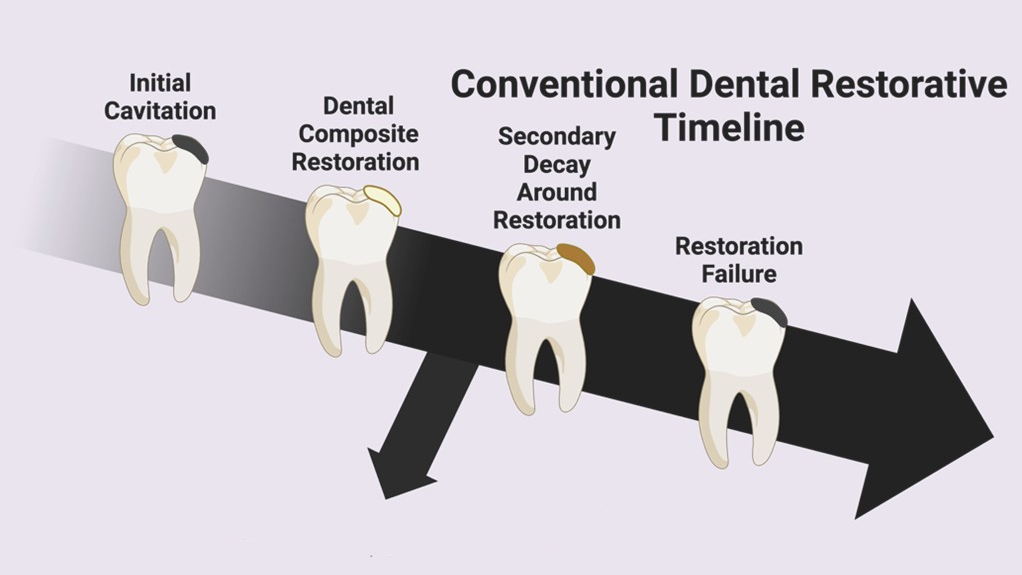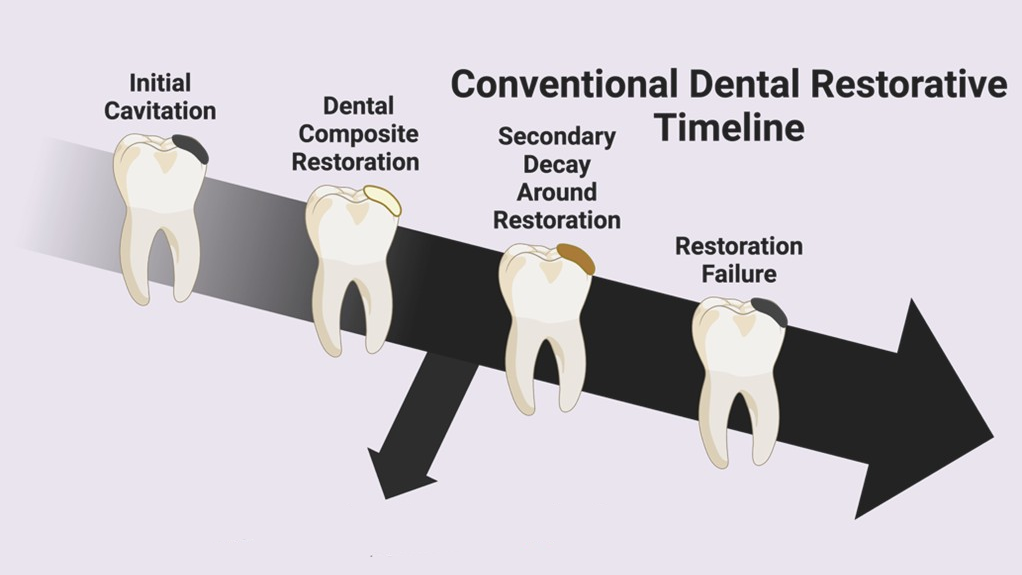
In our search for a life partner, we often seek a union built on strength, stability, and longevity—one that can withstand the test of time. In the world of restorative dentistry, the search is not so different, as we too aim to find the best material to restore tooth structures following the progression of dental decay, which may extend through the life of the patient. Finding this reliable (clinical) partner can feel like the search for “the one”. For decades, dentists have relied on methacrylate (MA) resin-based restorative materials (RBRs) as their go-to partners.1 On the surface, this relationship seems ideal. These materials are aesthetically pleasing, matching the natural colour of teeth, easy to work with, and far safer than their problematic and toxic (no pun intended) predecessor, the mercury-containing amalgam. Better yet, these MA-RBRs do not require invasive undercuts to be retained within the tooth, and instead, have the ability to bond both chemically and micromechanically to tooth structures, forming a connection that should last.
However, despite their widespread popularity, patient relationships with MA-RBRs do not last. The clinical service life of contemporary MA-RBRs is surprisingly short, averaging less than ten years,2,3 with some failing in as little as two.4–6 The two leading causes for these “breakups” are secondary caries and fracture, leaving patients and clinicians in a frustrating cycle of replacement and repair. This high failure rate reveals a fundamental incompatibility, a truth that researchers at the University of Toronto’s Santerre-Finer group have spent over 25 years uncovering. The core issue lies in a “personality” flaw at the very heart of the material’s chemistry. The MA-ester-based monomers which have been the foundation of restorative resins since the 1960s are chemically labile, or “weak” and break down when exposed to the daily stresses of the oral environment, which include bacteria, salivary enzymes, and changes in temperature and pH.7–10 The progressive degradation of the resin network contributes to microleakage at the restorative margins, creating a pathway for bacterial ingress and ultimately causing the relationship with the restorative to fail.
Faced with this recurring heartbreak, our initial impulse was not to end our relationship with MA-RBR materials, but rather to try to fix it. The first strategy was to “shield” the vulnerable aspects of our beloved MA-RBR materials (the ester groups in all MA resin monomers) from harm, in an attempt to repair our problematic partners.11 Technically, this fix involved the addition of fluorine adducts to the MA resin monomers, with the hope that these might make the materials more resilient to the oral environment, essentially creating a protective barrier like Teflon (PTFE), to keep the damaging oral environment out. However, unfortunately for us and our relationship, this fix did not address the core issue. Even though these fluorinated MA chemistries were thoughtfully designed and tested, material degradation persisted and actually compromised other existing desirable properties of MA-RBRs, including mechanical properties. This effort taught us a tough lesson: you cannot mask fundamental incompatibility with surface-level changes and expect a lifelong match.
These disappointing results led to a complete reframing of our search for “the one”. Through some serious soul-searching, we decided that, rather than trying to fix our fundamentally incompatible partners (MA resin monomers), we should focus on finding something completely different. Essentially, we moved from “How can I make this work?” to “What do I actually need in a partner?”. Through careful analysis of both our own and others’ previously failed attempts to move on from MA-RBRs, we applied an engineering approach to develop a systematic framework designed to efficiently vet potential ester-free partners.12 For this, we used a GO/NO-GO decision schema in an attempt to save unnecessary time and investment in relationships (with MA-alternative chemistries) that were doomed from the start. Over the past 5 years, we have used this “speed dating” approach to screen hundreds of potential partners with more than 40 serious candidates for their long-term compatibility potential. Through this methodical screening process, several highly promising MA-alternative candidates emerged, including novel resins (NR) based on non-ester containing acryl monomers.13
However, compatibility isn’t just about first impressions; it also requires meeting the essentials. In this case, that means maintaining critical physical properties such as curing, handling, and mechanical durability which would make NR-RBRs clinically feasible. Early comparisons showed that our NRs could indeed meet the fundamental properties of MA-RBRs, which are prerequisites for any serious commitment to these materials. Moreover, our research has demonstrated the remarkable resilience of NRs when exposed to the various oral stresses that have undermined MA-RBRs in the past. These included salivary, bacterial (Streptococcus mutans), and acidic challenges that traditionally led to rapid material degradation. While MA-based materials often crumbled under pressure, losing almost all structural integrity within a week of these stress tests, our new partner (NR) remains virtually unchanged. Perhaps most importantly, this stability was achieved without sacrificing the qualities that make a clinical relationship work, preserving the fundamental compatibility that clinicians rely on.
The implications of these findings and the potential of NR-RBRs stand to break the traditional failure cycle of contemporary MA-RBRs (Fig. 1). These biostable alternatives represents a fundamental shift in approach, which, to date, has not been achieved and offers the possibility of genuine long-term stability. Long-term stability for clinicians means more non-restorative time to spend with patients. For patients, long-term stability means fewer instances of secondary decay and failed restorations, reducing the economic burden of treatment costs. While current testing has been comprehensive under controlled conditions (including chewing simulation and relevant thermal aging), the true test will come through real-world application over extended use periods before materials based on these new chemistries hit the clinic.
Fig. 1
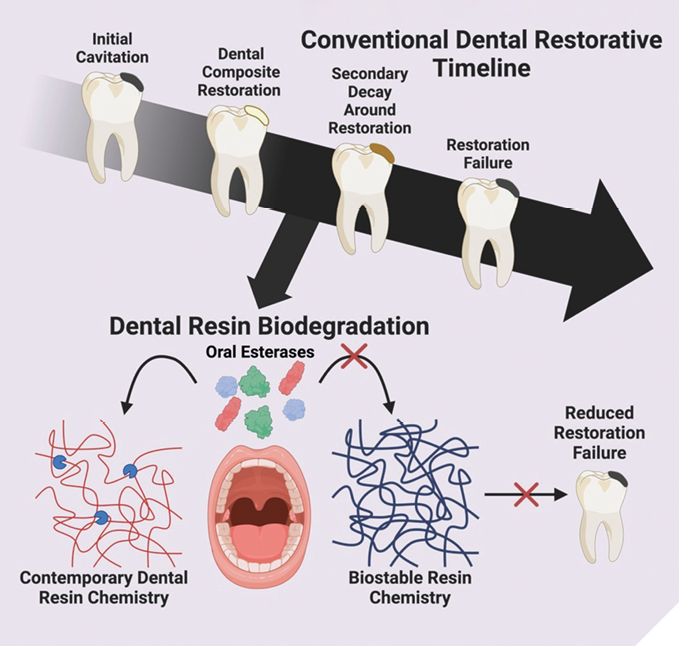
The journey from protecting flawed restorative relationships to finding genuinely compatible clinical partners has been a novel approach. By prioritizing fundamental compatibility over surface-level attraction or attempts to fix inherent flaws, this research at the University of Toronto points to the possibility of truly lasting partnerships. We believe that an engineering approach to finding “the one”, involving systematic evaluation, clearly defined criteria, and a refusal to settle for fundamental incompatibilities, offers a way to break the cycle of failures with MA-RBRs that have long plagued clinicians and patients alike. Sometimes the solution is not to try harder to make the wrong material work, but to have the wisdom to recognize when it is time to search for something completely new. 
Oral Health welcomes this original article.
References
- Ferracane, J. L. Resin Composite – State of the Art. Dent. Mater. 2011, 27 (1), 29–38. https://doi.org/10.1016/j.dental.2010.10.020.
- Kopperud, S. E.; Tveit, A. B.; Gaarden, T.; Sandvik, L.; Espelid, I. Longevity of Posterior Dental Restorations and Reasons for Failure. Eur. J. Oral Sci. 2012, 120 (6), 539–548. https://doi.org/10.1111/eos.12004.
- Kubo, S. Longevity of Resin Composite Restorations. Jpn. Dent. Sci. Rev. 2011, 47 (1), 43–55. https://doi.org/10.1016/j.jdsr.2010.05.002.
- Stewardson, D.; Thornley, P.; Bigg, T.; Bromage, C.; Browne, A.; Cottam, D.; Dalby, D.; Gilmour, J.; Horton, J.; Roberts, E.; Westoby, L.; Dietrich, T.; Burke, T. The Survival of Class V Restorations in General Dental Practice. Part 1, Baseline Data. Br. Dent. J. 2010, 208 (9), E17–E17. https://doi.org/10.1038/sj.bdj.2010.445.
- Stewardson, D. A.; Thornley, P.; Bigg, T.; Bromage, C.; Browne, A.; Cottam, D.; Dalby, D.; Gilmour, J.; Horton, J.; Roberts, E.; Westoby, L.; Creanor, S.; Burke, T. The Survival of Class V Restorations in General Dental Practice. Part 2, Early Failure. Br. Dent. J. 2011, 210 (11), E19–E19. https://doi.org/10.1038/sj.bdj.2011.430.
- Stewardson, D.; Creanor, S.; Thornley, P.; Bigg, T.; Bromage, C.; Browne, A.; Cottam, D.; Dalby, D.; Gilmour, J.; Horton, J.; Roberts, E.; Westoby, L.; Burke, T. The Survival of Class V Restorations in General Dental Practice: Part 3, Five-Year Survival. Br. Dent. J. 2012, 212 (9), E14–E14. https://doi.org/10.1038/sj.bdj.2012.367.
- Montes-G, G. M.; Draughn, R. A. In Vitro Surface Degradation of Composites by Water and Thermal Cycling. Dent. Mater. 1986, 2 (5), 193–197. https://doi.org/10.1016/S0109-5641(86)80012-4.
- Kusuma Yulianto, H. D.; Rinastiti, M.; Cune, M. S.; de Haan-Visser, W.; Atema-Smit, J.; Busscher, H. J.; van der Mei, H. C. Biofilm Composition and Composite Degradation during Intra-Oral Wear. Dent. Mater. 2019, 35 (5), 740–750. https://doi.org/10.1016/j.dental.2019.02.024.
- Münchow, E. A.; Ferreira, A. C. A.; Machado, R. M. M.; Ramos, T. S.; Rodrigues-Junior, S. A.; Zanchi, C. H. Effect of Acidic Solutions on the Surface Degradation of a Micro-Hybrid Composite Resin. Braz. Dent. J. 2014, 25 (4), 321–326. https://doi.org/10.1590/0103-6440201300058.
- Finer, Y.; Santerre, J. P. Salivary Esterase Activity and Its Association with the Biodegradation of Dental Composites. J. Dent. Res. 2004, 83 (1), 22–26. https://doi.org/10.1177/154405910408300105.
- Lagowski, M.; Gouveia, Z.; Yang, M.; Finer, Y.; Santerre, J. P. Synthesis and Challenges of Fluorinated Divinyl Urethane Monomers as a Strategy for Masking Hydrolytic Sensitive Methacrylate Groups in Resin Composites. Dent. Mater. 2024, 40 (10), 1624–1634. https://doi.org/10.1016/j.dental.2024.07.006.
- Gouveia, Z.; Finer, Y.; Santerre, J. P. Towards the Development of Biostable Dental Resin Systems – Design Criteria and Constraints beyond Ester-Free Chemistries. Dent. Mater. 2022, 38 (12), 1827–1840. https://doi.org/10.1016/j.dental.2022.09.016.
- Gouveia, Z.; Finer, Y.; Santerre, J. P. Development of Functional and Hydrolytically Stable Vinyl Monomers as Methacrylate Dental Resin Restorative Alternatives. Adv. Healthc. Mater. 2025, 2403427. https://doi.org/10.1002/adhm.202403427.
About the author

Zach Gouveia (BESc., MESc.) is currently a PhD candidate at the University of Toronto. His core thesis work (under the supervision of Dr. Paul Santerre and Dr. Yoav Finer) has focused on the development of a biostable dental resin system to improve the service life of restorative materials.