Geographic tongue (GT), also known as benign migratory glossitis, is a chronic, inflammatory oral condition of unknown etiology.1 It is characterized by erythematous lesions with irregular white borders, and is typically seen on the dorsal and lateral surfaces of the tongue in circinate2 or serpiginous patches.1 The lesions often alternate between periods of exacerbation and remission, and may appear in different locations within the oral cavity.3 This clinical pattern results from the loss of filiform papillae, which creates a smoother surface of the tongue, followed by their regeneration, which produces the characteristic white border.1
GT is a relatively common condition, affecting about 1 to 5 percent of the general population.2 Reported prevalence varies, with some studies noting higher rates in children1 and others in middle-aged adults.4 It is more prevalent in females, and its frequency tends to decrease with age.1 Although GT is usually asymptomatic,2 some patients experience discomfort or pain in the affected areas after consuming acidic, hot, or spicy foods and beverages.3 The exact causes of GT remain unclear; however, a combination of genetic, immunologic, and environmental factors are believed to play a role.5 Associations have been reported with systemic conditions such as psoriasis, a chronic inflammatory skin disorder with an immunogenetic basis, and with metabolic and autoimmune diseases, including diabetes mellitus.5
While GT most often involves the dorsal and lateral surfaces of the tongue, its occurrence in ectopic sites such as the buccal mucosa, lips, soft palate, uvula, or floor of the mouth is less common.3,5 These unusual presentations can closely resemble other oral mucosal diseases, including oral lichen planus, candidiasis, leukoplakia, and even early carcinoma, making accurate diagnosis crucial.6 Thus, this case highlights an uncommon presentation of GT, including involvement of the ventral tongue and floor of the mouth, sites that are less commonly affected, supported by clinical examination and biopsy.
Case presentation
A 74-year-old man was referred by his general dentist for evaluation of unusual oral lesions. His medical history included Type 1 diabetes mellitus (most recent HbA1c of 7.6%), hypertension, hyperlipidemia, atrial fibrillation, a previous stroke, myocardial infarction, cardiac surgery, and kidney disease. His medications included digoxin, amlodipine, metoprolol, valsartan, insulin, atorvastatin, ezetimibe, pantoprazole, allopurinol, and apixaban. He was not taking any immunosuppressive medications, had a smoking history negative for smoking, consumed no alcohol, and had no known drug allergies. During the initial consultation, the patient reported no pain or discomfort. He described having a “weird” tongue with multiple grooves and crevices, consistent with a fissured tongue, which is often associated with geographic tongue. He also mentioned a tendency to accumulate white film on his tongue unless he thoroughly brushed it. He denied any history of previous lesions in the same location.
Clinical findings
The lesions were first observed one week earlier during a routine dental appointment. At that time, the patient was unaware of their presence and reported no pain, burning, tingling, bleeding, or taste changes. There had been no recent alterations to his systemic health, medications or oral hygiene habits.
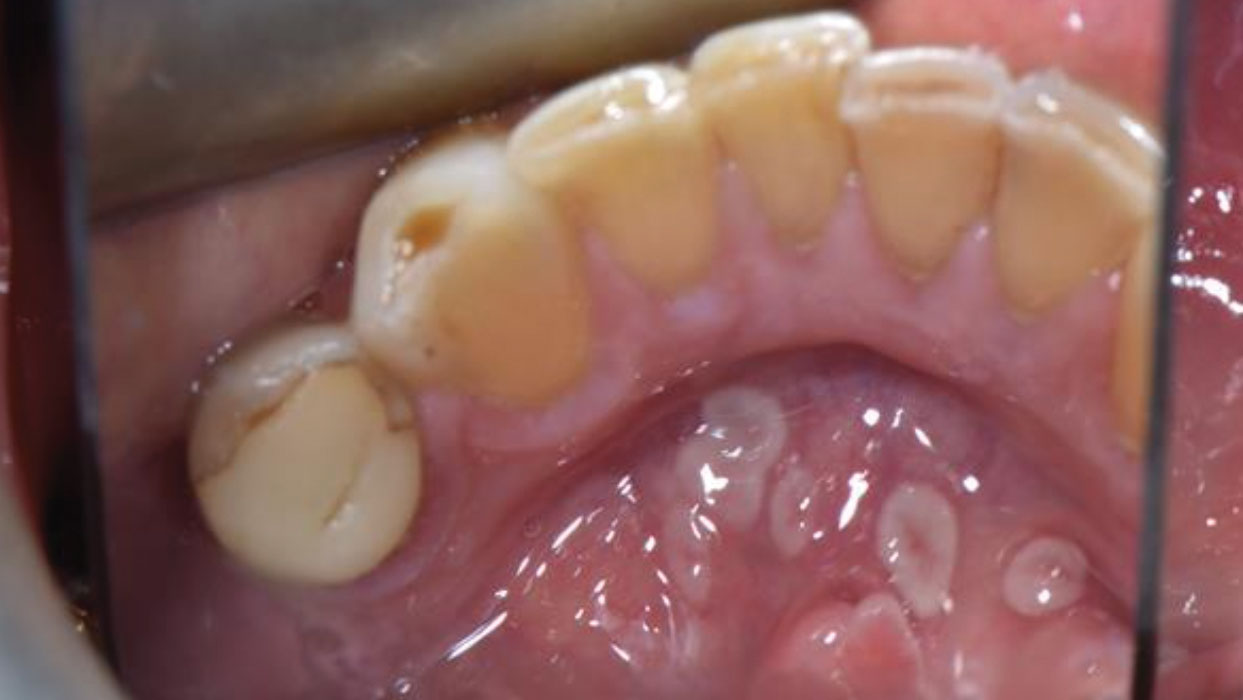
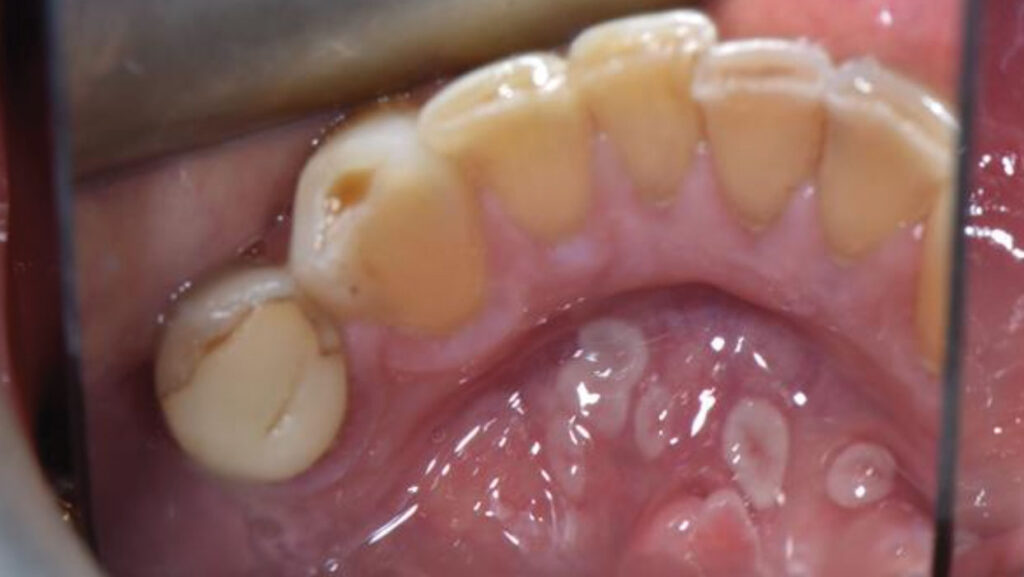
An intraoral examination revealed multiple crescent-shaped, well-defined erythematous and white lesions involving the dorsal surface of the tongue (Fig. 1), the ventral surface extending to the posterior floor of the mouth (Fig. 2), and most notably, around the midline of the anterior floor of the mouth (Fig. 3). Similar but smaller lesions were also observed on the right and left lateral borders of the tongue (Fig. 4). The largest lesion measured approximately 5 × 4 mm. All lesions were smooth and non-ulcerated, with no induration, bleeding, or signs of secondary infection. The lesions persisted without progression at the 3-month follow-up.
Fig. 1
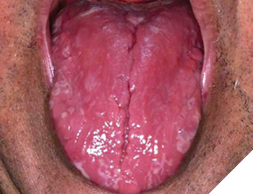
Fig. 2
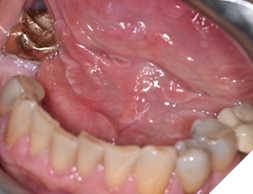
Fig. 3
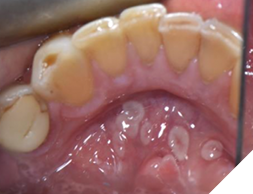
Fig. 4
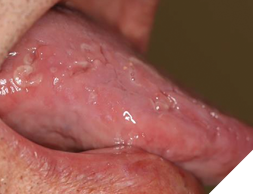
Diagnostic assessment
Given the unusual location of the lesions and their resemblance to other oral conditions, the clinical differential diagnoses included non-specific hyperkeratotic lesions or a potential oral lichenoid drug reaction to the patient’s current medications, possibly caused by amlodipine, valsartan, atorvastatin, or allopurinol. Other considerations included idiopathic lichen planus, chronic aphthous-like ulcers, early proliferative verrucous leukoplakia, and post-herpetic immune dysregulation. To determine the nature of the lesions and establish a definitive diagnosis, an incisional biopsy was performed under local anaesthesia on the largest lesion, situated just right of the midline on the anterior floor of the mouth (Fig. 3). The pathology report identified the lesion as geographic tongue, based on the presence of parakeratinized stratified squamous epithelium with neutrophil microabscesses, patchy chronic inflammatory infiltrates, and no candidal hyphae observed histologically.
Therapeutic intervention
The histopathological report confirmed a diagnosis of geographic tongue (GT), and therefore, no pharmacologic or surgical intervention was required. Given the benign and self-limiting nature of GT, management focused on patient education, reassurance, and prevention of potential irritant-induced symptoms.
The patient was advised to monitor for any changes in lesion size, appearance, or distribution, as well as the onset of new symptoms such as persistent pain, ulceration, or bleeding, and to report these promptly.
Home care recommendations:
- Maintain excellent oral hygiene with a soft-bristle rechargeable toothbrush, gently brushing the tongue surface to reduce food debris and biofilm accumulation, particularly in fissures.
- Use a mild, alcohol-free antimicrobial mouthrinse if irritation develops. Avoid high-alcohol rinses that can exacerbate discomfort.
- Limit consumption of acidic, spicy, salty, or very hot foods and beverages if they trigger symptoms.
- Keep the oral cavity well-lubricated by staying hydrated and using sugar-free xylitol gum or lozenges to relieve dryness.
- Avoid mechanical trauma from sharp or abrasive foods that may aggravate lesion borders.
- Consider temporary use of over-the-counter topical anesthetic gels (e.g., benzocaine) for short-term relief if mild burning occurs.
Given the patient’s systemic comorbidities, periodic re-evaluation during routine dental visits was advised to ensure stability and to detect any changes promptly.
Discussion
GT is most commonly diagnosed based on a distinctive history and characteristic clinical features, with histologic confirmation rarely needed. However, when lesions appear, biopsy remains the gold standard for confirming a diagnosis.4 Its cause is likely multifactorial, with evidence pointing to immune-related mechanisms and genetic predisposition.4 The link with systemic conditions, including psoriasis and diabetes, has also been well established.4
The patient’s history of hypertension and Type 1 diabetes may also be clinically relevant, as research has shown an increased prevalence of oral lesions, including GT, among hypertensive and diabetic individuals compared to the general population.7 Although the detailed mechanism is not fully understood, diabetes is known to impair mucosal immunity and epithelial integrity, likely influencing lesion development or persistence.8 The demographic profile in this case is also atypical, as GT occurs most frequently in younger adults and is more common in females,1 making its sudden presentation in a 74-year-old male unusual.
Another consideration to take into account is the patient’s medication history, as although causation has not been established, certain antihypertensive drugs (including amlodipine which the patient was taking), have been associated with increased prevalence of oral lesions and more specifically, GT.5, 7 Additionally, the co-occurrence of fissured tongue in this patient supports the final diagnosis, as fissured tongue is present in up to 40% of GT cases.9
Overall, this case underscores the importance of histopathological confirmation when GT appears in atypical locations, especially in older male patients with systemic conditions like diabetes and hypertension. Clinicians should stay alert that ectopic GT can closely resemble premalignant or malignant oral lesions, emphasizing the significance of biopsy to ensure accurate diagnosis and proper patient management.
Conclusion
In summary, this case highlights an uncommon ectopic presentation of geographic tongue involving the ventral surface of the tongue and the floor of the mouth. While GT is a benign condition, its occurrence in atypical sites can resemble more serious oral conditions such as leukoplakia, erythroplakia, candidiasis, and carcinoma. Clinically, oral health professionals should be especially alert to tongue changes during examinations of patients with diabetes and hypertension, given the higher prevalence of oral lesions in these groups. Recognizing these presentations is essential to prevent misdiagnosis, avoid unnecessary treatments, and lessen patient anxiety. Thorough clinical assessment, supported by biopsy when the location is unusual or patient risk factors are present, is essential to exclude dysplasia or malignancy. Documenting and sharing unusual presentations helps increase clinician awareness of GT variants, ultimately enhancing diagnostic accuracy and improving patient care.
Key clinical takeaways
Ectopic GT is uncommon: Geographic tongue most often affects the dorsal and lateral tongue; floor-of-mouth involvement is an uncommon variant that can mimic more serious lesions.
Consider broad differentials: Red and white oral lesions in atypical sites should prompt consideration of lichenoid reactions, leukoplakia, erythroplakia, candidiasis, and early carcinoma.
Biopsy is valuable: In unusual sites or high-risk patients, histopathologic confirmation is essential to rule out malignancy and reassure the patient.
Systemic associations are important: Type 1 diabetes and fissured tongue were present in this case, both of which have been reported to have associations with GT.
Patient reassurance is key: GT is benign and self-limiting; educating the patient about its migratory nature can significantly reduce anxiety.
Ongoing monitoring: Even with a benign diagnosis, periodic review ensures early detection of any changes. 
Oral Health welcomes this original article.
References
- Campana, F., Vigarios, E., Fricain, J.-C., & Sibaud, V. (2019). Geographic stomatitis with palate involvement. Anais Brasileiros de Dermatologia, 94(4), 449–451. https://doi.org/10.1590/abd180-4841.20197774
- Prasanth, V. J., & Singh, A. (2021). Geographic tongue. Canadian Medical Association Journal, 193(35). https://doi.org/10.1503/cmaj.202855
- Zadik, Y., Drucker, S., & Pallmon, S. (2011). Migratory stomatitis (ectopic geographic tongue) on the floor of the mouth. Journal of the American Academy of Dermatology, 65(2), 459–460. https://doi.org/10.1016/j.jaad.2010.04.016
- Ślebioda, Z., Drożdżyńska, J., Karpińska, A., Krzyżaniak, A., Kasperczak, M., Tomoń, N., Wiśniewska, P., & Wyganowska, M. L. (2025). Clinical characteristics and risk factors of geographic tongue: A retrospective analysis of 100 Polish patients. Healthcare, 13(11), 1299. https://doi.org/10.3390/healthcare13111299
- Ogueta, I. C., Ramírez, M. P., Jiménez, C. O., & Cifuentes, M. M. (2019). Geographic tongue: What a Dermatologist Should Know. Actas Dermo-Sifiliográficas (English Edition), 110(5), 341–346. https://doi.org/10.1016/j.adengl.2019.05.001
- Nandini, D. B. (2016). Paediatric geographic tongue: A case report, review and recent updates. Journal of Clinical and Diagnostic Research, 10(2), 5–9. https://doi.org/10.7860/jcdr/2016/16452.7191
- Al-Hajjar, S. H., Alhusseini, N. B., Annooz, T. S., Khalel, A. M., & Ibrahim, S. M. (2025). Common tongue manifestations in patients with diabetes and hypertension. The Open Public Health Journal, 18(1). https://doi.org/10.2174/0118749445402607250619104329
- Sanjeeta, N., Sivapathasundharam, B., & Nandini, D. B. (2022). Oral lesions and periodontal status in diabetics and non-diabetics. Journal of Oral and Maxillofacial Pathology, 26(3), 419. https://doi.org/10.4103/jomfp.jomfp_37_21
- Rogers, R., & Bruce, A. (2004). The tongue in clinical diagnosis. Journal of the European Academy of Dermatology and Venereology, 18(3), 254–259. https://doi.org/10.1111/j.1468-3083.2004.00769.
About the authors

Fernanda Rosenboom is a second-year dental student at University College Cork, where she is completing her Bachelor of Dental Surgery (BDS). She also holds a Bachelor of Science in Medical Sciences from Brock University. For the past three years, Fernanda has worked as a Dental Administrative Assistant at Dr. Peter C. Fritz’s Periodontal Wellness & Implant Surgery in Fonthill, Ontario.

Dr. Peter Fritz is an intrepid life-long, global learner. He leads an extraordinary, collaborative, and empowered team of clinicians, scientists, students, explorers, and artists who work together to innovate the specialty of periodontics and redefine the patient experience, utilizing their heads, hearts, and hands.