For years, dentistry has associated “technology” with the clinical side: digital impressions, imaging upgrades, and new diagnostic tools. Those innovations matter, and they’ve improved care in real ways. But the truth is, the biggest shift happening in dentistry right now isn’t only clinical.
It’s operational.
With DSOs continuing to grow and multi-location dentistry becoming more common, the operational side of dentistry can’t be treated as secondary. Dentistry isn’t just about great clinical care; it’s also about strong systems. The clinics that thrive in today’s environment are the ones that build consistency behind the scenes: scheduling logic, follow-up processes, team workflow, and patient communication that doesn’t fall apart when the day gets busy.
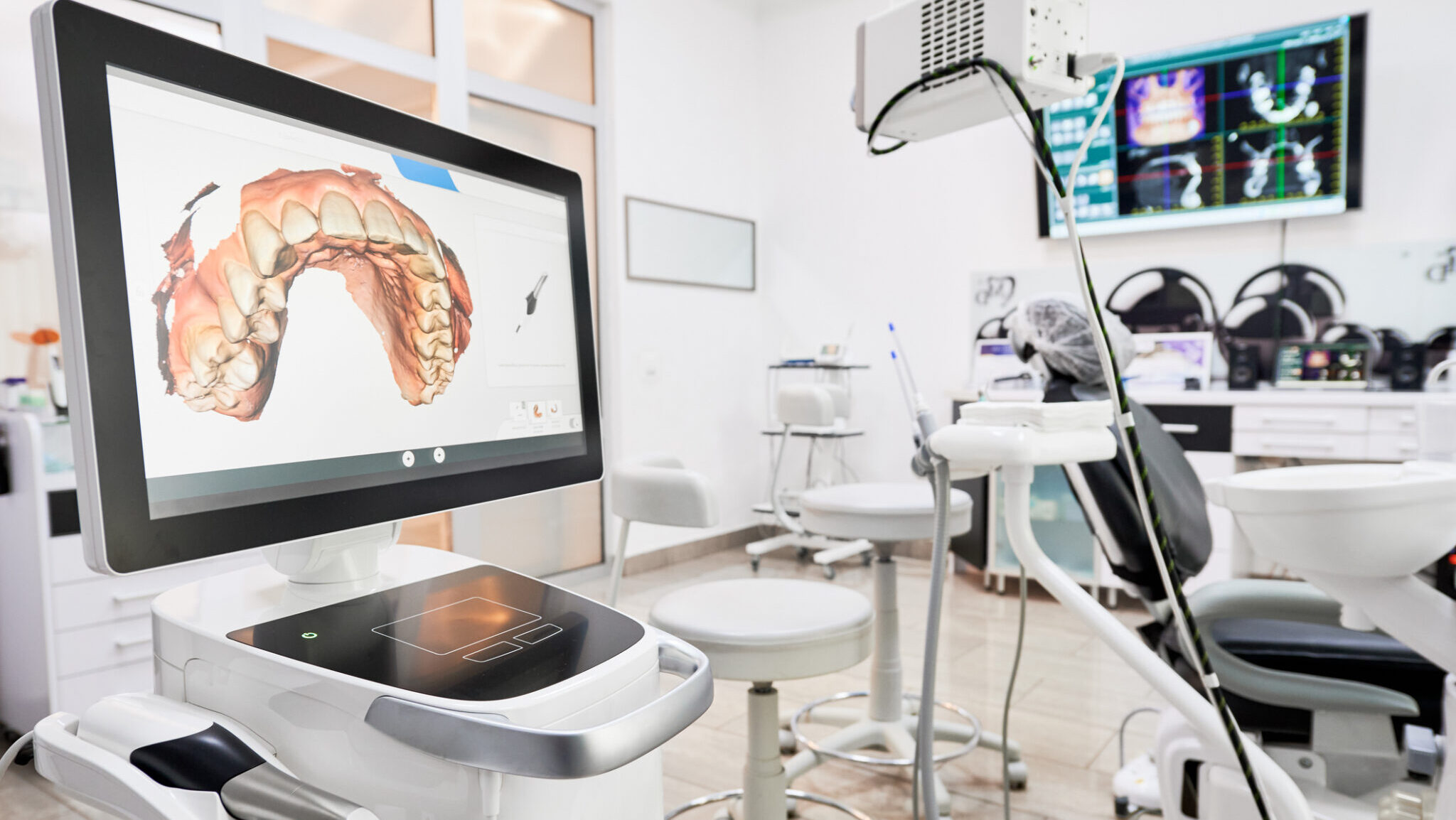
In many ways, that’s where AI is starting to matter most, not as a replacement for people, but as a support layer that helps practices run with more structure, visibility, and stability (Fig. 1).
Fig. 1

As dentistry scales, strong operations become the backbone of consistency, performance, and patient experience.
Dentistry has entered an “operations era”
Most dental teams don’t need to be told that dentistry feels harder to run than it did even a few years ago. Between staffing pressures, rising expectations, and the constant push to stay efficient without sacrificing quality, the day-to-day realities of managing a clinic have changed.
And the workforce strain isn’t just “a feeling.” Statistics Canada’s Survey of Oral Health Care Providers (SOHCP) was designed to collect operational and financial information from practices in Canada, including staffing and vacancies, services offered, and operational challenges.¹ As operations get more complex, access to this kind of data matters, not just for policy decisions, but for practice owners and leaders trying to understand what the market is telling them.
In one recent release, Statistics Canada reported that dentist offices were the most likely to report having at least one staffing or human resources challenge (82%), and difficulty recruiting skilled employees was the most cited challenge (64%).² Independent dental hygienist offices also reported recruiting challenges (50%).²
That kind of pressure changes how a practice runs. When recruiting is difficult and teams are stretched, clinics don’t struggle because care isn’t good, they struggle because the systems behind the care can’t consistently protect the day. A well-intentioned team can still lose momentum if the schedule becomes unpredictable, follow-up becomes inconsistent, and communication becomes reactive.
This is also where DSOs have influenced the industry. Scaling requires repeatable systems, consistent workflows, measurable performance, and clearer operational accountability. Dentistry can remain deeply personal while still being system-driven, and in many cases, strong systems protect the patient experience.
Where AI fits (and where it doesn’t)
AI is often marketed as something futuristic, but most dental teams don’t have time for futuristic. They need practical.
In a real clinic setting, AI is most helpful when it supports the team in simple ways: organizing information, reducing manual admin work, and helping workflows stay consistent even on the busiest days. It’s less about flashy features and more about creating structure and clarity, so fewer things slip through the cracks.
Across industries, the attention on AI is not just hype. McKinsey estimates that generative AI could add the equivalent of $2.6 trillion to $4.4 trillion annually across the use cases they analyzed.³ Dentistry won’t capture that value overnight, but the takeaway is important: AI creates meaningful impact when it improves productivity in everyday workflows, especially the work that consumes time but doesn’t directly improve patient care.
1) Scheduling: The fastest way to lose (or protect) revenue
There’s a reason experienced managers say the schedule is the heartbeat of the practice. A single short-notice cancellation doesn’t just create a gap; it creates a ripple effect:
- Hygiene checks get pushed
- Treatment runs late
- The front desk scrambles
- Production drops
- The team feels behind
Operationally, downtime is one of the most expensive problems because it doesn’t show up as a billable error. It shows up as time that disappears.
What’s interesting is that patients understand how critical access and convenience are. One dataset reported that 71% of patients believe offering same-day or next-day appointments would help reduce no-shows, cancellations, and rescheduling.⁴ That number speaks to a larger shift in patient behaviour: people still want dental care, but they want flexibility and speed, and when they don’t get it, attendance becomes less predictable.
Technology can support scheduling by strengthening consistency in confirmation workflows, improving responsiveness to openings, and reducing the “manual scramble” that often happens when time opens up unexpectedly.
2) Treatment plan follow-up: The revenue clinics don’t realize they’re losing
If you ask most practices what their biggest growth challenge is, many will say new patients. But what’s often missed is the amount of revenue and care that sits inside unscheduled treatment.
This is one of the most common operational breakdowns in dentistry:
- The patient agrees, but doesn’t book
- The day gets busy and follow-up doesn’t happen
- There’s no system to bring that patient back into the pipeline
- Different team members assume someone else is handling it
The difference between a strong practice and a struggling one often isn’t the quality of the treatment plan, it’s the structure behind the follow-up. Clinics that build consistent follow-up systems create better continuity of care, better patient outcomes, and better production stability.
The goal isn’t to pressure patients. It’s to support them with clarity, education, and timely outreach so treatment doesn’t quietly disappear.
3) Patient communication: The best practices don’t leave it to chance
Strong patient communication can’t be improvised. The best practices treat communication like a system, because it affects:
- Trust
- Attendance
- Case acceptance
- Rebooking
- Reviews and reputation
In many clinics, communication becomes reactive: the front desk is moving quickly, messages pile up, and reminders can feel inconsistent depending on who is working. When communication is consistent, the patient journey becomes more predictable, and the overall experience improves.
Technology can help teams maintain consistency, reduce missed touchpoints, and ensure patients receive the information they need, without losing the human tone that defines great dentistry.
4) Workflow support: Less burnout, more accountability
One of the biggest operational problems in dentistry isn’t a lack of talent, it’s overload. Front desk teams are expected to manage phones, walk-ins, confirmations, insurance questions, billing, scheduling, and patient concerns all at once.
When systems are weak, the clinic runs on memory. And when the clinic runs on memory, burnout becomes the default. Strong operations are about reducing mental load, protecting team energy, and creating clarity around what must happen every day for the clinic to run smoothly.
This is where the right tools can make life easier, not by replacing people, but by supporting them so they can focus on the work that truly requires human attention.
5) Why DSOs are leaning into operations and technology faster
DSOs don’t grow by accident. The operational stack behind them is part of what enables scale, and that same thinking is spreading across the industry.
Grand View Research estimates the global dental service organization market was USD 68.16 billion in 2024 and is projected to reach USD 294.34 billion by 2033, growing at a CAGR of 17.67% from 2025 to 2033.5 Regardless of the exact structure in Canada, those growth expectations signal something bigger: multi-location dentistry is expanding, and operational discipline is becoming non-negotiable.
Scaling requires standardization, reporting, accountability, and visibility, without losing culture and patient experience.
Risks, ethics, and leadership oversight
AI is not “plug and play,” especially in a healthcare-adjacent environment. Practices need to think seriously about governance, because the risks are real:
- Privacy and data security
- Unclear accountability
- Poor data quality leading to poor outcomes
- Over-automation that damages trust
For leaders, the best questions to ask before adopting tools are simple:
- What data is being collected, stored, or shared?
- Who can access it, and what protections exist?
- Where does human oversight stay mandatory?
- How will we measure success, and what happens when it underperforms?
The safest, most sustainable approach is using AI as a support layer, not a decision-maker.
Dentistry will always be built on clinical excellence. But the practices that thrive in today’s environment, especially as DSOs grow and multi-location models expand, will be the ones that also master operations.
AI isn’t dentistry’s future. In many clinics, it is already becoming dentistry’s operations layer, the system behind the system. And when it’s implemented responsibly, it can protect what matters most: time, team energy, patient trust, and consistency.
References
- Statistics Canada. Survey of Oral Health Care Providers (SOHCP).https://www.statcan.gc.ca/en/survey/business/5397
- Statistics Canada. The Daily — Survey of Oral Health Care Providers. March 26, 2025. https://www150.statcan.gc.ca/n1/daily-quotidien/250326/dq250326b-eng.htm
- McKinsey & Company. The economic potential of generative AI: The next productivity frontier. 2023.
- Tebra. Stats you need to know about patient cancellations and no-shows.
- Grand View Research. Dental Service Organization Market Report, 2033.
About the author

Julie Hamada is a Chief Operating Officer with deep experience leading dental organizations and growth-stage companies through scale, operational complexity, and organizational change. She oversees operations, marketing, and people leadership with a disciplined, execution-driven approach—translating strategy into structured systems that support sustainable growth and operational excellence. Her work focuses on building scalable infrastructure, strengthening leadership cadence, and aligning teams around clear priorities and accountability.