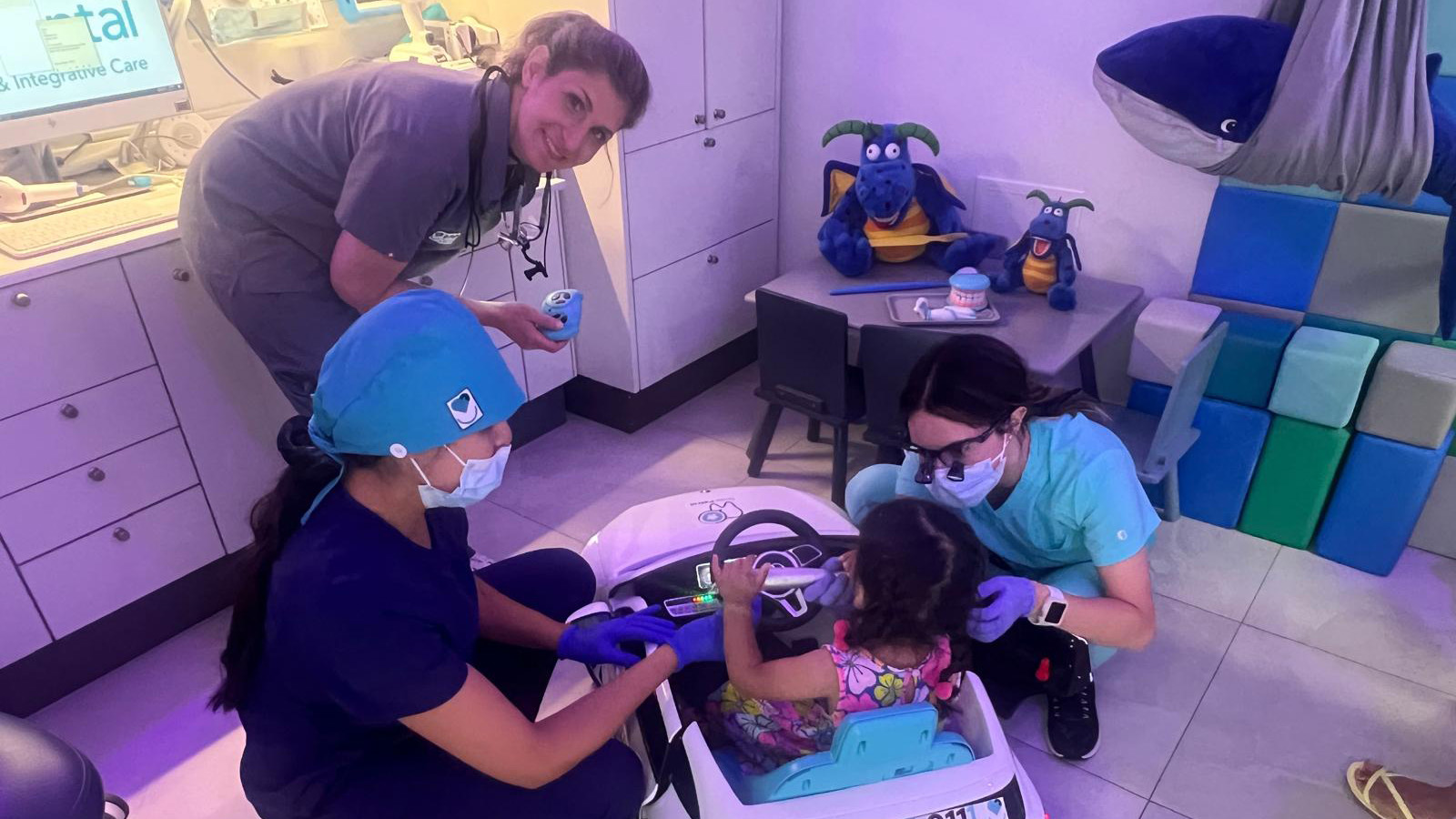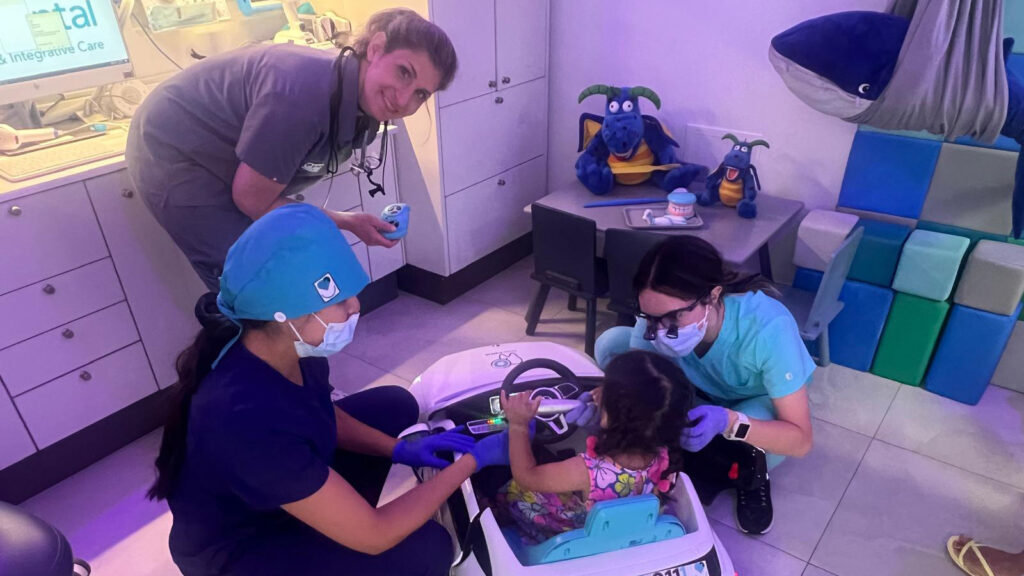
One morning in February, Dr. Salome Lomlomdjian and her team cleared their Mississauga clinic so an 11-year-old patient, Max, could receive treatment in a calm, controlled setting — reducing the risk of him becoming overwhelmed or dysregulated.
For Max’s mother, Maria Garito, the level of preparation stood in sharp contrast to the barriers she had faced elsewhere while seeking dental care for her son, who has profound nonverbal autism. At one specialized clinic, she said, the wait was 12 months. Hospital-based care can also take anywhere from six to 12 months.
“The energy and empathy in the room made such a difference,” Garito said. “They treated Max with patience and respect, and for the first time we felt like we were truly understood.”
Founded in 2022, In Path Dental was created to provide inclusive care for patients with accessibility needs, using an empathy-driven model where storytelling and patient-centred preparation are central to treatment.
Garito said she first learned about the clinic through a CBC News story and a local autism parent support group.
“We are creating something that doesn’t exist. This is not a regular dental practice,” Lomlomdjian said.
“There’s no training in Canada to create a specialty in special care dentistry,” she added, pointing to a broader gap in structured training pathways. Special care dentistry is not currently a formally recognized specialty in Canada.

While the clinic operates as a general practice, it is designed to expand access for patients with conditions such as autism spectrum disorder, sensory processing disorder, Down syndrome, Alzheimer’s disease, Parkinson’s disease, dental anxiety, and other mental, intellectual and physical disabilities.
“The goal in the practice is always to avoid sedation as much as possible,” Lomlomdjian said. After all, she uses communication techniques, when possible, to reduce reliance on sedation when managing behavioural challenges.
The clinic itself is designed around sensory needs, with sounds, colours and layout carefully considered to minimize overstimulation. Sensory-adapted strategies are also used in the operatory.
“These patients require behavioural management. Many are scared. Some don’t want to sit in the chair or approach the panoramic machine,” she said.
To address this, the clinic uses storytelling to demystify equipment — sometimes referring to the panoramic machine as a “spaceship” — and walks patients through each step of the process.
Parents are actively involved, helping prepare their child at home and sometimes staying present during care. Toys, tablets and step-by-step guidance are used to build familiarity and trust.
Each case is approached individually. For Max, Lomlomdjian’s team gathered detailed information in advance and coordinated closely with the anesthesiologist.
“They prepared for every possibility — taking his measurements, ensuring the equipment and medications were ready, and planning how to respond if something unexpected happened,” Garito said. “When we arrived, the entire team was ready.”
Following treatment — which included extractions of infected teeth, treatment of a severe abscess, extensive cleaning and preventive care — Max’s parents reported a significant reduction in aggressive and self-injurious behaviour linked to his untreated dental condition. His sleep also improved.
“As you know, he couldn’t tell us he was in pain, especially with his high pain tolerance,” Garito added.

Persistent gaps in access
People with disabilities continue to face significant barriers in accessing care. A Canadian study published in Disability and Health Journal found they are more than four times as likely to report unmet health-care needs compared with those without disabilities.
“These constraints in supply meet rising need, creating persistent queues,” said Dr. Mario Brondani, a professor and chair of the Division of Dental Public Health at the University of British Columbia.
“Data show long waits across specialty care, and dentistry requiring hospital time competes for scarce operating room resources,” he said. “Few clinics are configured for complex disability care — in terms of space, equipment, sedation access and trained teams.”
Most Canadians rely on private insurance for dental care. While the federal Canadian Dental Care Plan (CDCP), launched in 2023, is expected to improve affordability for uninsured Canadians, eligibility is tied to tax filing.
Brondani said participation among providers may still be limited for complex cases if reimbursement does not reflect the time and resources required.
To read Brondani’s full analysis, see: Why long waits for specialized dental care persist — and what could ease the bottleneck
Related: CDCP ends 2025 with a milestone — but challenges persist
Demand is growing
Against this backdrop, demand for Lomlomdjian’s model continues to grow, with patients travelling from across Ontario and beyond.
“The office is growing, and more complex patients are coming from different parts of the province and even other provinces,” she said. “As complexity increases, the system has to constantly adapt.”
Rethinking care delivery
A key challenge lies in diagnostics, particularly X-rays, which can be difficult for patients with sensory sensitivities or behavioural challenges.
Unlike conventional approaches, Lomlomdjian’s team keeps caregivers in the room during imaging, reinforcing positive cues.
“Some patients come to us after negative experiences where they were restrained or held down,” she said. “Those experiences can create lasting trauma.”
In some cases, multiple visits are required. A single appointment may be dedicated solely to completing a panoramic X-ray before treatment can proceed.
Financial pressures and sacrifice
Despite growing demand, scaling the model presents significant challenges.
“I know some pediatric offices incorporate sensory elements into their spaces, but it’s not just about creating a sensory-friendly environment on paper,” Lomlomdjian said. “Training and hiring the right people is a major part of it.”
“The general fee guide does not reflect the time, complexity and level of care required,” she said. “In other practices, appointments are quick. Here, everything takes longer — and that’s the challenge.”
The clinic also faced setbacks during construction when a contractor disappeared with a significant portion of the budget.
“We lost everything — the entire budget was gone,” she said.
CIBC later approved additional financing, allowing the project to move forward. The clinic ultimately opened with two loans instead of one.
Financial pressures extend to families as well. Max’s treatment cost $5,500 out of pocket.
“We were fortunate enough to be able to do that,” Garito said. “You’re paying for the anesthesiologist, additional supports and the procedures themselves.”
But the cost — both financial and emotional — has been significant for Garito, who left her 20-year career as a high school teacher to care for her son full time.
“He’s at home with me 24/7. There’s no funding for respite,” she said. “It’s very easy to feel like you’re one paycheque away from being homeless.”
Related: The senior-friendly dental office environment: How and why it is essential
Related: Study links periodontal bacterium to multiple sclerosis disability severity
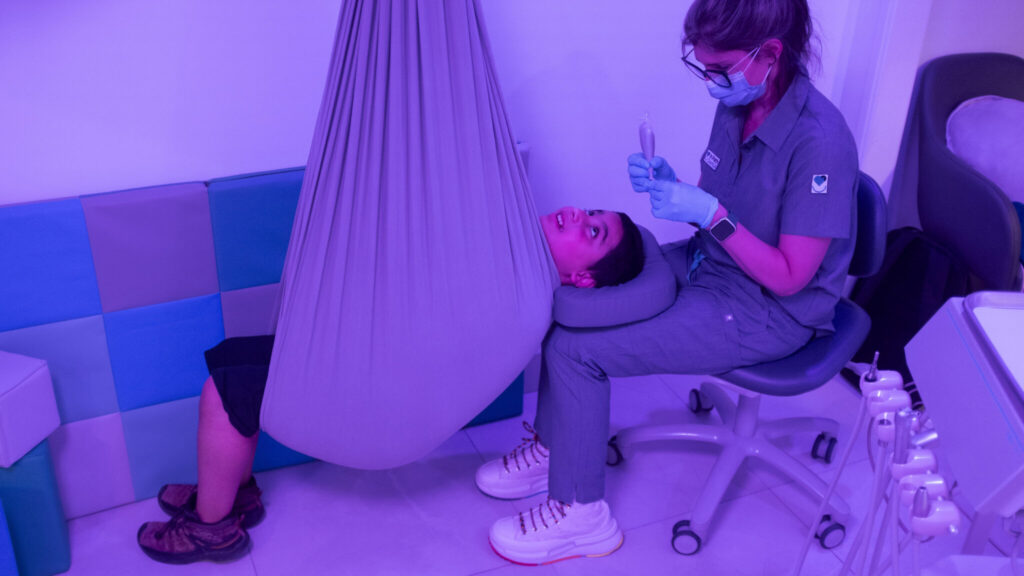
A foundation in empathy
When asked how her approach developed, Lomlomdjian reflected on her childhood in Argentina, recalling a daycare friend with special health-care needs who was often isolated.
“Nobody would play with her,” she said. “She was nonverbal, and everything was a challenge. We became really good friends.”
Later, living in different countries and languages — from Montreal to Brazil — the dentist said she came to see communication as something deeper.
“I communicate with my patients or people in general by energy,” she said.
That experience shaped her approach to inclusive care.
“We don’t say no,” she said. “Just because a patient has special health-care needs doesn’t mean they should receive anything less than the same standard of care.”
Lomlomdjian’s approach is felt by families like Garito’s.
“We don’t have enough people willing to take that chance,” she said. “It’s easier — and I hate to say this — but it’s easier to just see neurotypical children, in and out.”
“To me, that’s what justice looks like. It’s about removing barriers for people.”