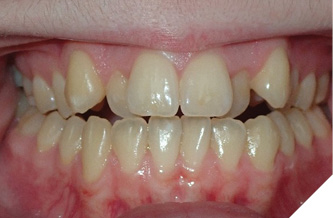
Fig. 4A
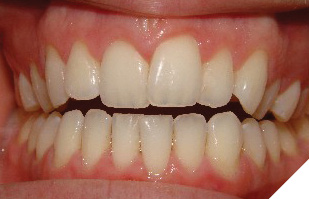
Fig. 4B
Maintaining AOB closures after orthodontic treatment remains one of the greatest orthodontic challenges and there have been several recommendations suggested to maintain overbite correction. One of the challenges in evaluating open bite stability after orthodontic treatment is the lack of discussion regarding retention protocols and strategies.18 My preference for mixed dentition retention is a maxillary Hawley with a palatal window as it maintains our maxillary width after expansion and provides a physical reminder for ideal resting tongue position at the anterior palate. While the Bluegrass appliance is theoretically effective, it occupies the anterior palate and the space where the tongue should ideally be resting. Careful thought should be given to retention strategies depending on the underlying cause of the anterior open bite (Table 8).
Table 8: Retention strategies
| Maxillary Hawley with posterior bite planes – prevents supraerption of the posterior teeth for better vertical control |
| Maxillary Hawley with palatal window – allows tongue to sit on the palate with a physical reminder |
| Bluegrass appliance – stimulates tongue movement against the palatal bead as a physical reminder |
| Maxillary and Mandibular vacuum-formed retainers – posterior bite block effect |
| Maxillary and Mandibular fixed lingual retainers bonded canine-to-canine – minimizes incisor intrusion |
Our goals as dentists and orthodontists are to work collaboratively to screen and identify habits that may be contributing negatively to the growth and development of our early mixed dentition patients and to educate our patients and parents on the negative effects that these prolonged habits can have on occlusion and optimal function. Having tried a handful of myofunctional appliances in our office and having been unsuccessful with them it can be hard seeing patients for the first time who have already been in these programs for years without seeing success. When patients need further orthodontic treatment it can be a financial burden if they have already used a significant portion of their lifetime orthodontic benefit. It is for this reason that I urge you to better understand the causes of AOBs to help gauge the success of your outcome before prescribing treatment. Collaboration can open the door for your patient’s success, but their motivation is the only way for them to walk through it.
 Fig. 5
Fig. 5

Oral Health welcomes this original article.
Acknowledgement: Special Thanks and Acknowledgement to Shanda Hunter-Trottier at SpeechWorks (slhunterspeechworks.com) for collaborating and caring for our patients.
References
- Sá de Lira A,RSA. Influence of non-nutritive sucking habits on anterior open bite. Brazilian Journal of Oral Sciences. 2020; 20.
- Paik CH,LMH,PJH. Treatment strategies for vertical maxillary excess: Cases with and without anterior open bite. Seminars in Orthodontics. 2024; 30: p. 648-672.
- Tanny L,HB,YNN,CG. Non-orthodontic interventions and non-nutritive sucking behaviours: a literature review. Kaoshiung Journal of Medical Sciences. 2018; 34: p. 215-222.
- Cozza P,BT,FL,MM,PA. Sucking habits and facial hyperdivergency as risk factors for anterior open bite in the mixed dentition. Am J Orthod Dentofacial Orthop. 2005; 128: p. 517-9.
- Remmers D,VHR,BE,BS,KC. Treatment results and long-term stability of anterior open bite malocclusion. Orthod Craniofac Res. 2008;(11): p. 32-42.
- Popovich F,TG. Thumb- and finger-sucking: its relation to malocclusion. Am J Orthod. 1973; 63: p. 148-155.
- Zhang F TZSYZBYHLSLQ. Efficiency of oro-facial myofunctional therapy in treating obstructive sleep apnoea: A meta-analysis of observational studies. J Oral Rehabil. 2022 Jul; 49(7): p. 734-745.
- Watson W. Open-bite – a multifactorial event. Am J Orthod. 1981; 80: p. 443-446.
- Kato C,OT. Anterior open bite due to temporomandibular joint osteoarthrosis with muscle dysfunction treated with temporary anchorage devices. Am J Orthod Dentofacial Orthop. 2018; 154(6): p. 848-859.
- Wolford L. Idiopathic condylar resorption of the temporomandibular joint in teenage girls (cheerleader’s syndrom). Proc (Bayl Med Univ Cent). 2001; 14: p. 246-252.
- Meyer-Marcotty P HJSEA. Dentoalveolar open bite treatment with spur appliances. J Orthofac Orthop. 2007; 68: p. 510-521.
- Shah SS NMBVea. Orofacial Myofunctional Therapy in Tongue Thrust Habit: A Narrative Review. Int J Clin Pediatr Dent. 2021; 14(2): p. 298-303.
- Miyawaki S,OS,TYT. Long-term changes in dentoskeletal pattern in a case with Beckwith-Wiedemann syndrome following tongue reduction and orthodontic treatment. Angle Orthod. 2000; 70: p. 326-331.
- Bereznicki T,BEWNHF. Unintended changes to the occlusion following the provision of night guards. British Dental Journal. 2018; 225(8): p. 717-724.
- Moss M. The primacy of functional matrices in orofacial growth. Dent Pract Dent Rec. 1968; 19: p. 65-73.
- Bosio J,JR. Treatment and retreatment of a patient with a severe anterior open bite. Am J Orthod Dentofacial Orthop. 2013 Oct; 144(4): p. 594-606.
- Scheffler N,PW,PC. Outcomes and stability in patients with anterior open bite and long anterior face height treated with temporary anchorage devices and a maxillary intrusion splint. Am J Orthod Dentofacial Orthop. 2014; 146: p. 594-602.
- Smithpeter J,CD. Relapse of anterior open bites treated with and without orofacial myofunctional therapy. Am J Orthod Dentofacial Orthop. 2019; 137: p. 605-614.
- Moimaz SAS RNdGASO. The effect of breastfeeding in the acquisition of non-nutritive sucking habits and malocclusion prevention. Rev Odontol UNESP. 2013; 42(1): p. 31-6.
- Warren JJ BS. Duration of nutritive and nonnutritive sucking behaviors and their effects on the dental arches in theprimary dentition. Am J Orthod Dentofacial Orthop. 2002; 121: p. 347-56.
- Dahan JS LO. Effects of bite raising and occlusal awareness on tongue thrust in untreated children. Am J Orthod Dentofac Orthop. 2003; 124: p. 165-172.
- Saba EKHHPJN. Orofacial Myofunctional Therapy for Obstructive Sleep Apnea: A Systematic Review and Meta-Analysis. Laryngoscope. 2024; 134: p. 480-495.
- Homem A,VAR,FS,RJM,ML. Effectiveness of orofacial myofunctional therapy in orthodontic patients: A systematic review. Dental Press J Orthod. 2014; 19(4): p. 94-99.
- AlQhtani F. Evaluating the impact of myofunctional therapy on orthodontic treatment outcomes. J Pharm Bioall Sci. 2024; 16: p. S2667-9.
- Klocke A NBK. Anterior open bite in the deciduous dentition: longitudinal follow-up and craniofacial growth considerations. Am J Orthod Dentofacial Orthop. 2002; 122: p. 353-358.
- Koletsi D MMP. Effect of orthodontic management and orofacial muscle training protocols on the correction of myofunctional and myoskeletal problems in developing dentition. A systematic review and meta-analysis. Orthod Craniofac Res. 2018; 21: p. 202-215.
- Proffit W,PC,TT. Stability following superior repositioning of the maxilla by LeFort I osteotomy. Am J Orthod Dentofacial Orthop. 1987; 92(2): p. 151-161.
- Epker B,FL. Surgical-orthodontic correction of open bite deformity. Am J Orthod. 1977; 71: p. 278-299.
- Seemaan J,KG,SdC. Relationship between occlusal findings and and orofacial myofunctional status in primary and mixed dentition Part IV. J Orthofac Orthop. 2011; 72: p. 21-32.
- Van Dyck C,DA,VE,ME,GA,FS,&WG. The effect of orofacial myofunctional treatment in children with anterior open bite and tongue dysfunction: a pilot study. European Journal of Orthodontics. 2016; 38(3): p. 227-234.
- Ingervall B,SR. Effect of surgical reduction of the tongue on oral stereognosis, oral motor ability, and the rest position of the tongue and mandible. Am J Orthod Dentofac Orthop Off Publ Am Assoc Orthod Its Const Soc Am Board Orthod. 1990; 97: p. 58-65.
- Brandt, S. (1977) JCO Interviews Dr. William R. Proffit on the proper role of myofunctional therapy. J Clin Ortho. 11(2), 101
About the author

Dr. Melissa Milligan completed her DMD at UBC in 2012 and her orthodontic residency at UofT in 2016. She currently works in private practice in Burlington and Waterdown and is a clinical instructor for the department of graduate orthodontics at UofT. She is passionate about organized dentistry, continuing education, and technological advancements in dentistry.