
Abstract
Clear aligner therapy has significantly transformed orthodontic practice by providing an aesthetic and removable alternative to traditional fixed appliances. Conventional thermoformed aligners, although widely successful, are limited by force degradation, stress relaxation, and deformation under intraoral conditions, affecting treatment predictability. Recent advances in material science, particularly the emergence of 3D-printed shape memory polymers (SMPs), have introduced novel approaches to address these shortcomings. This review explores the chronological development of aligner materials, comparing traditional thermoformed systems with innovative SMP-based technologies such as Graphy’s Tera Harz series and LuxCreo’s ActiveMemory™. While these next-generation materials offer potential improvements in force stability, geometric precision, and biomechanical control, clinical validation remains in early stages. The progression of material innovations and their implications for clinical practice are discussed to guide future research and aligner system selection.
Keywords: clear aligners, orthodontics, shape memory polymers, 3D printing, thermoplastic material
Since the late 1990s, clear aligner therapy has redefined the landscape of orthodontic treatment by offering patients a more discreet and comfortable alternative to fixed appliances.1,2 This shift in clinical approach has been fueled by growing patient demand and a parallel evolution in material science and manufacturing techniques.3-5
Despite their popularity, conventional thermoformed aligners, typically fabricated from polyethylene terephthalate glycol (PETG) or thermoplastic polyurethane (TPU), exhibit material limitations that can compromise treatment outcomes.6 These limitations include force degradation over time,7-9 deformation due to intraoral stress and temperature, and inconsistencies in achieving intended tooth movements, particularly in complex cases.10
To address these challenges, the integration of additive manufacturing and shape memory polymers has emerged as a promising alternative. These advanced materials offer enhanced mechanical behavior, including temperature-triggered shape recovery and improved force sustainability.11 The transition from traditional vacuum thermoforming to direct 3D printing represents a paradigm shift in aligner fabrication, with the potential to optimize both clinical outcomes and manufacturing efficiency.12,13
The evolution of aligner materials can be categorized into several distinct phases, beginning with basic single-layer thermoplastics, progressing to multi-layer composites, and most recently, encompassing 3D-printed shape memory polymers featuring dual activation mechanisms14,15 (Fig. 1).
Fig. 1
Evolution of clear aligner materials
Thermoformed Aligners (1997–2010): The initial era of clear aligners began with the introduction of Invisalign in 1997, which utilized single-layer PETG sheets shaped through vacuum thermoforming.16 These early materials were transparent and easily processed but displayed significant stress relaxation, limited elastic recovery, and difficulty in achieving controlled force systems.
By the early 2000s, the development of multi-layer composites sought to enhance mechanical performance.17 Typically consisting of three layers, with the outer layers providing rigidity and the inner layer offering resilience, these materials improved elastic recovery and reduced deformation. TPU and modified PETG became standard, and a uniform aligner thickness of approximately 0.75 mm was adopted to optimize force delivery and anatomical fit. Although these refinements contributed to more predictable outcomes, fundamental issues such as time-dependent force decay and limited control over complex tooth movements remained unresolved.
Shape memory polymers (2018–2022): A significant advancement occurred with the introduction of photocurable shape memory polymers (SMPs) for orthodontic applications.18-20 These materials possess the ability to return to a pre-programmed shape upon exposure to specific thermal conditions, enabling aligners to recover their original geometry even after intraoral deformation.
In 2020, Graphy Inc. introduced the first commercially available 3D-printable SMP aligner material, TC-85. This innovation marked a departure from traditional thermoforming, allowing for direct digital fabrication of aligners with controlled thickness and geometry. The company subsequently develop the TA-28 polymer to provide further improvements in clinical efficiency and patient comfort. The naming suggests optimal shape memory activation near intraoral temperature thresholds, possibly around 28°C.
Initial clinical applications of these materials were limited to case reports and pilot studies, with no prospective data available during this phase.13,21 Proper post-curing protocols were identified as essential to achieve the desired mechanical properties and shape recovery behavior.22,23 Reports described a light, continuous force delivery, consistent with biologically favorable tooth movement (Fig. 2).
Fig. 2
Active memory polymers (2022–Present): The most recent generation of aligner materials incorporates dual activation mechanisms, combining mechanical programming during manufacturing with temperature-driven reactivation during daily intraoral use. LuxCreo’s ActiveMemory™ exemplifies this category, integrating a dual-mode system intended to deliver continuous, predictable force while maintaining geometric stability throughout the treatment cycle.
These materials are designed to address stress relaxation more effectively than conventional thermoformed aligners, enhancing force sustainability, engaging undercuts and potentially reducing reliance on bonded attachments. Through the improved engagement in dental undercuts and more efficient force distribution, active memory polymers aim to extend wear intervals and improve patient comfort. These polymers are reactivated daily using a warm water bath (60 degrees Celsius) to potentially restore them to their original shape and reduce stress relaxation significantly when compared to thermoformed (Fig. 3).
Fig. 3
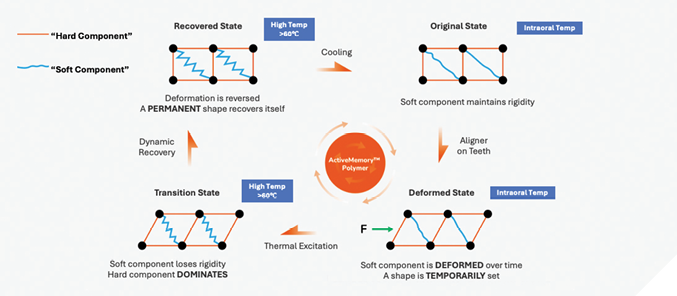
Comparative timeline of material evolution
A chronological overview of aligner material development highlights the incremental improvements across successive generations. From 1997 to 2010, thermoformed PETG and TPU materials dominated, offering basic elastic performance with significant stress relaxation and creep. From 2018 onward, shape memory polymers emerged, offering temperature-activated recovery and early clinical applications. Since 2022, dual-activation systems have introduced mechanical and thermal reactivation strategies, supported by emerging clinical reports (Table 1).
Table 1: Timeline of clear aligner materials introduction
| Period | Technology | Key Characteristics | Clinical Status |
| 1997 – 2010 | Thermoformed PETG/TPU | Basic elastic deformation | Extensively validated |
| 2010 – 2018 | SMA Integration Attempts | Limited hybrid approaches | Minimal adoption |
| 2018 – 2022 | Shape Memory Polymers | Temperature-activated recovery | Early clinical validation |
| 22 – Present | Active Memory Polymers | Dual-activation mechanisms | Emerging clinical evidence |
Thermoformed aligner systems
Thermoformed aligners remain widely used due to their long history of clinical success and established production workflows. Their advantages include extensive peer-reviewed validation, cost-effectiveness, and global regulatory approval. The manufacturing process is mature and reproducible, supporting consistent material quality and supply chain efficiency.24 They are cost effective and predictable.
However, these aligners are affected by mechanical behavior changes under oral conditions. Studies have shown that aligners experience significant force reduction, often between 50 to 70 percent, within the first day of wear. This force decay results from material fatigue, creep, and thermal softening, which may impact treatment efficacy.25 Furthermore, the precision of certain tooth movements, such as rotation, extrusion, and torque, can vary based on case complexity, leading to potential refinements or overcorrections.26,27
Due to geometric adaptation Extended wear may also result in deformation, reduced fit, and reduced efficiency, potentially affecting resulting in more refinements or incomplete treatment.9,28 Extended wear may result in visible material changes and reduced retention, potentially impacting patient compliance in some cases29 (Fig. 4).
Fig. 4
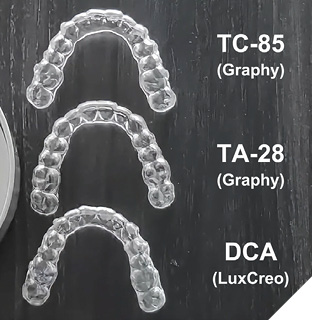
Emerging shape memory technologies
Shape Memory Polymers : Graphy Tera Harz Systems: Graphy Inc. has pioneered the use of photocurable30 polymers for direct 3D printing of clear aligners based on several research projects reporting on the shape memory of these polymers. TC-85, the company’s first direct printed material, was designed to overcome the mechanical limitations of conventional thermoplastics by offering enhanced elastic behavior at intraoral temperatures. Other benefits consisted of the elimination of several time-consuming steps such as model printing and thermoforming procedures.31 An image of the aligners on the build plate with supports offers a glimpse into this streamlined workflow (Fig. 5). Enhanced precision, reduced manufacturing waste, and customizable aligners are cited as improvements over thermoformed aligners.32
Fig. 5

Subsequent advancements led to the development of TA-28, which aimed to increase patient comfort and treatment efficiency. Both materials exhibit a controlled glass transition temperature that facilitates shape recovery at physiological temperatures. Dynamic mechanical analysis has demonstrated superior thermo-mechanical and viscoelastic properties, including improved elastic modulus, shape retention, and resistance to creep. The numerical designation “28” may refer to optimized performance characteristics at or around 28°C, which represents a critical temperature threshold for shape memory activation in clinical applications.
The digital manufacturing approach allows for precise control over aligner thickness and geometry, reducing material waste and eliminating the need for vacuum forming. The properties of these materials can also be tuned during the printing and post-curing process, making the system highly customizable to individual treatment needs.33
LuxCreo ActiveMemory™ Technology
LuxCreo’s ActiveMemory™ system integrates a dual process of mechanical programming and daily thermal reactivation, designed to restore structural integrity under intraoral conditions while providing controlled flexibility for patient comfort and ease of insertion/removal, aiming to provide sustainable orthodontic force across the wear cycle. This dual-activation system supports continuous shape restoration and geometric recovery under intraoral stress. The combination of mechanical and thermal activation mechanisms aims to provide sustained force systems optimized for biological tooth movement
The material is designed to retain structural integrity while allowing sufficient flexibility for insertion and removal. By maintaining a constant force level, it potentially reduces the need for overcorrection and frequent aligner changes. This system may also support longer wear intervals, customized activation schedules, and broader treatment applications.
Although these theoretical benefits are compelling, robust clinical studies are required to assess their impact in real-world practice and to compare their efficacy against thermoformed systems across a variety of malocclusions.
Theoretical advantages of advanced polymer systems: Shape memory polymer technologies, including ActiveMemory™ and Graphy systems,34 propose several theoretical advantages over conventional aligner materials. Their intrinsic shape memory properties allow aligners to revert toward their original prescribed geometry, potentially reducing stress relaxation and creep.35 Furthermore, the temperature-responsive behavior characteristic of these polymers will enable customizable force activation and reactivation, enhancing clinical control and flexibility. Direct 3D printing processes, integral to these systems, facilitate greater geometric recovery. Additionally, ActiveMemory™, integrate dual activation mechanisms, combining mechanical and thermal stimuli which may result in superior and more finely tuned orthodontic force control compared to traditional aligner materials.
Despite their theoretical advantages, shape memory polymer aligners face several considerations. There is currently limited long-term clinical data available compared to the extensive evidence supporting traditional thermoformed aligners. Additionally, the specialized 3D printing technologies and materials used for these polymers may increase overall treatment costs. The scalability of manufacturing also poses challenges, as production capacity and quality control systems for directly printed aligners are still evolving. Moreover, newer materials may require additional regulatory validation processes before achieving widespread clinical acceptance. Lastly, biocompatibility and safety remain important areas for ongoing assessment, particularly regarding long-term compatibility in the oral environment, potential material degradation, byproduct formation, and patient sensitivity or allergic responses.36,37 (Figs. 6A-B)
Fig. 6A
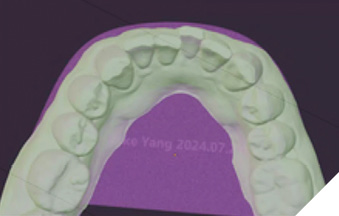
Fig. 6B
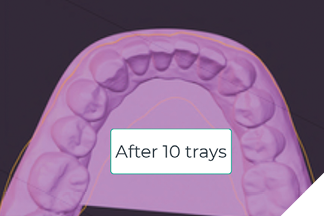
Clinical evidence and research directions
Thermoformed aligners are supported by extensive clinical research, including systematic reviews and long-term outcome studies.17 These aligners have demonstrated effectiveness in a wide range of treatment scenarios and are considered reliable for predictable tooth movement in a wide range of cases.2,6
In contrast, shape memory polymer systems, while technologically advanced, are still in the early phases of clinical validation. Preliminary data from case reports and in vitro studies indicate favorable mechanical properties and force consistency. However, comprehensive trials are necessary to determine their long-term effectiveness, safety, toxicity and patient satisfaction compared to traditional systems.
Future research should prioritize randomized controlled trials comparing treatment efficiency, biomechanical accuracy, and patient-reported outcomes between SMPs and thermoformed aligners. Additional investigations are needed into the biocompatibility and degradation behavior of photocurable SMPs in the oral environment, as well as their economic feasibility and manufacturing scalability (Fig. 7).
Fig. 7A
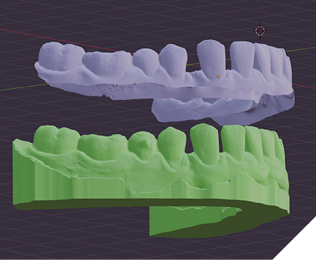
Fig. 7B
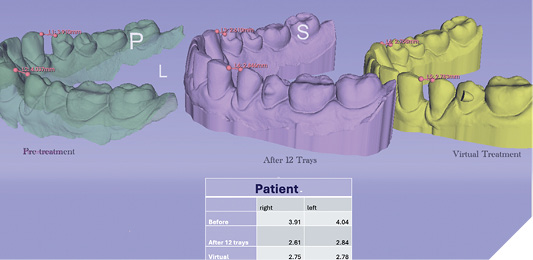
Conclusion
Clear aligner materials have undergone substantial innovation over the past two decades. While thermoformed systems continue to offer dependable outcomes and manufacturing ease, recent advances in 3D-printed shape memory polymers present new possibilities for orthodontic treatment. Technologies such as Graphy’s Tera Harz and LuxCreo’s ActiveMemory™ show potential benefits in force stability, geometric accuracy, and reduced reliance on attachments. Despite these advantages, clinical adoption should be guided by high-quality evidence, patient needs, and case complexity. Continued research is essential to establish best practices for material selection and to maximize the therapeutic potential of these evolving systems. 
Oral Health welcomes this original article.
References
- Djeu, G., C. Shelton, and A. Maganzini, Outcome assessment of Invisalign and traditional orthodontic treatment compared with the American Board of Orthodontics objective grading system. Am J Orthod Dentofacial Orthop, 2005. 128(3): p. 292-8; discussion 298.
- Rossini, G., et al., Efficacy of clear aligners in controlling orthodontic tooth movement: a systematic review. The Angle Orthodontist, 2015. 85(5): p. 881-889.
- Putrino, A., E. Barbato, and G. Galluccio, Clear Aligners: Between Evolution and Efficiency-A Scoping Review. Int J Environ Res Public Health, 2021. 18(6).
- Ellis, C.P., Invisalign and changing relationships. Am J Orthod Dentofacial Orthop, 2004. 126(1): p. 20A-21A; author reply 21A.
- Weir, T., Clear aligners in orthodontic treatment. Aust Dent J, 2017. 62 Suppl 1: p. 58-62.
- Castroflorio, T., S. Parrini, and G. Rossini, Aligner biomechanics: Where we are now and where we are heading for. J World Fed Orthod, 2024. 13(2): p. 57-64.
- Albertini, P., et al., Stress relaxation properties of five orthodontic aligner materials: a 14-day in-vitro study. Bioengineering, 2022. 9(8): p. 349.
- Lombardo, L., et al., Stress relaxation properties of four orthodontic aligner materials: A 24-hour in vitro study. Angle Orthod, 2017. 87(1): p. 11-18.
- Hahn, W., et al., Influence of thermoplastic appliance thickness on the magnitude of force delivered to a maxillary central incisor during tipping. Am J Orthod Dentofacial Orthop, 2009. 136(1): p. 12.e1-7; discussion 12-3.
- Bollen, A.M., et al., Activation time and material stiffness of sequential removable orthodontic appliances. Part 1: Ability to complete treatment. Am J Orthod Dentofacial Orthop, 2003. 124(5): p. 496-501.
- Kwon, J.S., et al., Force delivery properties of thermoplastic orthodontic materials. Am J Orthod Dentofacial Orthop, 2008. 133(2): p. 228-34; quiz 328.e1.
- Maspero, C., et al., Correlation between Dental Vestibular-Palatal Inclination and Alveolar Bone Remodeling after Orthodontic Treatment: A CBCT Analysis. Materials (Basel), 2019. 12(24).
- Tartaglia, G.M., et al., Direct 3D Printing of Clear Orthodontic Aligners: Current State and Future Possibilities. Materials (Basel), 2021. 14(7).
- Goracci, C., et al., Clinically Relevant Properties of 3D Printable Materials for Intraoral Use in Orthodontics: A Critical Review of the Literature, in Materials (Basel). 2023: Switzerland.
- Narongdej, P., et al., Advancements in clear aligner fabrication: a comprehensive review of direct-3D printing technologies. Polymers, 2024. 16(3): p. 371.
- Wong, B.H., Invisalign A to Z. Am J Orthod Dentofacial Orthop, 2002. 121(5): p. 540-1.
- Jia, L., et al., Efficacy of various multi-layers of orthodontic clear aligners: a simulated study. Comput Methods Biomech Biomed Engin, 2022. 25(15): p. 1710-1721.
- Bichu, Y.M., et al., Advances in orthodontic clear aligner materials, in Bioact Mater. 2023, © 2022 The Authors.: China. p. 384-403.
- Atta, I., et al., Physiochemical and mechanical characterisation of orthodontic 3D printed aligner material made of shape memory polymers (4D aligner material). J Mech Behav Biomed Mater, 2024. 150: p. 106337.
- Alkhamees, A., The new additive era of orthodontics: 3D-printed aligners and shape memory polymers-the latest trend-and their environmental implications. J Orthod Sci, 2024. 13: p. 55.
- Knode, V., et al., Directly printed aligner therapy: A 12-month evaluation of application and effectiveness. American Journal of Orthodontics and Dentofacial Orthopedics, 2024.
- Jindal, P., et al., Mechanical and geometric properties of thermoformed and 3D printed clear dental aligners. Am J Orthod Dentofacial Orthop, 2019. 156(5): p. 694-701.
- Jindal, P., et al., Mechanical and geometric properties of thermoformed and 3D printed clear dental aligners. American Journal of Orthodontics and Dentofacial Orthopedics, 2019. 156(5): p. 694-701.
- Schuster, S., et al., Structural conformation and leaching from in vitro aged and retrieved Invisalign appliances. Am J Orthod Dentofacial Orthop, 2004. 126(6): p. 725-8.
- Iliadi, A., D. Koletsi, and T. Eliades, Forces and moments generated by aligner-type appliances for orthodontic tooth movement: A systematic review and meta-analysis. Orthod Craniofac Res, 2019. 22(4): p. 248-258.
- Kohda, N., et al., Effects of mechanical properties of thermoplastic materials on the initial force of thermoplastic appliances. Angle Orthod, 2013. 83(3): p. 476-83.
- Lyu, X., et al., Biomechanical effects of clear aligners with different thicknesses and gingival-margin morphology for appliance design optimization. Am J Orthod Dentofacial Orthop, 2023. 164(2): p. 239-252.
- Haouili, N., et al., Has Invisalign improved? A prospective follow-up study on the efficacy of tooth movement with Invisalign. Am J Orthod Dentofacial Orthop, 2020. 158(3): p. 420-425.
- Eliades, T. and G. Eliades, Intraoral ageing of aligners and attachments: Adverse effects on clinical efficiency and release of biologically-active compounds. Korean J Orthod, 2024. 54(4): p. 199-209.
- Gunes, S.I. and S.C. Jana, Shape memory polymers and their nanocomposites: a review of science and technology of new multifunctional materials. J Nanosci Nanotechnol, 2008. 8(4): p. 1616-37.
- Kim, K.B., et al., Direct printing of clear aligners
- Force profile assessment of direct-printed aligners versus thermoformed aligners and the effects of non-engaged surface patterns, in J Clin Orthod. 2023, © 2022. The Author(s). United States
- Germany. p. 450-458.
- Rajasekaran, A. and P.K. Chaudhari, Integrated manufacturing of direct 3D-printed clear aligners. Frontiers in dental medicine, 2023. 3: p. 1089627.
- Panayi, N., J.-Y. Cha, and K.B. Kim. 3D Printed Aligners: material science, workflow and Clinical applications. in Seminars in Orthodontics. 2023. Elsevier.
- Lee, S.Y., et al., Thermo-mechanical properties of 3D printed photocurable shape memory resin for clear aligners. Scientific reports, 2022. 12(1): p. 6246.
- Sharif, M., et al., Force system of 3D-printed orthodontic aligners made of shape memory polymers: an in vitro study. Virtual and Physical Prototyping, 2024. 19(1): p. e2361857.
- Iodice, G., et al., Effect of post-printing curing time on cytotoxicity of direct printed aligners: A pilot study. Orthod Craniofac Res, 2024. 27 Suppl 2: p. 141-146.
- Ferreira, M., et al., Do Clear Aligners Release Toxic Chemicals?-A Systematic Review. J Funct Biomater, 2025. 16(5).
About the author

Dr. Jean-Marc Retrouvey is a Senior Lecturer at Baylor College of Medicine.
