Advancements in the field of dental implant therapy have lead to predictable survival rates of dental implants. 1 The current definition of success in addition to long-term predictability, function and integration of the implant focuses on esthetic considerations. 1,2 In the anterior maxilla this is more critical due to the visibility of the region and if a high lip line is present, the smile line is more revealing thus increasing the need for an esthetic result, with some authors ranking function and aesthetics in the anterior maxillary region to be of equal importance. 3-6
The esthetic component of an implant is dictated by the soft tissue framing, which is defined as the gingival contour that surrounds the prosthesis, this includes the preservation of the interdental papillae and a gingival margin which is symmetrical with the adjacent gingival architecture. 7,8 The interdental papilla to completely fill the space between teeth or implants can be achieved by having the crest of the interproximal bone within 5mm of the proposed contact point of the final restoration. 1,9-11 An ideal emergence profile is achieved when there is proper placement of the implant in a correct 3-dimensional position. 1,12 The centering of the implant mesiodistally is important and requires a minimum of 1.5mm of space between the implant and the adjacent natural tooth or implant;1,8,12 if this distance is violated, than a loss of interdental papilla is expected. 12 Evaluation of the position in a labial-palatal direction is also important because placement too far labially may result in overcontouring of the crown, which cannot be corrected for prosthetically. 1 Labial malpositioning can also cause recession due to a decrease in thickness of buccal bone. 11 Palatal placement is also contraindicated because it may require a modified ridge lap, thus limiting the type of design and increasing the difficulty for maintenance. 13-16 The third and final dimension of concern is apicoronal malpositioning. If too apical there is an expected bone resorption and gingival recession, while a coronal placement may be unesthetic due to the visibility of the implant shoulder. 1,12 The implant should be placed 1.5mm to 3.0mm below the CEJ for optimal implant esthetics. 17 It is thus evident that in order to have ideal esthetics with implant prosthesis adequate bone must be present to allow for proper placement of the implant. 18 If deficiencies are noticed during presurgical planning then appropriate corrective procedures must be undertaken. 2,18-20 Correction of bone defects can be done in a variety of ways which include barrier membranes with guided bone regeneration, 2,18-20 onlay grafts, block grafts or distraction osteogenesis.
Guided bone regeneration is a predictable method for the regeneration of adequate volume of bone for implant placement and can be done simultaneously with implant placement or in a staged approach. 21-25 Even though immediate implant placement has shown comparable success rates a delayed or staged placement may be a better choice in esthetic areas when there are defects observed. 2,18-20
This article illustrates a case report where implant placement in the aesthetic zone has been done in a staged approach as there was inadequate supporting bone and soft tissue.
CASE REPORT
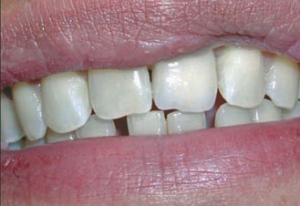
A 23-year-old female patient came in the clinic with the chief complaint of “I don’t like my tooth in the front and it is loose” (Fig. 1). Her medical history revealed a history of depression and anxiety that was related to her marital status. Her dental history revealed a fall on her face that she said occurred at least 10 years ago, no damage to her teeth was noted. A detailed examination revealed no missing teeth. Oral hygiene was satisfactory and her periodontal pocket depths were under 3mm in all teeth except the maxillary left central incisor which had pockets of 9mm on the mesial and 7mm on the distal aspect and had class II mobility associated with it. All her other teeth were generally in good health except for the bottom right and left molars which had occlusal decay and there was evidence of a discolored composite restoration on her maxillary right central incisor. Radiographically the clinical findings were verified and additionally revealed vertical bone loss that was limited to the maxillary left central incisor (Fig. 2). The maxillary left central incisor was deemed as a hopeless tooth. The patient was presented with different treatment options, after discussing the pros and cons of each the following treatment option was agreed upon; extraction of the maxillary left central incisor with concurrent bone grafting, followed by implant placement and subsequent restoration. During the healing phase a transitional removable partial denture would be fabricated for esthetics and function. For the occlusal decay on the molars Class I amalgams were recommended and for the discolored composite restoration on her maxillary right central incisor replacement of the composite with a new composite restoration was recommended.
PROCEDURE
1. Alginate impressions were taken of both arches and poured in Type II dental stone. Shade was selected and the casts were hand-articulated in maximum intercuspation (MI) and sent to the lab for the fabrication of a transitional maxillary partial denture.
2. At the patient’s next visit local anesthetic was administered in the area of the maxillary left upper incisor. An incision was made on the buccal and palatal aspect of the involved central incisor, releasing incisions were made on mesial of the adjacent central incisor and on the distal of the lateral incisor. A full thickness flap was raised, granulation tissue was removed and the maxillary left central incisor was extracted (Fig. 3). The extraction socket was thoroughly debrided and then packed with 0.25 to 1.0mm bovine cancellous bone granules and covered with a resorb-able bilayer collagen membrane (Fig. 4) following the guided bone regeneration (GBR) protocol. The gingiva was sutured to achieve primary closure. Following which the transitional maxillary partial denture was delivered, ensuring that it did not compress the underlying soft tissue and was not in occlusion. Post-surgically amoxicillin 500mg TID for five days and Chlorhexidine 0.12% 30ml rinse BID for seven days was prescribed, while Ibuprofen 200mg PRN was recommended for pain relief. The patient was put on a two week, one month and three month recall ensuring the proper management of the edentulous site.
3. In the recall visits healing was observed (Figs. 5 & 6), modifications to the transitional partial denture was done to ensure non-impingement of the underlying tissue and the occlusion modified to ensure minimal contact on the partial denture.
4. Six months after the GBR procedure a radiograph (Fig. 7) of the edentulous site was taken which revealed adequate bone volume, bone sounding was done and it was felt that there was about 7mm of bone in a bucco-palatal direction. It was decided that implant placement could be attempted at this time. For the fabrication of a surgical template an alginate impression was taken.
5. After infiltrating appropriate anesthetic in the area of the missing central incisor a palatally positioned full-thickness incision was made and the flap was raised (Fig. 8). Bone width was measured to be 8mm and following the manufacturers protocol for implant placement an ostectomy (Fig. 9) was drilled with the help of the surgical template. A parallel sided, threaded, rough surface implant was then placed and primary stability was achieved at 35N, a healing abutment was placed on top of the implant and the flap was closed with the help of silk 3.0 sutures (Fig. 10). The maxillary transitional enture was relieved to accommodate for the healing abutment (Fig. 11). A post surgical rad
iograph was taken, and it showed adequate placement (Fig. 12). Post surgically the patient was prescribed Chlorhexidine 0.12% mouth rinse 30ml BID for seven days and for pain Ibuprofen 200mg PRN was suggested.
6. The patient was seen post-surgically after one week for suture removal, no untoward sign or symptom was noted.
7. Six weeks after implant placement the healing abutment was removed and an impression coping placed, followed by a Poly Vinyl Siloxane open-tray impression to capture the position of the implant (Fig. 13). The impression coping was removed and the healing abutment replaced, shade was also recorded. The case was then sent to the laboratory for temporary crown and custom abutment fabrication.
8. The patient was now seen after eight weeks of healing, at this time the healing abutment was removed and the customized UCLA abutment (Fig. 14) was placed; a radiographic was taken to confirm the seating of the abutment (Fig. 15). The abutment was then torqued to 35N with the help of a torque wrench. The temporary crown was then placed, the proximal contacts and occlusion verified. In MI there was light contact with no contact in protrusive and lateral excursions. The temporary crown was then cemented with the help of a noneugenol based temporary cement (Fig. 16). Excess cement was removed and the occlusion was verified again.
9. The patient was then seen after 12 weeks when it was decided to proceed with the final restoration. The patient was booked four weeks later.
10. After 16 weeks of healing since implant placement the temporary crown was removed and the gingival was observed for healing (Fig. 17), it exhibited an adequate amount of interdental papilla and the buccal contours were observed to be similar to the adjacent tooth. An abutment level impression using PVS was made and sent to the laboratory for fabrication of the final prosthesis. Prior to this the temporary crown was re-cemented for the duration it required to fabricate the final prosthesis.
11. Final restoration was delivered at 20 week after implant placement. The temporary crown was removed, the abutment cleaned with copious amounts of water and the final crown was then tried in. The proximal contacts and occlusion was checked to ensure minor contact in MI with similar contact to the adjacent teeth in protrusive and lateral excursions, once established. The crown was then cemented using a resin modified glass ionomer cement (Fig. 18). Excess cement was removed the occlusion verified. At this time the composite on the adjacent central incisor was also replaced with a new composite matching the shade of the final prosthesis.
The patient was very happy with the final esthetic and functional outcome (Fig. 19).
DISCUSSION
A differential diagnosis to the cause of the problem associated with the patient’s maxillary left central incisor was ambiguous. The patient did present with a history of trauma but the typical findings of wounds, injuries to the oral mucosa, fracture of the tooth, pulp exposure, -ve vitality tests, displacement and mobility 26 were not evident, though the patient did report displacement but it would be difficult to conclusively state that as the reason. Another diagnosis could be localized aggressive periodontitis which exhibits itself typically with small amounts of plaque, mobility and migration of the molars and incisors, increase in the size of the clinical crown and rapid progression. 27 In addition the patient did report stress due to marital problems and it has been suggested that depression and stress can be a contributing risk factor. 28 Despite the inconclusive etiology, the diagnosis of a hopeless tooth was made on sound clinical signs and symptoms.
Alternate treatment modalities to our treatment plan included a removable partial denture, fixed partial dentures and resin bonded bridges (Maryland bridges). Removable partial dentures while an option can contribute to the loss of alveolar bone on both abutment and non-abutment teeth29 along with that the dissatisfaction rate of removable partial dentures is relatively high, ranging
fro 9-26%..30 On the other hand the use of fixed partial dentures would have required the unnecessary destruction of adjacent teeth to prepare them as abutments and loss of pristine tooth structure. Another option would be a resin bonded bridge, which would reduce the amount of adjacent tooth destruction but with a high incidence of pontic failure and debonding31 we felt an implant would have been the best option.
Using the classification system proposed by Funato et al. 2007, the site in this case was Class IV which is characterized by vertical and buccal bone loss. 3 Immediate implant placement in a class IV site may result in a deviation from the alveolar housing and a compromised esthetic result. 3 It was thus necessary to perform bone and tissue augmentation so that optimal gingival profiling and a more esthetic result could be achieved. 3,32 Extraction sockets will have an in growth of bone that is accompanied by narrowing and shortening of the ridge. 25 This resorption can be as much as 4mm after six months of healing. 25 Socket preservation in the anterior region is achieved by various methods but always involves an atraumatic extraction technique. 25,33 When performing a staged implant placement an initial socket grafting accompanied by an absorbable collagen dressing will allow for a healing environment that is isolated from the oral cavity. 25 Guided bone regeneration using barrier membranes allow for bone progenitor cells to develop uninhibited by the surrounding soft tissue cells. 21 The membrane disrupts in growth of soft tissue cells, which in turn are not able to disturb osteogenesis. 21 Use of this augmentation method can result in a vertical gain anywhere from 2.4mm to 5.1mm, 24 and a horizontal gain from 1.3mm to 3.7mm.23,24 The expected healing time required can be anywhere from five months to 10 months. 23,24 Agaloo et al. 2007 reported a 95.5% implant success rate with the use of guided bone augmentation. 22 The site is reevaluated after an appropriate healing time to determine if the alveolar housing is adequate for ideal three-dimensional implant placement.
CONCLUSION
Immediate implants, while a viable and successful option, are a beneficial form of treatment but some cases would benefit from a staged approach to allow for a successful and desirable esthetic result. This article illustrates a case where the authors describe a step-by-step approach that resulted in a predictable and esthetically pleasing smile. OH
Adnan Qayyum, BDS, DDS. Private Practice, Allentown, PA.
M. Najeeb Saad, BDS, C. Prosthodontics. Assistant Professor Schulich School of Medicine & Dentistry, University of Western Ontario.
Cameron Crawford, B. Sc(Hons), DDS candidate 2010. Schulich School of Medicine & Dentistry, University of Western Ontario.
Oral Health welcomes this original article
REFERENCES
1. Bashutski JD, Wang HL. Common implant esthetic complications. Implant Dent. 2007;16(4):340-8.
2. Simeone P, De Paoli C, De Paoli S, Leofreddi G, Sgr S. Interdisciplinary treatment planning for single-tooth J Esthet Restor Dent. 2007;19(2): 79-88;
3. Funato A, Salama MA, Ishikawa T, Garber DA, Salama H. Timing, positioning, and sequential staging in esthetic implant therapy: a four-dimensional perspective. Int J Periodontics Restorative Dent. 2007;27(4):313-23.
4. Garber DA. The esthetic dental implant: letting restoration be the guide. J Oral Implantol. 1996;22(1): 4550.
5. Kamalakidis S, Paniz G, Kang KH, Hirayama H. Nonsurgical management of soft tissue deficiencies for anterior single implant-supported restorations: a clinical report. J Prosthet Dent. 2007;97(1): 1-5
6. Sadan A, Blatz MB, Salinas T
J, Block MS. Singleimplant restorations: a contemporary approach for achieving a predictable outcome. J Oral Maxillofac Surg. 2004;62(9 Suppl 2):73-81
7. Garber DA, Salama MA, Salama H. Immediate total tooth replacement. Compend Contin Educ Dent. 2001;22(3):210-6, 218.
8. Paolantoni G, Marenzi G, Fusco A, Sammartino G. Implant rehabilitation of central incisor: a staged approach. Implant Dent. 2007;16(4):349-55.
9. Tarnow DP, Elian N, Fletcher P, Froum S, Magner A, Cho SC, Salama M, Salama H, Garber D. Vertical Distance from the crest bone to the height of the interproximal papilla between adjacent implants Journal of Periodontology 2003; 74(12) 1785-1788.
10. Tarnow DP, Magner AW, Fletcher P: The effect of distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol 1992; 63(12): 996-996.
11. Kois J. Altering gingival levels: the restorative connection. Part 1. Biological variable. J Esthet Dent 1994;6(3) 9.
12. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 Suppl:43-61.
13. Belser UC, Bernard JP, Buser D. Implant-supported restorations in the anterior region: Prosthetic Considerations. Pract Periodontics anasthet dent 1996;8:875-883.
14. Belser UC, Buser D, Hess D, Schmid B, Bernard JP, Lang NP. Aesthetic implant restorations in partially edentulous patients-A critical appraisal. Periodontol 2000 1998;17:132-150
15. Parel SM, Sullivan DY. Esthetics and Osseointegration. Dallas: Osseointegration Seminars, 1989.
16. Tarnow DP, Eskow RN. Considerations for single-unit esthetic implant restorations. Compend Contin Educ Dent 1995:16:782-784.
17. Zetu L, Wang HL. Management of inter-dental/inter-implant papilla. J Clin Periodontol. 2005;32: 831-839.
18. Carrin JB, Barbosa IR. Single implant-supported restorations in the anterior maxilla. Int J Periodontics Restorative Dent. 2005;25(2):149-55.
19. Stephen L. Wheeler. Implant Complications in the Esthetic Zone. J Oral Maxillofac Surg 65: 93-102, 2007, Suppl 1.
20. Malmquist JP. Successful Implant Restoration with the Use of Barrier Membranes Oral Moxillofoc Surg 1999;57(11) 114-i 116.
21. Esposito M. Interventions for replacing missing teeth: bone augmentation techniques for dental implant treatment. Cochrane Database of Systematic Reviews 2008. Issue 4, 2005.
22. Aghaloo TL, Moy PK. Which hard tissue augmentation techniques are the most successful in furnishing bony support for implant placement? Int J Oral Maxillofac Implants. 2007;22 Suppl:49-70.
23. Hmmerle CH, Jung RE, Yaman D, Lang NP. Ridge augmentation by applying bioresorbable membranes and deproteinized bovine bone mineral: a report of twelve consecutive cases. Clin Oral Implants Res. 2008;19(1):19-25.
24. Kfir E, Kfir V, Eliav E, Kaluski E. Minimally invasive guided bone regeneration. J Oral Implantol. 2007;33(4):205-10.
25. Sclar AG: Ridge Preservation for Optimum Esthetics and Function. The Bio-Col Technique. Compendium 1999;6(1).
26. Andreasen JO. Traumatic injuries of the teeth. chapter 2: examination and diagnosis of dental injuries. Munksgaard. Copenhagen 1972.
27. Carranza FA, Newman MG. Clinical periodontology 8th edition. W. B Saunders Company. Philadelphia 1996.
28. Saletu A, Pirker-Frhauf H, Saletu F, Linzmayer L, Anderer P, Matejka M. Controlled clinical and psychometric studies on the relation between periodontitis and depressive mood. J Clin Periodontol. 2005;32(12):1219-25.
29. Z lataric DK, Celebic A, Valentic -Peruzovic M. The effect of removable partial dentures on periodontal health of abutment and non-abutment teeth. J Periodontol. 2002;73(2):137-44.
30. Frank RP, Milgrom P, Leroux BG, Hawkins NR. Treatment outcomes with Mandibular removable partial dentures: A population based study of patient satisfaction. J Prosthet Dent. 1998;80(1): 36-45.
31. Berekally TL, Smales RJ. A retrospective clinical evaluation of resin-bonded bridges inserted at the Adelaide Dental Hospital. Aust Dent J. 1993;38(2):85-96.
32. Salama H, Salama MA, Li TF, Garber DA, Adar P. Treatment planning 2000: an esthetically oriented revision of the original implant protocol. J Esthet Dent. 1997;9(2):55-67.
33. Nevins M. Camelo M. De Paoli S. Friedland B. Schenk R, Parma-Benfenati S, Simion M, Tinti C, Wagenberg B. A Study of the Fate of the Buccal Wall of Extraction Sockets of Teeth with Prominent Roots. Int J Periodontics, 2006;26(1): 19-29.
34. Wagner B, Kern M. Clinical evaluation of removable partial dentures 10 years after insertion: success rates, hygienic problems, and technical failures. Clin Oral Investig. 2000;4(2):74-80.
35. Creugers NH, Kyser AF, Van’t Hof MA. A seven-and-a-half-year survival study of resin-bonded bridges. J Dent Res. 1992;71(11): 1822-5.
36. Creugers NH, Van ‘t Hof MA. An analysis of clinical studies on resin-bonded bridges. J Dent Res. 1991;70(2):146-9.
———
ABSTRACT
Dentists placing implants are often faced with the dilemma of whether to place an immediate implant or not in the anterior maxilla. This article illustrates a step-by-step case where a decision to proceed with a staged approach was taken in light of the anatomy. Consideration of esthetic parameters allows us to make decisions that are predictable and lead to a highly esthetic result with harmony of the gingiva and teeth. As a technique the guided bone regeneration (GBR) method is shown to safely develop bone in areas where it was deficient and finally the prosthetic outcome using a UCLA abutment and crown has been illustrated.
———
Even though immediate implant placement has shown comparable success rates a delayed or staged placement may be a better choice
———
Immediate implants are a beneficial form of treatment but some cases would benefit from a staged approach to allow for a successful and desirable esthetic result